Ghanshyam Yadav, MD*, Chandra Sekhar Pradhan**, Surendra Kumar Gupta**, Gaurav Jain, MD, PDCC***, Sandeep Khuba, MD, PDCC*, Dinesh Kumar Singh, MD****
*Assistant Professor, **Junior resident, ***Senior resident, ****Professor and Head.
Department of Anaesthesiology, Sir Sunder Lal Hospital, Institute of Medical Sciences, BHU, Varanasi, 221005, UP, India.
Correspondence: Dr Ghanshyam Yadav, Assistant Professor, Department of Anaesthesiology, Sir Sunder Lal Hospital, Institute of Medical Sciences, BHU, Varanasi 221005,UP (India); Phone: +91-9838894169; Fax: 05422300285; E mail: ghanshyamx@rediffmail.com
ABSTRACT
Objectives: This study was conducted to compare the sedative efficacy of bupivacaine 0.5% with lignocaine 2% plus adrenaline in epidural anaesthesia by using BIS monitor.
Study design: A randomized, double blind study.
Methodology: Sixty patients, ASA physical status I or II, of age group 20-65 yrs, undergoing elective gynaecological surgery under epidural anaesthesia, were randomly but equally placed into two groups (group-B and group-L). Patients received (2ml/segment) bupivacaine 0.5% or lignocaine 2% with adrenaline in group-B and group-L respectively, to achieve a sensory block up to T8 level. After confirmation of sensory blockade, propofol infusion was started at a rate of 100 µg/kg/min to get a BIS value of ≤ 80 and the time was measured (onset time). Surgery was allowed to start immediately after the onset time. Propofol infusion was titrated to maintain the BIS value at 60-80. Infusion was stopped at the end of surgery. The time taken to reach the BIS of≥90 was recorded as ‘recovery time’. The amount of propofol consumed for onset of sedation and total amount consumed during the surgery were noted and compared.
Results: There was no significant difference regarding demographic data and onset time in both groups (P>0.05). Recovery time was significantly prolonged in group-B than group-L 5.57+1.25 min and 4.38+0.94 min respectively (P<0.05). Dose of propofol consumed for onset of sedation was significantly low in group-B than group-L, 17.13+4.22 mg vs. 27.77+8.39 mg respectively (P<0.05). Total amount of propofol consumed was also significantly low in group-B than group-L, 140.33+34.59 vs. 184.80+38.21 respectively (P<0.05).
Conclusion: We conclude that epidural block with 0.5% bupivacaine is associated with less propofol consumption as compared with 2% lignocaine with adrenaline to maintain BIS 60-80 and hence is more effective.
Key words: BIS; Bupivacaine; Lignocaine with adrenaline; Propofol; Onset time; Recovery time.
CITATION: Yadav G, Pradhan CS, Gupta SK, Jain G, Khuba S, Singh DK. Comparison of sedative efficacy of epidural bupivacaine 0.5% with lignocaine 2% plus adrenaline by measuring BIS guided propofol requirement in gynaecological surgery. Anaesth Pain & Intensive Care 2012;16(1):13-17.
INTRODUCTION
Epidural anaesthesia is a widely used method and may be associated with stress, anxiety and even intra-operative discomfort. When using sedative medication as a part of regional anaesthesia technique, the anaesthesiologists attempt to titrate the drug to optimize patient comfort while maintaining cardio respiratory stability and intact protective reflexes.1 Among all available sedative agents propofol provides rapid recovery and faster return of cognitive function.2
There are many ways to monitor the depth of sedation like observing clinical parameters, Ramsay Sedation Scale (RSS), Visual Analogue Scale (VAS), Sedation Agitation Scale (SAS) or Motor Activity Assessment Scale (MAAS). Although these methods are documented to be valid and reliable, 3 but they are prone to subjective bias. The BIS (Bispectral Index) monitor processes a modified EEG (electroencephalogram) to assess the hypnotic effect of sedatives and anaesthetics, replacing the reliance on physiologic variables for determining the depth of anesthesia.4
Various studies have been carried out to compare the efficacy of two local anaesthetics (0.5%bupivacaine and 2% lignocaine with adrenaline) in reducing propofol requirement, during epidural anaesthesia for gynaecological surgery.
METHODOLOGY
After approval from the institutional ethical committee and written informed consent from the patients, this randomised, double blind study was conducted in Department of Anaesthesiology, Sir Sunder Lal Hospital, Institute of Medical Sciences, BHU, Varanasi, UP (India) from January 2010 to January 2012. Sixty patients, aged between 20-60 yrs, ASA physical status I and II, undergoing elective gynaecological operations under epidural anaesthesia were enrolled in the study. Participants to this study were explained about the anaesthetic procedure at the preanesthesia evaluation visit. Patient refusal, a history suggestive of hypersensitivity to bupivacaine, lignocaine or propofol, known history of alcohol and drug abuse, hypovolumia, severe respiratory disease, neurological or psychiatric illness, hypertension, hypotension, valvular heart disease, bleeding disorders, obesity (BMI>30), local skin infection at L1-S1 and pregnant women were excluded from this study.
Power analysis (alpha=0.05 and beta = 0.01) suggest that a sample size of 18 patient per group was needed to detect 30% decrease in propofol requirements. We enrolled 30 patients in each group for any drop out at any stage.
The patients were randomized into two groups, group-B and group-L, of 30 each, by computer generated random numbers. Patients received epidural (2 ml/segment) 0.5% bupivacaine or 2% lignocaine with adrenaline in group-B and group-L respectively. All participants were premedicated with oral alprazolam 0.5mg on the evening and in the morning 2 hr before the surgery. All patients were kept nil per oral for solid food 8 hrs and clear liquid for 2 hrs. Intravenous (IV) access was established using an 18 gauge cannula in nondominant hand. After establishing IV access patients were connected to pulse oximeter, non-invasive blood pressure (NIBP), electrocardiograph (ECG) monitor. All patients were preloaded with ringer lactate 10 ml/kg over 15 min. With all aseptic precautions, skin was cleaned and draped in lateral decubitus position. The L3-L4 space was palpated and the skin was infiltrated with 2% lignocaine to render the procedure painless. Then a 16G Tuohy needle was inserted and epidural space was located by loss of resistance technique. Through the needle an 18G epidural catheter was passed and fixed; the patients were placed in supine position. A test dose 3 ml of 2% lignocaine with adrenaline was given and the patients were observed for 5 min to exclude any intravascular or intrathecal injection. BIS monitor was attached to the patient. The patients were given 2ml/segment of either 0.5% bupivacaine (group-B) or 2% lignocaine with adrenaline (group-L) to achieve a sensory block up to T8 level. Sensory block was assessed by pin prick method. Baseline BIS value was recorded and propofol infusion was started at a rate of 100 µg/kg/min, when sensory block was confirmed. The time to get BIS≤80 was measured as onset time and the surgery was allowed. BIS reading was maintained within a range of 60-80 by titrating the dose of propofol by 10µg/kg/min in every 20 seconds. Propofol infusion was stopped at the end of surgery. The time taken to reach the BIS≥90 was recorded as recovery time.
The primary outcome measures were dose of propofol to get BIS<80 and total dose of propofol consumed; secondary outcome measures were time of onset of block, onset time to get BIS 80, recovery time, vital signs e.g. heart rate (HR), mean arterial pressure(MAP)] and side effects including hypotension, postoperative nausea and/or vomiting (PONV), urinary retention, bradycardia and shivering . All the end points were assessed by an independent observer (SK) who was blinded to group allocation. HR, MAP and BIS were monitored at 5 min intervals till the end of surgery. Intra-operative hypotension was taken as systolic blood pressure < 80 mm of Hg or 20% below baseline value or MAP < 60 mm of Hg and was treated with inj mephentermine 5 mg IV bolus in incremental doses. HR fall <50 was treated with incremental doses of inj. atropine 0.25 mg IV.
Power analysis (alpha=0.05 and beta=0. 0.8) suggested that a sample size of 24 patients per group was needed to detect 30% decrease in propofol requirements to maintain BIS at 60-80. To make provision for drop outs, if any, we enrolled 30 patients in each groups. Therefore, study consisted of 60 patients Statistical analysis was done by using SPSS 16.0 software. Comparison between groups for patient characteristics, onset and recovery times, propofol doses, BIS values, hemodynamic variables and SpO2 was done by independent samples t- test.
RESULTS
All sixty patients completed the study. There was no significant difference regarding the demographic data and volume of epidural 0.5% bupivacaine and 2% lignocaine with adrenaline used in both groups (p>0.05) (Table 1).
The time of onset of block i.e. to achieve T8 level of sensory block, the amount of propofol for onset time to achieve BIS< 80 and total dose of propofol consumed was significantly low in group-B as compared to group-L (p<0.00). Recovery time was significantly prolonged in group-B when compared to group –L (p<0.00). There was no difference in onset time to achieve BIS< 80 for both groups (p>0.05) (Table 2).
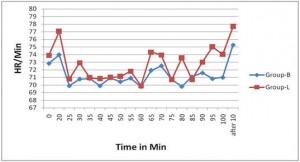
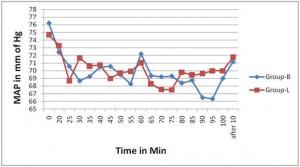
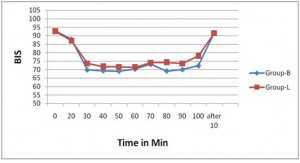
Vital signs like HR, MAP, SpO2 did not change significantly in both group and the inter group differences in these parameter were also not significant (Figure 1 and 2). BIS value was comparable in both groups throughout the procedure (Figure 3).
Side effects like hypotension, urinary retention and bradycardia were more in group–B. Shivering was more in group-L, while PONV was equivalent in both groups (Table 3).
DISCUSSION
We observed significant reduction in propofol requirement for sedation in epidural block obtained with 0.5% bupivacaine.
Most speculated mechanism for sedation during epidural anaesthesia is a de-afferentation phenomenon. The loss of facilitatory input to the reticular activating system renders it more susceptible to actions of sedative drugs. Regarding the afferentation theory, active muscle movement has a stimulatory effect on the central nervous system mediated in part by muscle afferent receptors. Certainly, pronounced reduction of muscle afferent activity and direct neuraxial sensory blockade of the noxious stimulus by epidural anaesthesia may be the reason for its significant effect on the brain’s sensitivity to sedative drugs.6,7
The cause of decreased propofol requirement for sedation or the superior sedative efficacy of bupivacaine can be explained by its greater potency in comparison to lignocaine.8 This greater degree of de-afferentation might be due to a greater potency of bupivacaine than lignocaine and greater availability of the former drug (bupivacaine being more lipid soluble than lignocaine) in the intradural compartment near the spinal cord.
Previous studies have shown that spinal anaesthesia produces general anaesthetic effects,9 and reduces hypnotic requirements.10 Epidural anaesthesia also reduced the requirements of volatile11 and intravenous anesthetics.12 Tadahiko reported that in volunteers, epidural anaesthesia leads to a significant decrease in BIS levels in awake state. In contrast, this study did not reveal any observable sedation before the start of propofol infusion. This is supported by Morley and colleagues,13 who concluded that in nonsedated patients, neither epidural nor spinal anaesthesia produce clinically detectable sedation, whereby they found an increase in ß frequencies similar to that seen in patients with low plasma concentrations of midazolam.
A previous study by Arakawa et al 14 explains that lumbar epidural anaesthesia exerts minimal effects on autonomic nervous system, hence HR and MAP variability are not significant. In our study though the variability in HR and MAP are also statistically insignificant in both groups, but they decreased from the baseline value, which is due to the cardiovascular depressant action of propofol.15 The BIS variability in both groups after 30 , 50 and 80 minutes is statistically significant, which can be explained by the wide range of BIS (60-80) taken to maintain sedation during the study.
Higher incidence of urinary retention in group B was due to long lasting sensory block by bupivacaine, which may affect the voiding capability.16 Higher incidence of bradycardia in group B was perhaps due to more cardiotoxicity with bupivacaine than lignocaine.17
There were a few limitations to this study; first, there was no control group, without any systemic sedation, however, it would not have been ethical to keep the patients unsedated during any surgical procedure. Second, all of our patients were administered 2-3 lit/min of oxygen by face mask and in all patients SpO2 never fell below 96%, so the hypoxia, attributed to the effect of drugs could not be elicited.
CONCLUSION
We conclude that epidural block with 0.5% bupivacaine is associated with less propofol requirement than 2% lignocaine with adrenaline to maintain BIS within a range of 60 to 80.
Acknowledgement: We would like to thank the technical staff that helped us during the study.
Source of Support: Nil
Conflict of interest: Authors declared no conflict of interest.
REFERENCES
- Burns AM, Shelly MP, Park GR. The use of sedative agents in critically ill patients. Drugs 1992; 43: 507–15.
- Boysen K, Sanchez R, Ravn J, Pedersen E, Krintel JJ, Dryberg V. Comparison of induction with and first hour of recovery from breif propofol and methohexital anaesthesia. Acta Anaesthesiologica Scandinavica.1990; 34:212-15.
- DeJonghe, D. Cook and C. Appere-De-Vecchi et al., Using and understanding sedation scoring systems: a systematic review, Intensive Care Med 2000;26: 275- 285.
- Glass PS, Bloom M, Kearse L, et al. Bispectral analysis measures sedation and memory effects of propofol, midazolam, isoflurane, and alfentanil in healthy volunteers. Anaesthesiology 1997; 86:836–47.
- Park WY, Thompson JS, Lee KK. Effect of epidural anesthesia and analgesia on peri-operative outcome. Ann Surg. 2001; 234: 560-571.
- Lanier WL, Iaizzo PA, Milde JH. Cerebral function and muscle afferent activity following intravenous succinylcholine in dogs anesthetized with halothane: the effects of pretreatment with a defasciculating dose of pancuronium. Anaesthesiology 1989; 71:87–95.
- Lanier WL, Iaizzo PA, Milde JH, Sharbrough FW. The cerebral and systemic effects of movement in response to a noxious stimulus in lightly anesthetized dogs. Possible modulation of cerebral function by muscle afferents. Anaesthesiology 1994; 80:392–401.
- Columb MO, Lyons G. Determination of the minimum local analgesic concentrations of epidural bupivacaine and lignocaine in labor. Anaesthesia & Analgesia; 1995; 81: 833-7.
- Pollock JE, Neal JM, Liu SS, et al. Sedation during spinal anaesthesia. Anaesthesiology 2000; 93:728–34.
- Ben-David B, Vaida S, Gaitini L. The influence of high spinal anesthesia on sensitivity to midazolam sedation. Anesth & Analg. 1995; 81:525–8.
- Casati L, Fernández-Galinski S, Barrera E et al. Isoflurane requirements during combined general/epidural anesthesia for major abdominal surgery. Anesth Analg 2002; 94:1331–7.
- Tverskoy M, Shifrin V, Finger J, et al. Effect of epidural bupivacaine block on midazolam hypnotic requirements. Reg Anesth 1996; 21:209–13.
v A. P. Morley, D. C. Chung, A. S. Y. Wong and T. G. Short. The sedative and electroencephalographic effects of regional anaesthesia. Anaesthesia 2000:55:864-9.
v Arakawa M, Goto F. Power analysis of heart rate and blood pressure variability in lumber epidural anaesthesia. Can J Anaesth. 1994; 4:680-7.
- Horiguchi T, Nishikawa T. Heart rate response to intravenous atropine during propofol anaesthesia. Anaesth Analg 2002; 95:389–92.
- Kamphuis ET, lonescu TI, Kuipers TWG, et al. Recovery of storage and emptying functions of the urinary bladder after spinal anaesthesia with lidocaine and with bupivacaine in man. Anaesthesiology 1998; 88:310-16.
- Max GF. Cardiotoxicity of local anesthetics the plot thickness, Anaesthesiology 1984, 60: 3-5.
Table 1: Comparison of patient characteristics, volume of drugs and duration of surgery (Mean+SD).
| Parameters | Group B
(N=30) |
Group L
(N=30) |
p value |
| Age(yr) | 45.67±13.70 | 45.97±9.77 | 0.92 |
| Weight(kg) | 48.00±8.03 | 51.57±8.47 | 0.10 |
| Volume of LA (ml) | 14.53±2.09 | 14.87±1.63 | 0.49 |
| Duration of surgery (min) | 58.50±14.33 | 52.33±12.57 | 0.08 |
LA= Local Anaesthetic; P>0.05 = Non-significant.
Table 2: Comparison of onset time, recovery time and propofol requirements (Mean+SD).
| Parameters | Group B
(N=30) |
Group L
(N=30) |
p value |
| Time of onset of block (min) | 12.07±3.50* | 15.87±2.86 | 0.00 |
| Onset time to get BIS < 80 (min) | 2.88±1.42 | 3.50±1.65 | 0.07 |
| Recovery time (min) to get BIS > 90 | 5.57±1.25 * | 4.38±0.94 | 0.00 |
| Dose of Propofol for onset time
to achieve BIS< 80 (mg) |
17.13±4.22 * | 27.77±8.39 | 0.00 |
| Total dose of propofol (mg) | 140.33±34.59* | 184.80±38.21 | 0.00 |
* denotes the p<0.05; Showing significantly decreased time of onset of block, the amount of propofol for onset time to achieve BIS< 80 and total dose of propofol in group-B.
Table 3: Comparison of adverse effect: Number(%).
| Parameters | Group B
(N=30) |
Group L
(N=30) |
P value |
| Hypotension | 4(13.3) | 3(10) | 0.694 |
| PONV | 1(3.3) | 1(3.3) | 1.000 |
| Urinary retention | 1(3.3) | – | 0.321 |
| Bradycardia | 2(6.6) | – | 0.151 |
| Shivering | 1(3.3) | 3(10) | 0.300 |
PONV= Postoperative nausea vomiting; (p<0.05)
Figure 1: Heart rate at different time periods in both groups. HR=Heart rate
Figure 2: Mean Arterial Pressure (MAP) at different time periods in two groups.
Figure 3: BIS value at different time periods in both groups.