Roopa Sachidananda, DA, DNB*, Safiya Shaikh, MD**, Sarala Mahesh, MBBS***
*Assistant professor; Professor and HoD; ***Junior resident
Department of Anesthesiology, Karnataka Institute of Medical Sciences, Hubli, Karnataka 580 021, (India).
Correspondence: Dr. Roopa Sachidananda, Assistant professor, Department of Anesthesiology, Karnataka Institute of Medical Sciences, Hubli, Karnataka-580 021 (India); Phone: +918362370579; Mobile: +919448658220; E-mail: roopasac@rediffmail.com
Abstract
Patients with intraoral mass may present to anesthesiologists for various diagnostic or definitive procedures. These patients may be challenging not only due to inherent airway problems associated with tumour mass but also due to comorbid conditions. Pedunculated lipoma arising from the buccal mucosa is rare. We report the anticipated airway difficulty encountered in a 55-year-old male patient with an intraoral pedunculated lipoma made easy by the patient by facilitating the mass out of the oral cavity manually.
Key words: Lipoma; Difficult airway
Citation:Sachidananda R, Shaikh S, Mahesh S. Intubation in a patient with a large pedunculated oral lipoma: a unique experience. Anaesth Pain & Intensive Care 2014;18(2):195-197
Introduction
Patients with oral cavity mass may present to anesthesiologist for various diagnostic or definitive procedures. These patients may be challenging not only in view of their inherent airway problems due to tumour mass but the mass may also be associated with some comorbid conditions. Pedunculated lipoma arising from the buccal mucosa is rare and only a few cases have been reported so far. 1-3 Apart from an anticipated difficult airway with a risk of airway obstruction upon induction of general anesthesia, anesthetic concerns also include possibility of trauma to the growth and bleeding.4 We report the anticipated airway difficulty encountered in a 55-year-old male patient with an oral pedunculated lipoma in which our difficulty was eased by the patient by facilitating the mass himself out of the oral cavity manually.
Case report
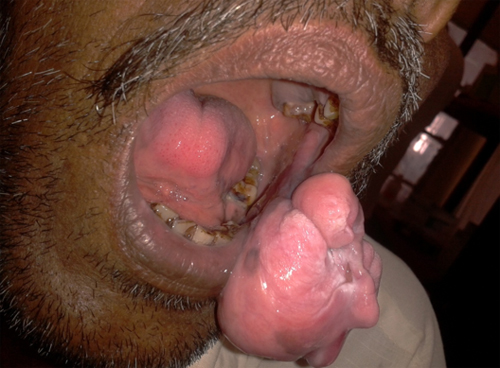
A 55-year-old man presented with a two-year history of swelling in the left buccal cavity which had been progressively increasing in size. He complained of difficulty in chewing, swallowing and speaking. No other positive history was noted. Examination revealed a soft, non-tender, globular red mass of about 10×8 cm in size arising from the left buccal mucosa occupying the oral cavity and obscuring the posterior pharyngeal wall. It became more prominent and popped out of the mouth with the patient manipulating it manually (Figure 1).
Figure 1: Pedunculated intraoral mass presenting outside the oral cavity
General physical examination was unremarkable. Patient’s airway assessment revealed Mallampati class IV. The patient was able to retract the mass out of the oral cavity as the mass was pedunculated. The thyromental and sternomental distances were 7 and 13 cm, respectively. Laboratory investigations were unremarkable. The contrast-enhanced computed tomography revealed a well-defined round homogenous mass lesion measuring 8×10.2×10 cm with smooth margins in the oral cavity occupying most of the oral cavity. It abutted the base of tongue anteriorly and the posterior pharyngeal wall posteriorly. On either side, it extended to the lateral pharyngeal walls.
Excision of the swelling was planned under general anesthesia. After obtaining informed consent including consent for tracheostomy in case of emergency, the patient was scheduled for surgery. On the day of surgery an intravenous line was secured and inj. glycopyrrolate 0.2 mg and midazolam 2 mg was given as premedication. After pre-oxygenating the patient, anesthesia was induced with fentanyl 150 μg and propofol 120 mg intravenously. Mask ventilation was attempted when the patient was apnoeic, however adequate ventilation could not be achieved. A check laryngoscopy was attempted to assess the feasibility of passing the tube beyond the swelling. The mass was seen to be attached to the left buccal mucosa and the blade of the scope could not be passed into the oral cavity. The mass was then scooped out of the oral cavity with the help of a gloved finger in the same manner in which the patient had shown us before and adequate ventilation could now be achieved. Muscle relaxation was achieved with intravenous succinylcholine 80 mg. A 7.5 size cuffed flexo-metallic endotracheal tube was passed without any difficulty and tube position was confirmed by bag ventilation and capnography. Anesthesia was maintained with oxygen, nitrous oxide, propofol infusion and vecuronium. Heart rate, non-invasive blood pressure, peripheral oxygen saturation, electrocardiography and end tidal carbon-dioxide were continually monitored. After the completion of surgery, which lasted for 40 min trachea was extubated uneventfully. The histopathology of the resected specimen indicated that it was a lipoma.
Discussion
Lipomas are benign mesenchymal neoplasms composed of adipocytes. Intraoral lipomas represent 1-4% of all benign tumours involved in oral cavity.5 Lipomas are sessile or pedunculated. Very few cases of intraoral pedunculated lipomas and their anesthetic implications have been reported in literature.1-3
Establishing an airway in a patient with intraoral mass is a nightmare to the anesthesiologist. Surgical excision of such tumours is best done under local anesthesia when the mass is small. However large swellings, vascular lesions, pedunculated lesions which require proper exposure need to be considered under general anesthesia. General anesthesia was opted for in our case for the convenience of maintaining adequate airway and to facilitate surgical approach. Difficulties may be encountered either during mask ventilation or during laryngoscopy when the mass occupies the oral cavity and is fixed and this may lead to considerable morbidity and/or mortality, especially in a situation of ‘cannot intubate, cannot ventilate’.6,7 There was no history of snoring in our patient and we did encounter difficult mask ventilation on induction of anesthesia until the lesson taught by the patient was recalled and implemented by manually bringing out the pedunculated mass from the oral cavity.
Difficult mask ventilation is an underestimated aspect of the difficult airway and needs its due emphasis. Awake fibreoptic intubation is an invaluable technique in airway management.8-10 However, it needs considerable expertise, especially in a large intraoral mass where trauma to the mass could initiate bleeding and obscure the field.11 Flexible fiberscopes arenot available at most of the centres in the subcontinent and this aspect needs to be highlighted at appropriate forums. Tracheostomy, as a last resort, would have to be done in case of a failed intubation.
Anesthesia in our patient was well maintained with oxygen, nitrous oxide, propofol infusion and vecuronium as it was the routine practice followed in our hospital. In fact our difficulties were removed by the patient himself by showing us the probability of pulling the mass out of the oral cavity, leaving enough space for mask ventilation and conventional laryngoscope aided intubation.
Conclusion
Airway management in cases with intraoral mass requires a range of manual skills, as well as knowledge and judgement. Although flexible fibreoptic intubation is the gold standard for such cases, the lack of its universal availability and expertise can be a limiting factor especially in the developing countries. Our case was unique and has been reported to highlight the anticipated difficulty and how it was overcome during mask ventilation.
References
- Shah KM. Twin pedunculated intraoral submucosal lipoma. BMJ Case Rep. 2013; pii: bcr2013009774. [PubMed][Free Full Text]
- Dai XM, Li YS, Liu H, Liu L. Giant pedunculated fibrolipoma arising from right facial and cervical region. J Oral Maxillofac Surg. 2009;67:1323-6.[PubMed]
- Persaud RA, Kotnis R, Ong CC, Bowdler DA. A rare case of a pedunculated lipoma in the pharynx. Emerg Med J. 2002;19:275. [Pubmed][Free Full Text]
- R Garg, V Darlong, R Pandey, J Punj. Anesthesia for Oncological ENT surgeries: Review. The internet Journal of Anesthesiology. 2008;Volume 20, Number 1. [Access Online]
- de Castro AL, de Castro EV, Felipini RC, Ribeiro AC, Soubhia AM. Osteolipoma of the buccal mucosa. Med Oral Patol Oral Cir Bucal 2010;15:347-349. [PubMed][Free Full Text]
- Adnet F. Difficult mask ventilation. Anesthesiology 2000;92:1217-1218. [PubMed][Free Full Text]
- Baskett PJF, Bossaert L, Carli P, Chamberlain D, Dick W, Nolan JP et al. European resuscitation council writing subcommittee. Guidelines for the advanced management of the airway and ventilation during resuscitation. Resuscitation 1996;31:201-230. [PubMed]
- Benumof JL. Laryngeal Mask Airway and the ASA difficult airway algorithm. Anesthesiology 1996;84:686-699. [PubMed][Free Full Text]
- Caplan R, Benumof JL, Berry FA, Blitt CD, Bode RH, Cheney FW et al. Practice guidelines for management of the difficult airway: a report by the ASA Task Force on Management of the Difficult Airway. Anesthesiology 1993;78:597-602. [PubMed][Free Full Text]
- Ovassapian A, Krejcie TC, Yelich SJ, Dykes MHM. Awake fibre-optic intubation in the patient at high risk of aspiration. Br J Anaesth 1989;62:13-16. [PubMed][Free Full Text]
- Huitink JM, Balm AJM, Keijzer C, Buitelaar DR. Awake fibrecapnic intubation in head and neck cancer patients with difficult airways: new findings and refinements to the technique. Anaesthesia 2007;62:214-219. [PubMed]
Answers to the queries
S1 Reference about the patient given
S2Reference given
S3Anatomical location mentioned
S4 The word ‘elevated’ is deleted
S5, S6, S11 This mobile mass was large enough as described to obscure the contents of the oral cavity. However, it could be manipulated in and out of the oral cavity.
S7 Figure mailed already
S8 measurements deleted
S9 Airway examination revealed Mallampati class IV with the mass inside the oral cavity.
S10 Sentence deleted
S12This is a unique case which is is being reported as a case of unanticipated difficult mask ventillation. As this patient gave no history of snoring we did not anticipate any difficulty in mask ventilation.
S13 Sentence added in discussion.
S14 rectified
S15 Oral intubation was performed as requested by the surgeon. Nasal fibreoptic intubation is known to cause epistaxis.
S16 Reference given
S17 sentence modified
S19, S18 references rectified
S20 No other photographs are available