Pratheeba. N, DNB*, Neha Singh, MD*, Ranjan R.V, DA, DNB**, T. R. Ramachandran, MD***, Sageev Koshy George, MD***, Ramya GS, MD****
*Assistant Professor, **Associate Professor, ***Professor, ****Postgraduate Resident
Department of anesthesiology, Pondicherry Institute of Medical Sciences , Pondicherry
Correspondence: Dr. Pratheeba Natarajan, Department of Anesthesiology, Pondicherry Institute of Medical Sciences, Kanagachettikulam, Pondicherry 605014 (India); Cell: 09894919554; e-mail: pratheeba.rk@gmail.com
ABSTRACT
Alkaptonuria is a rare inherited autosomal recessive disorder of metabolism due to deficiency of homogentisic acid oxidase. This results in deposition of homogentisic acid in almost all the collagenous structures of the body leading to progressive multisystem involvement (alkaptonuric ochronosis) and poses a big challenge in anesthetizing such patients. We present one such case posted for total hip replacement and its successful management under general anesthesia.
Key words: Alkaptonuria; Ochronosis; Homogentisic acid oxidase; Ochronosis
Citation: Pratheeba N, Singh N, Ranjan RV, Ramachandran TR, George SK, Ramya GS. Anesthetic management of a case of alkaptonuria. Anaesth Pain & Intensive Care 2013; 17(2):179-181
INTRODUCTION
Alkaptonuria is an autosomal recessive inherited disorder of tyrosine metabolism in which there is a deficiency of homogentisic acid oxidase.1 This leads to the deposition of a polymer of homogentisic acid, an ochre colored pigment in the cartilages and connective tissue.2 It is characterized by a triad of homogentisicaciduria, ochronosis and arthritis.2
Alkaptonuria occurs about 1 in 250000 to 1 in 1000000, the incidence being much higher in Slovakia upto 1 in 19000.3 The most common clinical manifestations of this disorder are severe arthritis and pain, restrictive lung disease, coronary artery disease, valvular heart disease, nephrolithiasis and other renal complications3.
Therefore the successful anesthetic management of these patients depends on the thorough evaluation and optimization of comorbidities, to prevent the associated perioperative complications.
CASE REPORT
A 50 yr old male patient came to our hospital with complaints of pain in the left hip, low backache and difficulty in walking since one year for which he was on tablet diclofenac sodium 50 mg thrice daily. He was a known hypertensive since 2 years, controlled with tablet atenolol 25 mg once a day. On examination, patient was conscious and oriented with a heart rate of 80/min and blood pressure of 130/80mmHg. Examination of cardiovascular and respiratory systems was normal. Black pigmentation of the sclera was observed along with auricular cartilage thickening. Airway examination revealed Mallampati Class II with adequate mouth opening and normal thyromental distance and minimal restriction of neck movements. Spine examination revealed narrowed intervertebral disc spaces. Investigations revealed hemoglobin of 13mg/dL, biochemical reports were within normal limits. Chest x-ray and 12 lead ECG were normal. A lumbosacral x-ray revealed sclerosis and narrowing of all the disc spaces (Figure 1). These x-ray findings along with black pigmentation of sclera and auricular cartilage thickening made us suspect a metabolic abnormality in the patient. On further detailed questioning, the patient reported a blackish discoloration of urine and staining of the undergarments which prompted us to do a urinalysis which revealed urine discoloration when exposed to air. A diagnosis of ochronosis of the left hip with severe secondary osteoarthritis was made. The patient was accepted for cemented total hip arthroplasty on the left side under ASA functional class II. A general anesthesia with controlled ventilation was planned. A written informed consent was obtained and the antihypertensive was continued on the morning of surgery. Patient was kept nil oral for 8 hours.
In the OR, an 18G IV cannula was placed in the left forearm. Standard monitors, e.g. ECG, SpO2 and NIBP, were instituted. Difficult intubation cart was kept ready. After preoxygenation for three minutes, patient was premedicated with 100 mcg fentanyl. Anesthesia was induced with inj. propofol 100 mg and atracurium 25 mg was given to facilitate intubation. Laryngoscopy revealed a Cormack-Lehane grading of II which improved to grade I with external laryngeal manoeuvre. The trachea was intubated with 8.0 mm endotracheal tube.
Anesthesia was maintained with isoflurane in oxygen and nitrous oxide and atracurium. Analgesia was maintained by bolus doses of fentanyl. Surgery lasted for two and half hours. Patient was reversed with neostigmine and glycopyrrolate and extubated once he was fully conscious.
DISCUSSION
The term alkaptonuria was first described by Boedeker in 18913. Virchow in 1866 coined the term ‘ochronosis’ meaning yellow disease in Greek, because the accumulated pigment in the connective tissue was ochre coloured.4
Ochronosis is of historical importance, as it was one of the first conditions in which Mendelian recessive inheritance was proposed and also became the corner stone of the fundamental concept of inborn errors of metabolism.5
Alkaptonuria is an autosomal recessive inherited genetic disorder of tyrosine metabolism. The deficiency of the enzyme homogentisic acid oxidase results in the accumulation of homogentisic acid (HGA). Initially, it is excreted by the kidneys and that which is not excreted through urine is polymerized into ochre coloured pigment which is deposited within the cartilage and collagenous structures. This is known as endogenous ochronosis.6 There is no specific therapy for these patients, however dietary protein reduction and ascorbic acid intake reduces urinary excretion of homogentisic acid and possibly reverse bone abnormalities.5
The clinical manifestations per se determine the guidelines for the perioperative management of the patient with ochronosis as there are no preset guidelines. The anesthetic technique is dependent on the evaluation and optimization of the systemic dysfunction.7,8
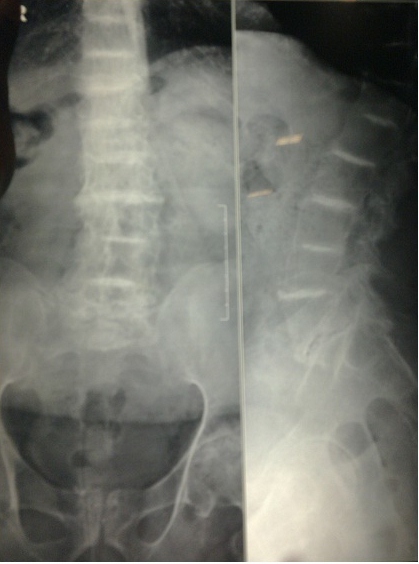
The pigment deposition in the cartilages of the skeletal system results in severe pain as a result of brittleness, fragmentation and destruction. These changes stress the importance of proper padding and careful positioning of the patient.9 Degenerative changes in the spine comprise of disc calcification, narrowing of intervertebral disc spaces and in extreme cases may lead to cord compression, which makes preoperative neurological examination mandatory. Difficulty in performing regional blocks is expected in these patients (as evident from the x-ray of the spine of our patient), hence regional anesthesia was deferred and general anesthesia was contemplated.
The cartilaginous tissue of the respiratory system may also be affected by ochronosis with heavy deposition of the pigment in the laryngeal, tracheal and bronchial cartilages resulting in hoarseness, dyspnea and difficult airway access.4 Hoarseness may indicate narrowing of glottis and may necessitate a smaller sized tube. Deposition of pigment and the degenerative changes in the cervical spine may result in the restriction of motion cervical spine further adding to the difficulty in airway management.4 Our patient had minimal restriction of the cervical spine, laryngoscopic grading was Cormack Lehane grade II. Intubation was done in the second attempt successfully with external laryngeal manouevre and gum elastic bougie. Involvement of the cartilaginous structures of the respiratory system may cause restrictive pathology signaling the need for a thorough preoperative pulmonary function analysis.8
Figure 1: X-ray LS spine (PA & Lateral) showing scleroses of all disc spaces
A spectrum of cardiovascular abnormalities such as calcified and stenotic valves, atherosclerosis and conduction blocks mandate an extensive evaluation of the cardiovascular system, thereby helping us in the tailoring of the anesthetic technique as required, and also in deciding about invasive monitoring usage.10 Our patient did not have any of the above mentioned cardiovascular abnormalities except for hypertension which was under control, hence the need for invasive monitoring did not arise. Excessive pigment deposition in the nails may interfere with pulse oximetry.2
Renal dysfunction as a result of inadequate excretion of HGA often results in renal calculi, UTI, obstructive uropathy and eventually renal failure, which however was not seen in our patient.11 However, since our patient was on non-steroidal anti-inflammatory agents for nearly an year for chronic pain, renal function tests, electrolytes and coagulation profile were done, as long term usage may result in platelet dysfunction, prolongation of bleeding time and gastrointestinal bleed12. The coagulation profile may indicate if central neuraxial blockade can be safely given, but regional anesthesia in this patient has its own demerits.
SUMMARY
Although rare, the anesthetic management of a patient with alkaptonuric ochronosis can be complex and challenging. Numerous literature is available which describe the clinical manifestations of this disease but very minimal information is available regarding the anesthetic management. Since there are no set guidelines for the anesthetic management, the systemic involvement should determine the anesthetic plan. A thorough preoperative evaluation, optimization with due anesthetic considerations for musculoskeletal and collagen vascular disorders may be beneficial in the management of these patients.
REFERENCES
1. Van Offel JF, De Clerck LS, Francx LM, Stevens WJ. The clinical manifestations of Ochronosis: a review. Acta Clin Belg 1995;50:358-62. [PubMed]
2. Ravindra Pandey et al. Perioperative management of patient with alkaptonuria and assosciated multiple comorbidities. JAnaesth clin pharmacol 2011;27:259-61. [PubMed] [Free Full Text]
3. Fisher AA, Davis MW. Alkaptonuric Ochronosis with Aortic valve and joint Replacements and femoral fracture: A case report and literature review. Clinical Medicine and Research 2004;2:209-15. [PubMed] [Free Full Text]
4. Collins E, Hand R. Alkaptonuric Ochronosis: A case report. AANA 2005;73:41-6. [PubMed]
5. Garrod E. The incidence of alkaptonuria: a study in chemical individuality. Lancet 1902;2:1616-20. [PubMed]
6. Micali G, DiStefano AG,Nasca MR,Mususmeci ML. A 46 year old man with a 4–year history of diffuse black pigmentation. Arch Dermatol 1998;134:98-101. [PubMed]
7. Dierdorf SF. Anesthesia for patients with rare and coexisting diseases. In: Barash PG, Cullen BF, Stoelting RK, eds. Clinical anesthesia. 4thed. Philadelphia, Pa: Lippincott Williams and Wilkins; 2001: p491-514.
8. Rosenblatt WH. Airway management. In: Barash PG, Cullen BF, Stoelting RK, eds. Clinical Anesthesia. 4th ed. Philadelphia, Pa: Lippincott Williams and Wilkins; 2001: p595-632.
9. Nitu M, Ancona K, Coleman C, Tunnessen WW Jr. Picture of the month. Arch Pediatr Adolescent Med 2001;155:1063-64. [PubMed] [Free Full Text]
10. Kocyigit H, Gurgau A, Terzioglu R, Gurgau G. Clinical radiographic and echocardiographic finding in a patient with ochronosis. Clin Rheumatol 1998;17:403-406. [PubMed]
11. Rotter S. Specific considerations with cardiac disease. In: Hurford WE, Balin MT, Davison JK, Haspel KL, Roscow C, eds. Clinical Anesthesia Procedures of the Massachusetts General Hospital. 5th ed. Philadelphia, Pa:Lippincott Williams and Wilkins; 1998:p14-32
12. Introne WJ, Phornphutkul C, Bernardini I, McLaughlin K, Fitzpatrick D, Gahl WA. Exacerbation of the Ochronosis of Alkaptonuria due to renal deficiency and improvement after renal transplantation. Mol Genet Metab 2002;77:136-42. [PubMed]
13. Marley RA, Kremer MJ, Alves SL. Preoperative evaluation and preparation of the patient. In: Nagelhout JJ, Zaglaniczny KL, eds. Nurse Anesthesia. 2nded. Philadelphia, Pa: WB Saunders.2001: p308-340.