Said D. Abuhasna, MD*, Mustafa Abu Ebaid, MD**, Eman D.M. Qadoom, Pharm D***,
Masood Ur Rahman, MD****
*Chairman; **** Deputy Chairman, Department of Critical Care Medicine
**Resident, Department of Internal Medicine
*** Department of Pharmacy
Tawam Hospital, P.O.Box 15258 Al Ain (United Arab Emirates)
Correspondence: Said Abuhasna, MD., Chairman, Department of Critical Care Medicine, Tawam Hospital, P.O. Box 15258, Al Ain, Abu Dhabi, UAE
Email: sabuhasna@tawamhospital.ae ; sabuhasna@gmail.com
ABSTRACT
Self-strangulation is an important cause of homicidal and suicidal injury, leading to death due to asphyxia and may be accidental or suicidal. Accidental strangulation is rare, and to be strangulated by a scarf is even less common. We report a 19-year-old male who was accidentally strangulated by his own scarf or ‘ghutra’ (a traditional cotton headdress worn by Arab males), while working on his idle vehicle engine, resulting in anoxic brain encephalopathy. The patient remained in a persistent vegetative state and ventilator dependent.
Because this was previously an unrecognized hazard of ‘ghutra’ as well as the unique mode of injury, it prompted us to report this case to highlight the circumstances surrounding the event in order to minimize similar.
Key words: Headscarf; Ghutra; Strangulation; Anoxic brain encephalopathy
Citation: Abuhasna SD, Ebaid MA, Qadoom EDM, Rahman MU. Accidental asphyxiation by an Arabic headscarf. Anaesth Pain & Intensive Care 2013;17(1):91-93
INTRODUCTION
Accidental strangulation is rare, and to be strangulated by a scarf is even less common. The traditional Arabic headdress goes by several names. It is called a ‘keffiyeh’, ‘shmagh’, ‘ghutra’ or a scarf. It can be worn in several different ways, either by itself or with a cap (‘igal’) and wreath (‘tagiyyah’) to keep it in place. The scarf was initially used by the dwellers of the desert to protect them from the harsh rays of the sun and the whipping sands of the desert. It still serves that purpose, but now it has become a symbol of Arab culture. It is also worn at weddings and by heads of state, when it serves a purely decorative function. The ‘shmargh’ is a large square piece of cotton cloth that is woven in a distinctive checkered design. It is usually red and white, or black and white.1
We present a case of a 19 years old male who was accidentally strangled by his own scarf, while he was working on his idle running vehicle. The scarf was accidentally tangled into the fan of the engine and tightened around his neck leading to asphyxiation and brain death, which left the patient in a persistent vegetative state.
CASE REPORT
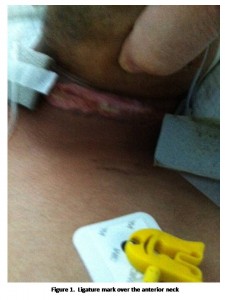
A 19 years old healthy male (weight 66 kg, height 155 cm) was admitted to our intensive care unit (ICU), comatosed with multiple facial abrasions and a fresh injury mark around his neck. The history was provided by the front seat passenger who was patient’s first cousin. The patient and his cousin were driving to report as newly inducted recruits to the police academy for training on a chilly morning. The patient was wearing the traditional scarf around his head and neck to keep him warm. On their way to the academy, the vehicle engine stalled. The patient reportedly exited the vehicle and opened the hood to check the engine. He was able to restart the engine while his head was still under the hood. Evidently, the fan of the engine started abruptly, catching his scarf in the fan belt, and tightening it progressively more and more around his neck leading to asphyxiation with loss of consciousness. The passenger, who saw that his cousin head slammed on the engine, immediately turned off the engine and called Emergency Medical Service 911. Subsequently, he attempted to untangle the scarf and get it released from the fan, but he was not successful. The victim sustained asphyxiation and quickly became unconscious. The Emergency Medical Service transported the patient to the hospital on oxygen supplementation and monitoring. He was resuscitated at the trauma centre. Upon arrival to the ICU the patient was on a ventilator and was flaccid with a Glasgow coma scale of 3/15 and with decerebrate posture. The oxyhemoglobin saturation was 97% on FiO2 45%. The ventilatory rate was 12 in the assist control mode with a tidal volume of 6 ml/kg and a positive end-expiratory pressure (PEEP) of 5 cmH2O. The heart rate was 75 bpm in normal sinus rhythm, the temperture was 37.1° C and the BP was 100/58 mmHg. The pupils were fixed and dilated at 7 mm. There was a ligature mark over the anterior neck (Figure 1). No other injuries were found. Rest of his examination was unremarkable.
In the subsequent few days, he suffered from episodes of generalized tonic-clonic convulsions and ARDS, probably due to aspiration pneumonia. Arterial blood gas analysis showed PO2 of 56 mmHg on FiO2 90% and the chest radiograph showed bilateral infiltrates. The plain radiograph of the neck did not reveal any hyoid or cervical vertebral fractures and a computerized tomography (CT) scan of cranium showed skull fracture with moderate subdural hematoma on the right parietal area which was surgically evacuated. CT scan of the neck was unremarkable. Patient was treated with intravenous phenytoin for seizures; on 5th day of ICU admission, he developed diabetes insipidus (DI) and was treated with desmopressin infusion.
Due to his deep coma and vegetative state, tracheostomy was performed and he was placed on long term ventilation.
DISCUSSION
In different types of strangulation, the initially applied ligature causes venous congestion with stasis of cerebral blood leading to unconsciousness. After the person is limp, the ligature can tighten, progressing to complete arterial occlusion. Vagal reflexes from pressure on the carotid bodies can lead to dysrhythmias. Airway compression does not play an important role in the pathophysiology of strangulation injuries. Laryngeal fractures have been reported in hanging deaths but are rare in survivors.
The clinical features of strangulation can include indentation of the neck in the course of the ligature or other signs of trauma to the neck, such as scratches, abrasions or lacerated wounds (Figure 1).
Tardieu spots are petechial hemorrhages in the conjunctiva, mucous membranes, and skin cephalad to the ligature marks.2,3 Strangulation is a common method of homicide, but accidental ones like our case are rare. Accidental strangulation is a potentially fatal injury and only two cases similar to ours have been reported.4 In strangulation, and in some suicidal hangings where the individual is “saved” before death, there may be a variable period of survival, but with brain damage, followed by death. This delay is the effect of loss of blood flow to the brain, with partial asphyxiation of the brain. A decrease in blood flow to the brain will produce a pathologic change called anoxic encephalopathy. In our case there was strangulation with the headscarf, that resulted in anoxic encephalopathy and a vegetative state. The process of strangulation, whether by hand (manual) or by a ligature, results in blunt injury of the soft tissues of the neck. The pattern of these injuries allows us to recognize strangulation as a mechanism, and to distinguish strangulation from other blunt injuries including hanging, traumatic blows to the neck, and artifacts of decomposition.2,3 Fatal anoxic encephalopathy results in clinical “brain death” where the body functions of the heart and internal organs can be maintained by medical life support, but all hope of meaningful recovery is lost. Complications may include persistent vegetative coma, cerebral edema, and herniation of the brain. Apparently this is not the first case to die from strangulation of own headscarf. Searching the internet, we found two cases only reported in the news and information sites, but not in medical literature. The first case was of a well known American dancer named Angela Isadora Duncan, who died in a car accident in 1931. Her silk scarf, draped around her neck, became entangled around the open-spoked wheels and rear axle, breaking her neck.4 The second case was of a teenager girl Suzanne Cornwell, 18. She was strangled to death by her scarf in a freak go-karting accident when the garment got caught in the engine the first time she had ever tried the sport. Accidental strangulation of this variety is under-reported in the third world countries and is preventable if the public follows safety recommendations. Since the occurrence of this case we have started short courses of instructions to primary care physicians to provide anticipatory guidance to the public of the United Arab Emirates, and to explain to their patients and their families the dangers and the potential strangulation by a headscarf in certain situations such as inspection of a vehicle under the hood while the engine is running.
REFERENCES
1. How to Wear an Arabic Headdress: Available on http://www.ehow.com/how_6046805_wear-arabic-headdress.html. (Accessed on 10 March 2013).
2. Kelly M: Trauma to the neck and larynx [Review]. CRNA 1997 Feb;8(1):22-30. [PubMed]
3. Missliwetz J, Vycudilik W: Homicide by strangling or dumping with postmortem injuries after heroin poisoning? Am J Forensic Med Pathol. 1997 Jun;18(2):211-4. [PubMed]
4. Craine, Debra and Mackrell J. The Oxford Dictionary of Dance. Oxford University Press, Oxford. 2000; p152. ISBN 0-19-860106-9