Ashwini H. Ramaswamy*, Madhuri S. Kurdi**, Safiya I. Shaikh***,
Radhika S. Deva****, Syed Uwais Raza****
*Assistant Professor; **Professor; ***Professor & HoD; ****Postgraduate Student
Department of Anesthesiology, Karnataka Institute of Medical Sciences, Hubli, Karnataka, (India)
Correspondence: Dr Ashwini H. Ramaswamy, # NANDANA, Plot no 11, Deshpande Layout Second Stage, Hubli, Karnataka (India); Phone: 9448317163; E-mail: ashvenki.hubli@gmail.com
ABSTRACT
Prolonged tracheal intubation is a common cause of tracheal stenosis. These patients may present with respiratory insufficiency and stridor of insidious onset and progressive nature. Immediate management includes securing the airway which requires anesthesia. We present successful management of a case of post intubation tracheal stenosis using rigid bronchoscopy under a combination of regional and general anesthesia
Key words: Tracheal stenosis; Bronchoscopy; Stridor; Tracheostomy; Central airway obstruction
Citation: Ramaswamy AH, Kurdi MS, Shaikh SI, Deva RS, Raza SU. Awake rigid bronchoscopy for post intubation tracheal stenosis. Anaesth Pain & Intensive Care 2014;18(3):299-301
INTRODUCTION
The causes of adult tracheal stenosis include trauma, neoplasm, inflammation or collagen vascular diseases. The most common cause is trauma which can be internal (prolonged tracheal intubation, tracheotomy, burns) or external (blunt/penetrating neck injuries).1,2 Despite improvement in tracheal and tracheostomy tube design and material, tracheal stenosis after intubation remains an important cause of life threatening tracheal obstruction. The current therapeutic approaches for these patients include tracheobronchial stenting, surgical correction, progressive dilation or laser tracheoplasty.2,3
The reported incidence of tracheal stenosis following intubation ranges from 6-21%.4 Anesthesiologists are important and active participants in relieving the central airway obstruction. This article focuses on relevant anesthetic considerations in the airway management in an adult patient with tracheal stenosis.
CASE REPORT
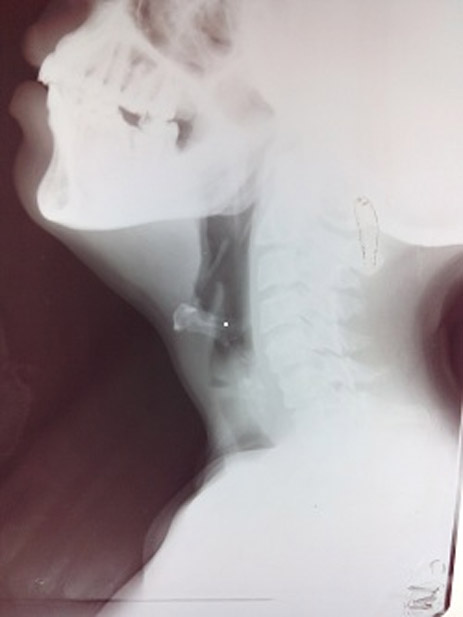
A 21 year old female patient presented with complaints of progressive difficulty in breathing and stridor for the last ten days. Patient had had accidental drowning 30 days back, for which she was intubated via the oral route and mechanically ventilated for ten days. She was discharged on 15th day of admission following restoration of normal respiration. On examination, she was tachypneic, wheezing and using accessory muscles of respiration. Pulse oximeter showed 80 % saturation on room air which worsened on lying down. Saturation improved on oxygen supplementation. A provisional diagnosis of post-intubation tracheal stenosis was made. An x-ray of the neck showed decreased air column below the glottis (Figure 1). Bronchoscopy revealed severe tracheal stenosis at the level of third and fourth tracheal ring.
In view of severe respiratory distress and lower tracheal stenosis, rigid bronchoscopy was planned. Patient was nil by mouth for the past seven hours. She was given inj. ranitidine 150 mg, metoclopramide 10 mg intravenously and transferred to the operating room. Her monitoring included NIBP, ECG, and pulse oximetry. Patient was positioned supine with a 20° head up tiltand 100% oxygen was supplemented through mask via Bain’s circuit. Glycopyrrolate 0.2 mg and fentanyl 100 µg was given IV avoiding anxiolytics. The superior laryngeal nerve was blocked bilaterally and the trachea was anesthetized using lignocaine 2% with 24G needle through the cricothyroid membrane. A Storz™ ventilating rigid bronchoscope was inserted and the fibrous membrane was incised. Relief of stenosis was indicated by the passage of the bronchoscope beyond the obstruction. At this juncture 80 mg propofol was administered and muscle relaxation was achieved with vecuronium 4 mg. Patient was ventilated through the side arm of the bronchoscope and tracheostomy was done at the level of the third and fourth tracheal rings. The stenotic site was serially dilated using inflated cuffs of different sized polyvinyl chloride (PVC) endotracheal tubes (ETT) until it could allow the passage of cuffed tracheostomy tube No. 7. The patient was reversed with neostigmine and glycopyrrolate and transferred to the intensive care unit for further management. Tracheal stenting was planned at a later date.
Figure 1: Lateral view of neck on x-ray showing distorted anatomical shadow of trachea
DISCUSSION
During the poliomyelitis epidemic in 1950’s, mechanical ventilation demanded prolonged oral endotracheal intubation. This resulted in various complications, of which tracheal stenosis at the cuff site was the most common.3Studies have identified cuff pressure exerted on the tracheal mucosa as the main cause.4 High cuff pressure (>30 mmHg) causes mucosal ischemia of trachea resulting in ulceration and chondritis of cartilages which heal circumferentially by fibrosis leading to tracheal stenosis.2,5-8A prospective study showed that the use of high volume, low pressure cuffs is also associated with tracheal stenosis in 11% of patients.3,4,9 Symptoms can be shortness of breath, inspiratory stridor and expiratory wheeze (monophonic) on exertion.10 The patient becomes symptomatic at rest and respiratory insufficiency may ensue with the trachea stenosed to 30% and 75% of the original diameter respectively.1Ahistory of previous intubation, coupled with symptoms unresponsive to bronchodilators are important indicators of tracheal stenosis.6
Rigid bronchoscopy and tracheal dilatation possibly with stent replacement is the only treatment required for small lesions. In severe cases it provides time for definitive procedures.3,11 Beside the degree of stenosis, position of stenosis is also important for anesthesia. For upper tracheal stenosis, a tracheal tube can be inserted below the stenotic area under local anesthesia or cervical epidural block. For most severely obstructed patients with critical stenosis and at risk of complete respiratory failure at any time, conventional anesthetic technique would be catastrophic as attempts at inserting a small ETT may cause complete obstruction of the airway. In these patients, the anatomy allows ventilation when breathing spontaneously.1
The anesthetic considerations for rigid bronchoscopy in tracheal stenosis are multiple and complex;12
- These surgical procedures take place in high risk patients
- Symptoms can be insidious and patient may present with advanced stenosis before developing dyspnoea
- Reconstructed multi-slice computerised tomography can be helpful as it details the nature, location of the airway obstruction and its effect on adjacent structures.
- If time permits, the significant medical co morbidities especially obstructive lung disease or infections can be optimized before the procedure.
- The relationship between the position of the patient, and relief or aggravation of the symptoms should be identified and considered during induction of anesthesia to relieve life threatening airway obstruction.
- Avoid anxiolytics as physiological reserve is limited and administration of anesthetic drugs as well as airway securing techniques can be sometimes risky as they can depress the patient’s auto compensation in a hypoxic setting resulting in respiratory and cardiac arrest.12
For emergent central airway obstruction rigid bronchoscopy is the airway stabilization procedure of choice,14 and induction of anesthesia needs to be tailored to the patients’ lesions and their medical history. The focus of induction should be rapid control of the airway because mask ventilation requires high pressures and may result in gastric distension. If mask ventilation is required, then rate should be slowed with longer inspiration and expiration time. Conacher et al suggest that the primary concern in central airway obstruction is not the limitation of inspiratory airflow but dynamic hyperinflation with hypercarbia and hemodynamic collapse.15 We preferred anesthetising the airway with regional blocks and anesthesia of the trachea using a local anesthetic agent. We opted for spontaneous breathing in accordance with the traditional teaching recommendation to defend against complete airway obstruction and as a protection against periglotic dynamic airway collapse.10 We did not attempt to pass an ETT, as blind passage of tube down the stenosed airway might have resulted in both bleeding as well as complete obstruction of the airway by friable tissue. Moreover in our case the stenosis was subglottic, which might have made the seating of an ETT impossible. Other ventilator modalities include intermittent positive pressure ventilation and low/high frequency jet ventilation.
Anesthesia can be maintained with either inhalational or intravenous agents. Inadequate scavenging and coupling of anesthetic delivery with ventilation is disadvantageous with former technique and cardiorespiratory depression in the latter method. Once the airway was secured, we used drugs intravenously to maintain the depth of anesthesia during frequent periods of suctioning, airway dilation and during insertion of tracheotomy tube when ventilation was interrupted. Selective use of steroids and racemic epinephrine may help in reducing the glottis oedema. Irrespective of the technique, the patient should be rendered awake with intact airway reflex at the end of the procedure.10
CONCLUSION
Tracheal stenosis secondary to prolonged intubation can present with stridor and respiratory insufficiency to the emergency department. Patient distress and lack of time for optimization of comorbid medical disorders may result in inadequate preparation for any type of anesthesia and surgical intervention. In these decompensated patients, securing the airway using minimal anesthetics is often demanded and justified. Our case shows that, rigid bronchoscopy done under a combination of regional and general anesthesia can lead to a successful outcome in such a challenging situations.
REFERENCES
- Zhou YF, Zhu SJ, Zhu SM, An XX. Anesthetic management of emergent critical tracheal stenosis. Zhejiang Univ Sci B 2007;8:522-25. [PubMed][Free Full Text]
- Dass A, M Nagarkar N, K Singhal S, Verma H. Tracheal T-Tube Stent for Laryngotracheal Stenosis: Ten Year Experience. Iran J Otorhinolaryngol 2014;26;37-42. [PubMed][Free Full Text]
- Spittle N, McCluskey A. Lesson of the week: tracheal stenosis after intubation. BMJ 2000;321:1000–2. [PubMed][Free Full Text]
- Sarper A, Ayten A, Eser I,Omer Ozbudak O, Demircan A. Tracheal stenosis after tracheostomy or intubation. Tex Heart Inst J 2005;32:154-8. [PubMed][Free Full Text]
- Kartik Syal, Anil Ohri, J. R. Thakur. Emergency tracheal reconstruction in a patient of tracheal stenosis. J Anaesthesiol Clin Pharmacol 2011;27:115-116. [PubMed][Free Full Text]
- Andrews MJ, Pearson FG. Analysis of 59 cases of tracheal stenosis following tracheostomy with cuffed tube and assisted ventilation, with special reference to diagnosis and treatment. Br J Surg. 1973;60:208–12. [PubMed]
- Cooper JD, Grillo HC. The evolution of tracheal injury due to ventilatory assistance through cuffed tubes: a pathologic study. Ann Surg 1969;169:334–48. [PubMed][Free Full Text]
- Cooper JD, Grillo HC. Experimental production and prevention of injury due to cuffed tracheal tubes. Surg Gynecol Obstet 1969;129:1235–41. [PubMed]
- Stauffer JL, Olson DE, Petty TL. Complications and consequences of endotracheal intubation and tracheotomy. A prospective study of 150 critically ill adult patients. Am J Med 1981;70:65–76. [PubMed]
- Daumerie G, S Su, E.A. Ochroch. Anesthesia for the Patient with Tracheal Stenosis. Anesthesiology Clin 2010;28:157–174. [PubMed]
- Kim HJ, Kim SW, Lee HY, Kang HH, Kang JY, Kim JS, et al. Clinical experience of rigid bronchoscopy in single center. Tuberc Respir Dis 2012;72:486–492. [PubMed][Free Full Text]
- Finlayson, Gordon N, Jay B. Brodsky. Anesthetic considerations for airway stenting in adult patients. Anesthesiology Clin 2008;26:281–91.
- Madan K, Agarwal R, Aggarwal A N, Gupta D.Therapeutic rigid bronchoscopy at tertiary care centre in north India; initial experience and systematic review of Indian literature. Lung India. 2014;31:9–15. [PubMed][Free Full Text]
- Conacher ID. Anaesthesia and tracheobronchial stenting for central airway obstruction in adults. Br J Anaesth 2003;90:367–74. [PubMed][Free Full Text]
- Knowlson GTG, Bassett HFM. The pressures exerted on the trachea by tracheal inflatable cuffs. Br J Anaesth 1970;42:834–7. [PubMed][Free Full Text]