Muhammad Arslan Zahid 1 , Jai Parkash 2 , Chandar Kala 3 , Hafiz Muhammad Furqan Izhar 4 , Zainab Sheikh 5 , Muhammad Abdul Rehman 6
Authors affiliations:
Converting health care to competent clinicians will depend on full teaching plans which connection practice along with theory. Medical education is pretty much a crux in learning clinical skills, critical thinking and decision-making in addition to basic science knowledge for patient care. The goal of this review is to highlight how teaching methodologies such as problem-based learning, simulation and mentor ship accomplish the task of bringing academic knowledge into clinical practice. Good clinical educators should provide more than just a technical skill but the ability to assess and progressively develop to be at least better than baseline as practitioners in teaching future recruits, this way the intern can cope with the modern healthcare system. In addition, the added value of lifelong learning and mentorship to clinical care is highlighted, highlighting how good medical education leads to better health outcomes.
Keywords: Clinical skills; Continuous learning; Critical thinking; Medical education; Problem-based learning (PBL); Professional development; Simulation-based learning; Teaching methodologies.
Citation: Zahid MA, Parkash J, Kala C, Izhar HMF, Sheikh Z, Rehman MA. The essential role of teaching in transforming medical practitioners into effective clinicians. Anaesth. pain intensive care 2026;30(3):370-376. DOI: 10.35975/apic.v30i3.3177
Received: October 02, 2024; Revised: October 26, 2024; Accepted: January 01, 2025
The practice of medicine is an important focus in the provision of healthcare, as it acts as a link between theory and the practical involvement of a physician in patient management. Medical practitioners must possess ample knowledge of the medical sciences and they must be able to utilize such knowledge in the field with its vagaries.1 Caring for a patient also encompasses skills that cannot be acquired from a learning room setting or from the pages of a textbook; such as clinical judgment, communication, compassion, and decision-making under duress, among other things.2 This emphasizes the importance of clinical practice which creates a knowledgeable and self-assured doctor that is geared to work in the healthcare institutions.
Clinical competence serves as one of the keys to the effective delivery of healthcare and this guarantees that the medical professional is able to transpose any theoretic dimension into a clinically-based patient care practice.3 Which entails, the skills set is vast from clinical handling to complexity of thought in regard to emergency management. It is an undeniable fact that as the world becomes more advanced and the patients require better care, the need for trained clinicians who can safely and effectively care for patients is at all times escalating. It is not about practicing the art of medicine; it is the preparation of the mind and body in advance merging the necessary skill and professionalism to the practice of care administration and hence better patient outcomes.
Teaching in medical education is essential for developing the clinical skills of the learners.4 Medical educators help budding practitioners to convert theoretical knowledge into practice through experiences, supervision, and hands-on practice. It is acknowledged that through critical thinking, reasoned diagnosis, and relationship management, teaching helps medical students generate the knowledge and strategize how that knowledge will be used for beneficial use. This review article seeks to highlight how a clinical educator needs to be a teacher and examining how educational methodologies impact clinical performance and patient care. It also recognizes the importance of using proper teaching techniques to integrate theory and practice.5
Being of great assistance in such development are teachers and mentors, who orient students through the field of clinical practice. These educators are important figures in interpreting concepts learned in hypothetical terms into practical solutions and ideas that go beyond what a textbook provides. Acting in such a manner allows students to perceive their future role that involves communicating with the patients, making decisions in clinical settings and providing care while grappling with moral and emotional issues. In a more organized way and by using case-based materials, medical teachers assist garnering critical thoughts, clinical reasoning development, and communication skills pertinent for quality care. The perpetual relationship to teacher in the ground level not only fast tracks the development of skills but nurtures the positive attributes of compassion, which are Canon in training strong clinicians.7
While the effectiveness of PBL in regard to clinical skill development has been demonstrated, this instructional method alone is not sufficient and simulations and hands-on training are also equally important for optimal learning. Simulation-based learning allows students to practice professional skills and patient care in a safe, controlled setting which is arguably the best way to shorten the chasm between classroom knowledge & clinical experience. Students will have increased opportunities to practice technical skills, as well as communicating with patients in a guided setting using high-fidelity mannequins or virtual patients in simulated clinical scenarios with immediate feedback from instructors. Together with the clinical rotations and internships, it forms a continuum of learning that allows students to apply their knowledge to real-world healthcare settings. In these experiential activities, users interact with patients, communicate and coordinate across a healthcare team, and navigate the challenges of diagnosing and treating “patients” with the help of clinical experts.9 These types of teaching methods, using theory in combination with hands-on experience help students to develop the necessary skills and confidence they need before they come face-to-face as clinicians.
Furthermore, learning through an interactive loop of feedback and reflection, supports the interactive process of problem-solving in medicine. So, facilitators are very important in guiding student`s medical practice through doing cases where they can make choice without avoiding the way if anything gets wrong. Teaching prompts students to engage in their clinical decisions critically and consider the options, including consequences of those choices, rather than guiding them down out an algorithmic path through passive learning. It helps polish their ability to think, analyze; on top of that it instigates a culture of continuous learning which is the secret potion to deal with industry-change. The complicated nature of modern clinical medicine is managed by physicians, who are equipped with logical tools as part of their medical training.11
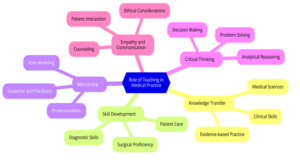
Figure 1: Key Roles of Teaching in Medical Practice
Mentorship goes far beyond simply refining clinical skills and practice patterns. It helps in professional identities of future clinicians.13 The mentor shows the mentee the implications, difficulties and satisfactions of this occupation and therefore contributes in cooperation with human virtues such as empathy, integrity and resilience. The process of observing seniors confront complex ethical dilemmas, manage patients, and interact with others on an expert level serves to mold young doctors into practitioners that carry the norms and values associated with their professional identity. Group learning and teaching with peers establishes a direct connection of experience and knowledge being imparted to the learners by mentors. This is good for building a community, but it also helps to retain and reinforce shorter term understandings of what was learned and the ability to apply them by mentees directed teaching-learning interactions. The team effort mind-set guarantees that the clinical evolution is not an individual venture but it transforms into a more gelled and rounded understanding, knowledge pool through the comprehensive acumen of this academia.
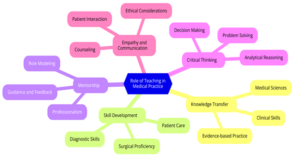
Figure 2: Key Roles of Teaching in Medical Practice
Medicine is understandably a fast paced industry where new research, technologies, and treatment protocols become standard regular practice shortly after they are introduced. With real-time information, this instills a culture of continuous development and enables the practitioner to stay atop the ongoing developments whilst maintaining excellence in clinical practice throughout their career. It promotes the fundamental principle of self-directed learning, which is based on the constructivist learning theory and actively seeking new information, critically reflect on experiences in practice and integrate evidence-based practice into daily work. Continuously examining one's own decisions, outcomes and patient interactions as part of what practitioners call 'reflection on practice', also an important ingredient in a successful clinical experience is becoming a real learning experience.15 The unwavering commitment to Lifelong learning not only serves as the driving force behind our physicians delivering excellent care, but also keeps them limber and nimble to navigate through the continuous flux that characterizes healthcare today.
With patient demands, clinical practice is a fast-paced environment with only limited time for formal teaching. This in turn could mean that, teachers might not be able to adequately mentor and coach their learners the way they should which may effectively ensure that experiential learning and deep reflection go out of window. The first duty to attend a clinical front inevitably consumes their time and energy much of the time leaving them in a persistent tug-of-war between their roles as mentor and teacher.
An interesting barrier is the lack of training provided to the medical educators is to enable them to properly learn about (i.e. teach) this aspect of patient care. Many clinicians are quite talented and know their field very well, but they have not necessarily been specifically trained in an effective way of teaching complex medical concepts.
Consequently they may end up with different levels of teaching quality. Furthermore, the prominent problem of disparity between acquired theoretical information and its application in actuality still exists in medical teaching. Closing this gap requires integrating classroom learning with patients in a manner similar to CBE, but also most educators have had no formal education in how to teach. Addressing these barriers aligned systems that facilitate both patient care provider roles as educator.necessitates more education of clinician-educators, better training to teach and system changes which create clinician-educators, better training to teach and system changes clinician-educators, better training to teach and system changes which create
Over and above, the impact of quality education goes past interaction with the individual patient over time to the entire healthcare system. Trained doctors are useful in improving health care on a bigger scope because they are more capable of managing difficult cases, working with teams of different specialties, and practicing evidence-based medicine.16 Studies have shown that organizations that have a strong education program have fewer complications, shorter length of stay in the hospitals and more patient satisfaction. Quality of medical education enhances healthcare by decreasing medical error and creaing a chain reaction that makes the system better for the future use by creating lifelong practitioners.17
These are the examples that clearly outline hands-on, real-world experience as the connector between theory and practice–turning medical trainees into competent clinicians. Researchers consider a hybrid approach to learning under supervision, as with apprenticeships, workplace-based experiential learning (See One, Do One, Teach One model - used by the Mayo Clinic), as aligning with their proposed pedagogy for SOE.19 This staged exposure teaches trainees autonomy so they are able to adapt decision-making skills and are not held back by technical aptitude. Furthermore, peer teaching during residency positively impacts medical knowledge, communication and leadership skills, thus underlining the necessity of good teaching in clinical training.20
In summary education is the key to the transformation of medical practitioners to integrate professional clinical theoretical knowledge into real pro clinicians and fill up that gap between basic and applied skills. Educators support the development of critical thinking, decision making and patient centered care skills through mentoring, experiential learning and cutting edge pedagogical methods such as problem-based learning and simulations. Professional identity is shaped by both hands-on mentorship and continual trauma education, as we strive to be ever ready for our next large-scale incident. While the challenges of time constraints and the lack of training among faculty to keep up with demand suggest that a renaissance for educational systems and support structures nears novel urgency in preparing the next generation of clinicians capable of navigating today's healthcare system.
The authors declare no financial, personal, or professional relationships could potentially impact the study or conclusions reported in this work.
Authors affiliations:
- Muhammad Arslan Zahid, National Medical Centre, Karachi, Pakistan; Email: dr.arslanzahid@gmail.com
- Jai Parkash, Children Hospital Ireland Crumlin, Ireland; Email: jaiparkash7483@gmail.com
- Chander Kala, Aga Khan University Hospital Karachi. Pakistan; Email: deshamashwari@ymail.com
- Hafiz Muhammad Furqan Izhar, Indus Hospital and Health Network, Karachi, Pakistan; Email: dr.furqanizhar@hotmail.com
- Zainab Sheikh, Islamabad Diagnostic Centre, Islamabad, Pakistan; Email: zainabshykh54@gmail.com
- Muahmmad Abdul Rehman, Bilawal Medical College, LUMHS, Jamshoro, Pakistan; Email: marehman479@gmail.com
ABSTRACT
Converting health care to competent clinicians will depend on full teaching plans which connection practice along with theory. Medical education is pretty much a crux in learning clinical skills, critical thinking and decision-making in addition to basic science knowledge for patient care. The goal of this review is to highlight how teaching methodologies such as problem-based learning, simulation and mentor ship accomplish the task of bringing academic knowledge into clinical practice. Good clinical educators should provide more than just a technical skill but the ability to assess and progressively develop to be at least better than baseline as practitioners in teaching future recruits, this way the intern can cope with the modern healthcare system. In addition, the added value of lifelong learning and mentorship to clinical care is highlighted, highlighting how good medical education leads to better health outcomes.
Keywords: Clinical skills; Continuous learning; Critical thinking; Medical education; Problem-based learning (PBL); Professional development; Simulation-based learning; Teaching methodologies.
Citation: Zahid MA, Parkash J, Kala C, Izhar HMF, Sheikh Z, Rehman MA. The essential role of teaching in transforming medical practitioners into effective clinicians. Anaesth. pain intensive care 2026;30(3):370-376. DOI: 10.35975/apic.v30i3.3177
Received: October 02, 2024; Revised: October 26, 2024; Accepted: January 01, 2025
1. INTRODUCTION
The practice of medicine is an important focus in the provision of healthcare, as it acts as a link between theory and the practical involvement of a physician in patient management. Medical practitioners must possess ample knowledge of the medical sciences and they must be able to utilize such knowledge in the field with its vagaries.1 Caring for a patient also encompasses skills that cannot be acquired from a learning room setting or from the pages of a textbook; such as clinical judgment, communication, compassion, and decision-making under duress, among other things.2 This emphasizes the importance of clinical practice which creates a knowledgeable and self-assured doctor that is geared to work in the healthcare institutions.
Clinical competence serves as one of the keys to the effective delivery of healthcare and this guarantees that the medical professional is able to transpose any theoretic dimension into a clinically-based patient care practice.3 Which entails, the skills set is vast from clinical handling to complexity of thought in regard to emergency management. It is an undeniable fact that as the world becomes more advanced and the patients require better care, the need for trained clinicians who can safely and effectively care for patients is at all times escalating. It is not about practicing the art of medicine; it is the preparation of the mind and body in advance merging the necessary skill and professionalism to the practice of care administration and hence better patient outcomes.
Teaching in medical education is essential for developing the clinical skills of the learners.4 Medical educators help budding practitioners to convert theoretical knowledge into practice through experiences, supervision, and hands-on practice. It is acknowledged that through critical thinking, reasoned diagnosis, and relationship management, teaching helps medical students generate the knowledge and strategize how that knowledge will be used for beneficial use. This review article seeks to highlight how a clinical educator needs to be a teacher and examining how educational methodologies impact clinical performance and patient care. It also recognizes the importance of using proper teaching techniques to integrate theory and practice.5
- Medical Education and Clinical Development:
Being of great assistance in such development are teachers and mentors, who orient students through the field of clinical practice. These educators are important figures in interpreting concepts learned in hypothetical terms into practical solutions and ideas that go beyond what a textbook provides. Acting in such a manner allows students to perceive their future role that involves communicating with the patients, making decisions in clinical settings and providing care while grappling with moral and emotional issues. In a more organized way and by using case-based materials, medical teachers assist garnering critical thoughts, clinical reasoning development, and communication skills pertinent for quality care. The perpetual relationship to teacher in the ground level not only fast tracks the development of skills but nurtures the positive attributes of compassion, which are Canon in training strong clinicians.7
- Pedagogical Approaches in Medical Training:
While the effectiveness of PBL in regard to clinical skill development has been demonstrated, this instructional method alone is not sufficient and simulations and hands-on training are also equally important for optimal learning. Simulation-based learning allows students to practice professional skills and patient care in a safe, controlled setting which is arguably the best way to shorten the chasm between classroom knowledge & clinical experience. Students will have increased opportunities to practice technical skills, as well as communicating with patients in a guided setting using high-fidelity mannequins or virtual patients in simulated clinical scenarios with immediate feedback from instructors. Together with the clinical rotations and internships, it forms a continuum of learning that allows students to apply their knowledge to real-world healthcare settings. In these experiential activities, users interact with patients, communicate and coordinate across a healthcare team, and navigate the challenges of diagnosing and treating “patients” with the help of clinical experts.9 These types of teaching methods, using theory in combination with hands-on experience help students to develop the necessary skills and confidence they need before they come face-to-face as clinicians.
- Teaching as a Tool for Critical Thinking and Problem-Solving:
Furthermore, learning through an interactive loop of feedback and reflection, supports the interactive process of problem-solving in medicine. So, facilitators are very important in guiding student`s medical practice through doing cases where they can make choice without avoiding the way if anything gets wrong. Teaching prompts students to engage in their clinical decisions critically and consider the options, including consequences of those choices, rather than guiding them down out an algorithmic path through passive learning. It helps polish their ability to think, analyze; on top of that it instigates a culture of continuous learning which is the secret potion to deal with industry-change. The complicated nature of modern clinical medicine is managed by physicians, who are equipped with logical tools as part of their medical training.11

Figure 1: Key Roles of Teaching in Medical Practice
- The Impact of Mentorship and Coaching in Clinical Growth:
Mentorship goes far beyond simply refining clinical skills and practice patterns. It helps in professional identities of future clinicians.13 The mentor shows the mentee the implications, difficulties and satisfactions of this occupation and therefore contributes in cooperation with human virtues such as empathy, integrity and resilience. The process of observing seniors confront complex ethical dilemmas, manage patients, and interact with others on an expert level serves to mold young doctors into practitioners that carry the norms and values associated with their professional identity. Group learning and teaching with peers establishes a direct connection of experience and knowledge being imparted to the learners by mentors. This is good for building a community, but it also helps to retain and reinforce shorter term understandings of what was learned and the ability to apply them by mentees directed teaching-learning interactions. The team effort mind-set guarantees that the clinical evolution is not an individual venture but it transforms into a more gelled and rounded understanding, knowledge pool through the comprehensive acumen of this academia.

Figure 2: Key Roles of Teaching in Medical Practice
- Continuing Education and Lifelong Learning:
Medicine is understandably a fast paced industry where new research, technologies, and treatment protocols become standard regular practice shortly after they are introduced. With real-time information, this instills a culture of continuous development and enables the practitioner to stay atop the ongoing developments whilst maintaining excellence in clinical practice throughout their career. It promotes the fundamental principle of self-directed learning, which is based on the constructivist learning theory and actively seeking new information, critically reflect on experiences in practice and integrate evidence-based practice into daily work. Continuously examining one's own decisions, outcomes and patient interactions as part of what practitioners call 'reflection on practice', also an important ingredient in a successful clinical experience is becoming a real learning experience.15 The unwavering commitment to Lifelong learning not only serves as the driving force behind our physicians delivering excellent care, but also keeps them limber and nimble to navigate through the continuous flux that characterizes healthcare today.
- Effective Clinician Development through Teaching:
- Challenges in the Integration of Teaching and Clinical Practice:
With patient demands, clinical practice is a fast-paced environment with only limited time for formal teaching. This in turn could mean that, teachers might not be able to adequately mentor and coach their learners the way they should which may effectively ensure that experiential learning and deep reflection go out of window. The first duty to attend a clinical front inevitably consumes their time and energy much of the time leaving them in a persistent tug-of-war between their roles as mentor and teacher.
An interesting barrier is the lack of training provided to the medical educators is to enable them to properly learn about (i.e. teach) this aspect of patient care. Many clinicians are quite talented and know their field very well, but they have not necessarily been specifically trained in an effective way of teaching complex medical concepts.
Consequently they may end up with different levels of teaching quality. Furthermore, the prominent problem of disparity between acquired theoretical information and its application in actuality still exists in medical teaching. Closing this gap requires integrating classroom learning with patients in a manner similar to CBE, but also most educators have had no formal education in how to teach. Addressing these barriers aligned systems that facilitate both patient care provider roles as educator.necessitates more education of clinician-educators, better training to teach and system changes which create clinician-educators, better training to teach and system changes clinician-educators, better training to teach and system changes which create
- Impact of Effective Teaching on Patient Care:
Over and above, the impact of quality education goes past interaction with the individual patient over time to the entire healthcare system. Trained doctors are useful in improving health care on a bigger scope because they are more capable of managing difficult cases, working with teams of different specialties, and practicing evidence-based medicine.16 Studies have shown that organizations that have a strong education program have fewer complications, shorter length of stay in the hospitals and more patient satisfaction. Quality of medical education enhances healthcare by decreasing medical error and creaing a chain reaction that makes the system better for the future use by creating lifelong practitioners.17
- Case Studies of Effective Teaching Practices in Clinical Settings:
These are the examples that clearly outline hands-on, real-world experience as the connector between theory and practice–turning medical trainees into competent clinicians. Researchers consider a hybrid approach to learning under supervision, as with apprenticeships, workplace-based experiential learning (See One, Do One, Teach One model - used by the Mayo Clinic), as aligning with their proposed pedagogy for SOE.19 This staged exposure teaches trainees autonomy so they are able to adapt decision-making skills and are not held back by technical aptitude. Furthermore, peer teaching during residency positively impacts medical knowledge, communication and leadership skills, thus underlining the necessity of good teaching in clinical training.20
11. CONCLUSION
In summary education is the key to the transformation of medical practitioners to integrate professional clinical theoretical knowledge into real pro clinicians and fill up that gap between basic and applied skills. Educators support the development of critical thinking, decision making and patient centered care skills through mentoring, experiential learning and cutting edge pedagogical methods such as problem-based learning and simulations. Professional identity is shaped by both hands-on mentorship and continual trauma education, as we strive to be ever ready for our next large-scale incident. While the challenges of time constraints and the lack of training among faculty to keep up with demand suggest that a renaissance for educational systems and support structures nears novel urgency in preparing the next generation of clinicians capable of navigating today's healthcare system.
- Conflict of Interest:
The authors declare no financial, personal, or professional relationships could potentially impact the study or conclusions reported in this work.
- Authors contribution
15. REFERENCES
- Bilal M, Haseeb A, Mari A, Ahmed S, Sher Khan MA, Saad M. Knowledge, Attitudes, and Barriers Toward Research Among Medical Students of Karachi. Cureus. 2019;11(9):e5599. PMID: 31700712 PMCID: PMC6822902 DOI: 7759/cureus.5599
- Babaii A, Mohammadi E, Sadooghiasl A. The Meaning of the Empathetic Nurse-Patient Communication: A Qualitative Study. Journal of patient experience. 2021;8:23743735211056432. PMID: 34869836 PMCID: PMC8640307 DOI: 1177/23743735211056432
- Hui T, Zakeri MA, Soltanmoradi Y, Rahimi N, Hossini Rafsanjanipoor SM, Nouroozi M, et al. Nurses' clinical competency and its correlates: before and during the COVID-19 outbreak. BMC nursing. 2023;22(1):156. PMID: 3714965 PMCID: PMC10163958 DOI: 1186/s12912-023-01330-9
- Spencer J. Learning and teaching in the clinical environment. BMJ (Clinical research ed). 2003;326(7389):591-4. PMID: 12637408 PMCID: PMC1125480 DOI: 10.1136/bmj.326.7389.591
- Gcawu SN, van Rooyen D. Clinical teaching practices of nurse educators: An integrative literature review. Health SA = SA Gesondheid. 2022;27:1728. PMCID: PMC9575343 PMID: 36262921 doi: 4102/hsag.v27i0.1728
- Hashemiparast M, Negarandeh R, Theofanidis D. Exploring the barriers of utilizing theoretical knowledge in clinical settings: A qualitative study. International journal of nursing sciences. 2019;6(4):399-405. PMID: 31728392 PMCID: PMC6838863 DOI: 1016/j.ijnss.2019.09.008
- Wang X. Exploring positive teacher-student relationships: the synergy of teacher mindfulness and emotional intelligence. Frontiers in psychology. 2023;14:1301786. PMCID: PMC10716249 PMID: 38094701 doi: 3389/fpsyg.2023.1301786
- Lim WK. Problem Based Learning in Medical Education: Handling Objections and Sustainable Implementation. Advances in medical education and practice. 2023;14:1453-60.
- Buljac-Samardzic M, Doekhie KD, van Wijngaarden JDH. Interventions to improve team effectiveness within health care: a systematic review of the past decade. Human resources for health. 2020;18(1):2.
- Ho YR, Chen BY, Li CM. Thinking more wisely: using the Socratic method to develop critical thinking skills amongst healthcare students. BMC medical education. 2023;23(1):173.
- Medina MS, Castleberry AN, Persky AM. Strategies for Improving Learner Metacognition in Health Professional Education. American journal of pharmaceutical education. 2017;81(4):78.
- Treasure AM, Hall SM, Lesko I, Moore D, Sharan M, van Zaanen M, et al. Ten simple rules for establishing a mentorship programme. PLoS computational biology. 2022;18(5):e1010015.
- Choi AMK, Moon JE, Steinecke A, Prescott JE. Developing a Culture of Mentorship to Strengthen Academic Medical Centers. Academic medicine: journal of the Association of American Medical Colleges. 2019;94(5):630-3.
- Forsetlund L, O'Brien MA, Forsén L, Reinar LM, Okwen MP, Horsley T, et al. Continuing education meetings and workshops: effects on professional practice and healthcare outcomes. The Cochrane database of systematic reviews. 2021;9(9):Cd003030.
- Koshy K, Limb C, Gundogan B, Whitehurst K, Jafree DJ. Reflective practice in health care and how to reflect effectively. International journal of surgery Oncology. 2017;2(6):e20.
- Pitsillidou M, Roupa Z, Farmakas A, Noula M. Factors Affecting the Application and Implementation of Evidence-based Practice in Nursing. Acta informatica medica : AIM : journal of the Society for Medical Informatics of Bosnia & Herzegovina : casopis Drustva za medicinsku informatiku BiH. 2021;29(4):281-7.
- McGaghie WC, Barsuk JH, Wayne DB, Issenberg SB. Powerful medical education improves health care quality and return on investment. Medical teacher. 2024;46(1):46-58.
- Al-Elq AH. Simulation-based medical teaching and learning. Journal of family & community medicine. 2010;17(1):35-40.
- Kotsis SV, Chung KC. Application of the "see one, do one, teach one" concept in surgical training. Plastic and reconstructive surgery. 2013;131(5):1194-201.
- Conner SM, Choi N, Fuller J, Daya S, Barish P, Rennke S, et al. Trainee Autonomy and Supervision in the Modern Clinical Learning Environment: A Mixed-Methods Study of Faculty and Trainee Perspectives. Research square. 2023.