Uday Gollamudi 1, Pravallika Rallapalli 2, R. S. Sachidananad 3
Authors affiliations:
The advent of video laryngoscopy (VL) has significantly improved the safety and efficacy of difficult airway management. Among the various VL devices available, the D-Blade of the C-MAC videolaryngoscope (VLS) has proven to be an invaluable tool, particularly in challenging scenarios. This case series highlights five unique, complex clinical scenarios involving patients with difficult airways, where the D-Blade of the C-MAC VLS facilitated successful intubation and contributed to better patient outcomes. We discuss each case, the challenges encountered, and the role of the D-Blade in overcoming these obstacles. Furthermore, we underscore the importance of further research to assess its broader applicability and potential in diverse clinical settings.
Abbreviations: ETT: endotracheal tube, PACU: post-anesthesia care unit, RTA: road traffic accident, VLS: Videolaryngoscope,
Keywords: Videolaryngoscope; C-Mac; D-blade; Difficult intubation
Citation: Gollamudi U, Rallapalli P. Sachidananad RS. The D-Blade of the C-MAC videolaryngoscope in airway management: a case series of five challenging intubations. Anaesth. pain intensive care 2025;29(3):720-725. DOI: 10.35975/apic.v29i3.2773
Received: February 23, 2025; Revised: March 13, 2025; Accepted: March 24, 2025
Airway management is a critical aspect of anesthesia, with difficult intubation being a significant cause of morbidity and mortality. Difficult airway management remains a challenge despite the invention of many novel airway devices, even in the hands of experienced anesthesiologists.1 Traditional direct laryngoscopy may be ineffective in patients with challenging anatomical features, such as limited neck mobility, obesity, reduced mouth opening, or airway distortions. While awake, flexible bronchoscopic intubation has long been considered the gold standard for managing anticipated difficult airways, the videolaryngoscope has emerged as a viable alternative.2 The use of videolaryngoscopes (VLS) such as the C Mac have increased over the past few years leading to a significant decrease in the number of awake fiberoptic intubations.3 VLS were designed to overcome the limitations associated with direct laryngoscopes and have shown great success in all scenarios of routine, emergency, and difficult airways.4 It has become a key tool in offering enhanced visualization and greater success rates in intubation. Videolaryngoscopy is an evolutionary step that involves the use of video and optical technology to provide a non-line of-sight view of the larynx. It yields a superior image of the larynx with a higher success rate, especially in difficult situations.5
Some VLSs (e.g., GlideScope and McGrath) do not provide visualization of the tip of the blade and, therefore, demand a tube stylet to guide the endotracheal tube (ETT) through the glottis.6
The C-MAC VLS, particularly with its D-Blade, has proven to be invaluable for managing difficult airways. The D-Blade features a unique design with a curved angulation that facilitates improved glottic visualization. It is specifically engineered to provide an optimal view of the vocal cords, even in patients with challenging airway anatomy. The D-Blade offers a range of viewing angles—typically between 60 to 80 degrees—which allows for a direct line of sight to the glottis, even in cases of limited neck mobility or anatomical obstructions. This enhanced visualization reduces the need for excessive manipulation, decreasing the risk of trauma, aspiration, and other complications.
This case series presents five distinct and complex airway scenarios, demonstrating the utility of the D-Blade in improving intubation outcomes. These cases cover a variety of difficult airway challenges, including acromegaly, morbid obesity, reduced mouth opening, cervical spine trauma, and large thyroid masses. In each case, the D-Blade facilitated a smooth and successful intubation, highlighting its effectiveness in managing high-risk airways.

Figure 1: D-Blade of the C-MAC VLS
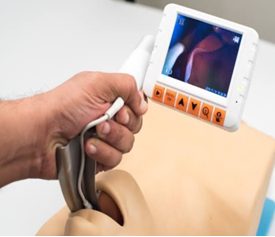
Figure 2: D-Blade of the C-MAC VLS in use
2.1. Case 1
A 55-year-old male with a known history of acromegaly was scheduled for a laparoscopic cholecystectomy. He also had a history of sleep apnea and was classified as ASA physical status III. His preoperative airway assessment revealed enlarged soft tissues, a thickened tongue, and a prominent jaw, all typical features of acromegaly. His Mallampati score was III, and neck mobility was reduced, raising significant concerns for difficult intubation. With these anatomical challenges, visualization of the glottis with a traditional laryngoscope would likely have been difficult, with a higher risk of failed intubation or airway trauma. Given the patient's airway characteristics and the anticipated difficulty in visualization, the D-Blade of the C-MAC VLS was chosen.
Intraoperatively, after the patient was pre-oxygenated and induced, the D-Blade was carefully inserted into his mouth. With minimal manipulation, the blade’s optimized angulation (60-80 degrees) allowed for a clear, unobstructed view of the glottis. The real-time video feedback from the C-MAC system enabled accurate visualization of the vocal cords, and the ETT was successfully advanced into the trachea on the first attempt. The entire process was smooth, with no complications such as trauma, hypoxia, or aspiration.
The surgery proceeded without any further issues. After the laparoscopic cholecystectomy was completed successfully, the patient was extubated smoothly and shifted to the post-anesthesia care unit (PACU) for recovery. The procedure concluded uneventfully, and the patient was monitored closely in the PACU until he regained full consciousness and stable vital signs.
2.2. Case 2
A 45-year-old female with morbid obesity (BMI 42 kg/m2) and a short neck was scheduled for a laparoscopic abdominal hysterectomy. Her preoperative assessment revealed a Mallampati score of IV and limited neck extension, both of which suggested a potentially difficult airway. The short neck combined with excessive adipose tissue raised concerns about obtaining adequate glottic visualization using conventional direct laryngoscopy. The risk of airway obstruction during intubation was high due to the patient’s anatomical features, making airway management challenging. Because of the anticipated difficulty in visualizing the glottis with a standard laryngoscope, the C-MAC D-Blade VLS was chosen for intubation.
In the operating room, after the patient was adequately preoxygenated and induced, the D-Blade was introduced into the patient’s mouth. Thanks to the larger angulation of the D-Blade, a clear view of the glottis was achieved without the need for excessive manipulation. The video screen provided real-time feedback, ensuring accurate placement of the ETT, which was successfully inserted on the first attempt. The entire procedure was smooth, with no complications such as trauma or difficulty in securing the airway. Following successful intubation, the patient was positioned for the laparoscopic abdominal hysterectomy, which proceeded without any issues. After the surgery, the patient was extubated smoothly and transferred to the PACU for recovery. The procedure concluded uneventfully, and the patient was closely monitored as she regained full consciousness and stable vital signs.
2.3. Case 3
A 65-year-old male with squamous cell carcinoma of the right buccal mucosa was scheduled for tumor resection and neck dissection. The patient’s airway assessment revealed a reduced mouth opening of approximately 1.5 fingers, which posed a significant challenge for intubation using traditional laryngoscopy. Additionally, the patient had restricted neck mobility due to both the tumor mass and previous radiation therapy, further complicating the airway management. These factors combined to increase the likelihood of difficult intubation, with concerns about airway obstruction and inadequate glottic visualization. Due to the reduced mouth opening and limited neck movement, intubation with a direct laryngoscope would likely be difficult. The C-MAC D-Blade VLS was chosen due to its ability to provide enhanced glottic visualization in such challenging cases.
After pre-oxygenation and induction, the D-Blade was introduced into the patient's mouth. Despite the limited mouth opening, the blade's angulated design allowed for a clear view of the glottis, even through the narrow oral opening. The video feed from the C-MAC system enabled precise visualization, allowing for the successful placement of the ETT on the first attempt without the need for additional maneuvers. There were no complications such as airway trauma, aspiration, or hypoxia.
After securing the airway, the patient was positioned for tumor resection and neck dissection, which proceeded uneventfully. Following the completion of the surgery, the patient was extubated safely and transferred to the PACU for monitoring. The procedure ended without complications, and the patient was stable postoperatively.
2.4. Case 4
A 35-year-old male was involved in a road traffic accident (RTA) and sustained multiple fractures, including a cervical spine fracture was posted for open reduction and internal fixation (ORIF) of the mandible fracture. Due to the nature of the injury, the patient had significant neck immobility, and his airway was considered potentially difficult due to restricted cervical motion and a history of mild dysphagia. The limited neck mobility from the cervical spine injury, combined with potential airway swelling and trauma, significantly increased the difficulty of performing intubation. The airway assessment revealed the possibility of both difficult visualization and potential airway obstruction due to the trauma, making intubation using a standard laryngoscope more challenging. Given these concerns, the C-MAC D-Blade VLS was selected for intubation.
After stabilizing the cervical spine appropriate induction agent and muscle relaxation were administered and the D-Blade was gently introduced. Despite the restricted cervical motion, the blade's angled design allowed for improved visualization of the glottis. The video feedback from the C-MAC system provided real-time assistance in guiding the placement of the ETT via nasotracheal route which was successfully completed on the first attempt. There were no complications such as trauma to the airway structures.
Following the successful intubation, the patient underwent ORIF of the mandible fracture. After the surgery was completed without further complications, the patient was extubated smoothly and transferred to the PACU for recovery and monitoring.
2.5. Case 5
A 60-year-old female with a large thyroid mass (9×5cm) was scheduled for a total thyroidectomy. The mass had caused significant tracheal deviation, and the patient also reported a history of dysarthria and dysphagia. Given the size of the mass, the airway was potentially compromised, with concerns about tracheal compression and risk of airway obstruction during intubation. The airway evaluation raised concerns about difficulty using standard laryngoscopy, as the mass could interfere with conventional blade angulation and compromise glottic visualization. To manage the anticipated difficult airway, the D-Blade of the C-MAC VLS was selected.
After administering appropriate induction agent and ensuring the patient's airway was adequately prepared, the D-Blade was introduced into the mouth. Despite the tracheal deviation and limited space due to the mass, the D-Blade’s angulation allowed for excellent visualization of the airway structures. The video feed from the C-MAC system provided real-time guidance, allowing the operator to precisely place the ETT. The intubation was successfully completed on the first attempt, with no complications such as airway trauma or difficulty in securing the airway.
Following the successful intubation, the patient underwent total thyroidectomy without further issues. The surgery proceeded uneventfully, and after the procedure, the patient was extubated smoothly and transferred to the PACU for recovery. The patient remained stable throughout the postoperative period and was monitored closely for any signs of airway compromise.
In all these cases intra venous midazolam 0.2 mg/kg and glycopyrrolate 0.2 mg as premedication, Fentanyl 1.5 mcg/kg for analgesia, propofol 1.2 mg/kg was used as induction agent, short acting depolarising muscle relaxant succinyl choline 1 mg/kg was given for muscle relaxation and the patient was maintained on isoflurane and intermittent dosages of Atracurium throughout the intraoperative period and before extubation Neostigmine and glycopyrrolate were given for reversal.
Prediction of difficult intubation can be possible using physical characteristics such as obesity, restricted mandibular protrusion, higher Mallampati classification, short thyromental distance, and immobility of the neck. However, anatomical abnormalities involving the larynx and trachea are frequently asymptomatic and can remain unsuspected until difficult tracheal intubation during anesthesia.7 However, several patients of apparently normal appearance unexpectedly present great difficulties at intubation. A study of anatomical factors in these patients should improve ability to predict and manage a potential failed intubation. When an experienced operator fails in two attempts at direct laryngoscope-assisted intubation, the case can be viewed as a difficult intubation case. If mask ventilation is possible, other airway management devices may be considered. Recently, clinical application of video laryngoscopy has been very helpful in resolving difficult intubation cases.8
The D-Blade of the C-MAC VLS has proven to be an invaluable tool in managing difficult airways, offering significant advantages over traditional intubation techniques. In this case series, we demonstrated its efficacy across five challenging clinical scenarios, where conventional laryngoscopy might have failed due to anatomical abnormalities, reduced mouth opening, limited neck mobility, and airway obstruction.
The D blade is specifically designed for the difficult airway. It can be used in both anesthetized and awake patients. With its flat profile and elliptically shaped blade, it can be glided along the tongue to guide the user directly to the epiglottis. Particularly when it comes to difficult intubation Cormack Lehane III and IV, the D blade enables successful intubation.3 One of the primary benefits of the D-Blade is its optimized angulation, providing an improved view of the glottis by offering an angle of 60-80 degrees, even in patients with anatomical challenges. This direct line of sight reduces the need for excessive manipulation and minimizes risks such as trauma, aspiration, and hypoxia. In all five cases, the D-Blade facilitated successful intubation, allowing for clear visualization of the vocal cords, even in patients with severe restrictions in neck movement or mouth opening.
The real-time video feedback provided by the C-MAC system is another crucial advantage. It allows for continuous visual assessment during intubation, helping the operator make adjustments for precise placement, which is particularly important in high-risk scenarios. The ability to see the airway structures on a video screen also promotes better team coordination and assists in training new clinicians.
While a VLS generally improves intubation success rates, their optimal use requires familiarity with the device and the ability to interpret the video feed accurately. Proper training is essential for maximizing the benefits of this technology, as inexperienced operators may struggle with the device’s unique angulation or video output. The advantage of using the VLS in relation to the Macintosh metal blade is that there is no need to align the pharyngeal and laryngeal axes during the laryngoscopy maneuver. Therefore, the VLS is a great option in scenarios in which there are factors suggesting the presence of difficult airway.4 However, several patients of apparently normal appearance unexpectedly present great difficulties at intubation. A study of anatomical factors in these patients should improve ability to predict and manage a potential failed intubation.9
The use of VLSs like the C-MAC system has been shown to enhance patient safety in difficult airway management. Studies indicate that video laryngoscopy improves first-attempt success rates, reduces complications, and offers greater precision compared to direct laryngoscopy, particularly in patients with challenging anatomies or in emergency situations.
Patients that could be intubated directly without difficulty or using only external laryngeal manipulation are more with D‑Blade. Use of accessory maneuvers such as tube rotation, partial inflation of cuff, and use of forceps were less with D‑Blade than Macintosh laryngoscope.4
It was easy to insert the C-MAC, to obtain a view of the glottis, and to intubate the trachea, without major complications. Because the shape of the blade is similar to the original Macintosh blade, using a tube stylet is not required.6 The use of the C-MAC VL in the setting of an anticipated difficult airway with Mallampati grade 3 and 4 should lead to a higher rate of successful intubation when compared with McCoy laryngoscopy.11 D-Blade VLS causes less dental compression compared to Macintosh and especially the conventional C-MAC VLS.12 C-MAC D-Blade videolaryngoscope had significant benefits for intubation time and difficulty compared to the McCoy laryngoscopy during nasotracheal intubation. It provided for better glottic visualization and it took less time to advance the nasotracheal tube from the oropharynx to the glottic inlet with this device.13 C-MAC VLS-aided intubations using D-blade significantly reduced the incidence and severity of post-operative sore throat, hoarseness of voice, and cough following orotracheal intubation as compared to use of traditional Macintosh laryngoscope.13 There was no significant difference in terms of sympathetic stimulation between Macintosh and C-MAC D-Blade videolaryngoscope.4
Despite its advantages, some limitations remain, such as its higher cost and potential reduced effectiveness in patients with extreme anatomical challenges. Additionally, the widespread adoption of VLSs may be limited in resource-constrained settings. In contrast to many previous VLS’s, the C-MAC has the unique advantage of obtaining both a direct laryngoscopic view and a camera view that are displayed on the video screen. On one hand, this may be very helpful for educational purposes, because the instructor may follow the student’s intubation attempts directly on the video screen.6
Further research is needed to evaluate the comparative effectiveness of the D-Blade against other VLSs and direct laryngoscopy, especially in emergency settings. Large-scale studies could also assess its impact on long-term patient outcomes, including airway trauma and post-intubation complications.
The D-Blade of the C-MAC video laryngoscope is a highly effective tool for managing difficult airways, providing superior glottic visualization and improving intubation success in complex scenarios. While operator proficiency is essential, its integration into routine airway management is likely to improve safety and outcomes, particularly in high-risk cases. Further studies are necessary to fully understand its broader applications and effectiveness.
5. Ethical considerations
Ethical approval was obtained from the institutional ethical committee. Written consent was obtained from every patient to use and publish the data for the academic interest.
6. Conflict of interest
All authors declare that there was no conflict of interest.
7. Funding
The study utilized the hospital resources only, and no external or industry funding was involved.
8. Authors’ contribution
UG: Concepts, Design, Literature search, Data acquisition, Manuscript preparation
PR: Concepts, Design, Literature search, Data analysis, Editing
SRS: Concepts, Design,
Authors affiliations:
- Uday Gollamudi, Associate Professor, Apollo Institute of Medical Sciences & Research, Hyderabad, Telangana, India; Email: gollamudiudayreddy@gmail.com; {ORCID:0000-0002-8509-3546}
- Pravallika Rallapalli, Junior Resident, Apollo Institute of Medical Sciences & Research, Hyderabad, Telangana, India; Email: rallapallipravallika@gmail.com; {ORCID:0009-0003-4079-3551}
- R. S. Sachidananad, Professor and Head of Department, , Apollo Institute of Medical Sciences & Research, Hyderabad, Telangana, India; Email: rachmalla@yahoo.com
ABSTRACT
The advent of video laryngoscopy (VL) has significantly improved the safety and efficacy of difficult airway management. Among the various VL devices available, the D-Blade of the C-MAC videolaryngoscope (VLS) has proven to be an invaluable tool, particularly in challenging scenarios. This case series highlights five unique, complex clinical scenarios involving patients with difficult airways, where the D-Blade of the C-MAC VLS facilitated successful intubation and contributed to better patient outcomes. We discuss each case, the challenges encountered, and the role of the D-Blade in overcoming these obstacles. Furthermore, we underscore the importance of further research to assess its broader applicability and potential in diverse clinical settings.
Abbreviations: ETT: endotracheal tube, PACU: post-anesthesia care unit, RTA: road traffic accident, VLS: Videolaryngoscope,
Keywords: Videolaryngoscope; C-Mac; D-blade; Difficult intubation
Citation: Gollamudi U, Rallapalli P. Sachidananad RS. The D-Blade of the C-MAC videolaryngoscope in airway management: a case series of five challenging intubations. Anaesth. pain intensive care 2025;29(3):720-725. DOI: 10.35975/apic.v29i3.2773
Received: February 23, 2025; Revised: March 13, 2025; Accepted: March 24, 2025
1. INTRODUCTION
Airway management is a critical aspect of anesthesia, with difficult intubation being a significant cause of morbidity and mortality. Difficult airway management remains a challenge despite the invention of many novel airway devices, even in the hands of experienced anesthesiologists.1 Traditional direct laryngoscopy may be ineffective in patients with challenging anatomical features, such as limited neck mobility, obesity, reduced mouth opening, or airway distortions. While awake, flexible bronchoscopic intubation has long been considered the gold standard for managing anticipated difficult airways, the videolaryngoscope has emerged as a viable alternative.2 The use of videolaryngoscopes (VLS) such as the C Mac have increased over the past few years leading to a significant decrease in the number of awake fiberoptic intubations.3 VLS were designed to overcome the limitations associated with direct laryngoscopes and have shown great success in all scenarios of routine, emergency, and difficult airways.4 It has become a key tool in offering enhanced visualization and greater success rates in intubation. Videolaryngoscopy is an evolutionary step that involves the use of video and optical technology to provide a non-line of-sight view of the larynx. It yields a superior image of the larynx with a higher success rate, especially in difficult situations.5
Some VLSs (e.g., GlideScope and McGrath) do not provide visualization of the tip of the blade and, therefore, demand a tube stylet to guide the endotracheal tube (ETT) through the glottis.6
The C-MAC VLS, particularly with its D-Blade, has proven to be invaluable for managing difficult airways. The D-Blade features a unique design with a curved angulation that facilitates improved glottic visualization. It is specifically engineered to provide an optimal view of the vocal cords, even in patients with challenging airway anatomy. The D-Blade offers a range of viewing angles—typically between 60 to 80 degrees—which allows for a direct line of sight to the glottis, even in cases of limited neck mobility or anatomical obstructions. This enhanced visualization reduces the need for excessive manipulation, decreasing the risk of trauma, aspiration, and other complications.
This case series presents five distinct and complex airway scenarios, demonstrating the utility of the D-Blade in improving intubation outcomes. These cases cover a variety of difficult airway challenges, including acromegaly, morbid obesity, reduced mouth opening, cervical spine trauma, and large thyroid masses. In each case, the D-Blade facilitated a smooth and successful intubation, highlighting its effectiveness in managing high-risk airways.

Figure 1: D-Blade of the C-MAC VLS

Figure 2: D-Blade of the C-MAC VLS in use
2. CASE SERIES
2.1. Case 1
A 55-year-old male with a known history of acromegaly was scheduled for a laparoscopic cholecystectomy. He also had a history of sleep apnea and was classified as ASA physical status III. His preoperative airway assessment revealed enlarged soft tissues, a thickened tongue, and a prominent jaw, all typical features of acromegaly. His Mallampati score was III, and neck mobility was reduced, raising significant concerns for difficult intubation. With these anatomical challenges, visualization of the glottis with a traditional laryngoscope would likely have been difficult, with a higher risk of failed intubation or airway trauma. Given the patient's airway characteristics and the anticipated difficulty in visualization, the D-Blade of the C-MAC VLS was chosen.
Intraoperatively, after the patient was pre-oxygenated and induced, the D-Blade was carefully inserted into his mouth. With minimal manipulation, the blade’s optimized angulation (60-80 degrees) allowed for a clear, unobstructed view of the glottis. The real-time video feedback from the C-MAC system enabled accurate visualization of the vocal cords, and the ETT was successfully advanced into the trachea on the first attempt. The entire process was smooth, with no complications such as trauma, hypoxia, or aspiration.
The surgery proceeded without any further issues. After the laparoscopic cholecystectomy was completed successfully, the patient was extubated smoothly and shifted to the post-anesthesia care unit (PACU) for recovery. The procedure concluded uneventfully, and the patient was monitored closely in the PACU until he regained full consciousness and stable vital signs.
2.2. Case 2
A 45-year-old female with morbid obesity (BMI 42 kg/m2) and a short neck was scheduled for a laparoscopic abdominal hysterectomy. Her preoperative assessment revealed a Mallampati score of IV and limited neck extension, both of which suggested a potentially difficult airway. The short neck combined with excessive adipose tissue raised concerns about obtaining adequate glottic visualization using conventional direct laryngoscopy. The risk of airway obstruction during intubation was high due to the patient’s anatomical features, making airway management challenging. Because of the anticipated difficulty in visualizing the glottis with a standard laryngoscope, the C-MAC D-Blade VLS was chosen for intubation.
In the operating room, after the patient was adequately preoxygenated and induced, the D-Blade was introduced into the patient’s mouth. Thanks to the larger angulation of the D-Blade, a clear view of the glottis was achieved without the need for excessive manipulation. The video screen provided real-time feedback, ensuring accurate placement of the ETT, which was successfully inserted on the first attempt. The entire procedure was smooth, with no complications such as trauma or difficulty in securing the airway. Following successful intubation, the patient was positioned for the laparoscopic abdominal hysterectomy, which proceeded without any issues. After the surgery, the patient was extubated smoothly and transferred to the PACU for recovery. The procedure concluded uneventfully, and the patient was closely monitored as she regained full consciousness and stable vital signs.
2.3. Case 3
A 65-year-old male with squamous cell carcinoma of the right buccal mucosa was scheduled for tumor resection and neck dissection. The patient’s airway assessment revealed a reduced mouth opening of approximately 1.5 fingers, which posed a significant challenge for intubation using traditional laryngoscopy. Additionally, the patient had restricted neck mobility due to both the tumor mass and previous radiation therapy, further complicating the airway management. These factors combined to increase the likelihood of difficult intubation, with concerns about airway obstruction and inadequate glottic visualization. Due to the reduced mouth opening and limited neck movement, intubation with a direct laryngoscope would likely be difficult. The C-MAC D-Blade VLS was chosen due to its ability to provide enhanced glottic visualization in such challenging cases.
After pre-oxygenation and induction, the D-Blade was introduced into the patient's mouth. Despite the limited mouth opening, the blade's angulated design allowed for a clear view of the glottis, even through the narrow oral opening. The video feed from the C-MAC system enabled precise visualization, allowing for the successful placement of the ETT on the first attempt without the need for additional maneuvers. There were no complications such as airway trauma, aspiration, or hypoxia.
After securing the airway, the patient was positioned for tumor resection and neck dissection, which proceeded uneventfully. Following the completion of the surgery, the patient was extubated safely and transferred to the PACU for monitoring. The procedure ended without complications, and the patient was stable postoperatively.
2.4. Case 4
A 35-year-old male was involved in a road traffic accident (RTA) and sustained multiple fractures, including a cervical spine fracture was posted for open reduction and internal fixation (ORIF) of the mandible fracture. Due to the nature of the injury, the patient had significant neck immobility, and his airway was considered potentially difficult due to restricted cervical motion and a history of mild dysphagia. The limited neck mobility from the cervical spine injury, combined with potential airway swelling and trauma, significantly increased the difficulty of performing intubation. The airway assessment revealed the possibility of both difficult visualization and potential airway obstruction due to the trauma, making intubation using a standard laryngoscope more challenging. Given these concerns, the C-MAC D-Blade VLS was selected for intubation.
After stabilizing the cervical spine appropriate induction agent and muscle relaxation were administered and the D-Blade was gently introduced. Despite the restricted cervical motion, the blade's angled design allowed for improved visualization of the glottis. The video feedback from the C-MAC system provided real-time assistance in guiding the placement of the ETT via nasotracheal route which was successfully completed on the first attempt. There were no complications such as trauma to the airway structures.
Following the successful intubation, the patient underwent ORIF of the mandible fracture. After the surgery was completed without further complications, the patient was extubated smoothly and transferred to the PACU for recovery and monitoring.
2.5. Case 5
A 60-year-old female with a large thyroid mass (9×5cm) was scheduled for a total thyroidectomy. The mass had caused significant tracheal deviation, and the patient also reported a history of dysarthria and dysphagia. Given the size of the mass, the airway was potentially compromised, with concerns about tracheal compression and risk of airway obstruction during intubation. The airway evaluation raised concerns about difficulty using standard laryngoscopy, as the mass could interfere with conventional blade angulation and compromise glottic visualization. To manage the anticipated difficult airway, the D-Blade of the C-MAC VLS was selected.
After administering appropriate induction agent and ensuring the patient's airway was adequately prepared, the D-Blade was introduced into the mouth. Despite the tracheal deviation and limited space due to the mass, the D-Blade’s angulation allowed for excellent visualization of the airway structures. The video feed from the C-MAC system provided real-time guidance, allowing the operator to precisely place the ETT. The intubation was successfully completed on the first attempt, with no complications such as airway trauma or difficulty in securing the airway.
Following the successful intubation, the patient underwent total thyroidectomy without further issues. The surgery proceeded uneventfully, and after the procedure, the patient was extubated smoothly and transferred to the PACU for recovery. The patient remained stable throughout the postoperative period and was monitored closely for any signs of airway compromise.
In all these cases intra venous midazolam 0.2 mg/kg and glycopyrrolate 0.2 mg as premedication, Fentanyl 1.5 mcg/kg for analgesia, propofol 1.2 mg/kg was used as induction agent, short acting depolarising muscle relaxant succinyl choline 1 mg/kg was given for muscle relaxation and the patient was maintained on isoflurane and intermittent dosages of Atracurium throughout the intraoperative period and before extubation Neostigmine and glycopyrrolate were given for reversal.
3. DISCUSSION
Prediction of difficult intubation can be possible using physical characteristics such as obesity, restricted mandibular protrusion, higher Mallampati classification, short thyromental distance, and immobility of the neck. However, anatomical abnormalities involving the larynx and trachea are frequently asymptomatic and can remain unsuspected until difficult tracheal intubation during anesthesia.7 However, several patients of apparently normal appearance unexpectedly present great difficulties at intubation. A study of anatomical factors in these patients should improve ability to predict and manage a potential failed intubation. When an experienced operator fails in two attempts at direct laryngoscope-assisted intubation, the case can be viewed as a difficult intubation case. If mask ventilation is possible, other airway management devices may be considered. Recently, clinical application of video laryngoscopy has been very helpful in resolving difficult intubation cases.8
The D-Blade of the C-MAC VLS has proven to be an invaluable tool in managing difficult airways, offering significant advantages over traditional intubation techniques. In this case series, we demonstrated its efficacy across five challenging clinical scenarios, where conventional laryngoscopy might have failed due to anatomical abnormalities, reduced mouth opening, limited neck mobility, and airway obstruction.
The D blade is specifically designed for the difficult airway. It can be used in both anesthetized and awake patients. With its flat profile and elliptically shaped blade, it can be glided along the tongue to guide the user directly to the epiglottis. Particularly when it comes to difficult intubation Cormack Lehane III and IV, the D blade enables successful intubation.3 One of the primary benefits of the D-Blade is its optimized angulation, providing an improved view of the glottis by offering an angle of 60-80 degrees, even in patients with anatomical challenges. This direct line of sight reduces the need for excessive manipulation and minimizes risks such as trauma, aspiration, and hypoxia. In all five cases, the D-Blade facilitated successful intubation, allowing for clear visualization of the vocal cords, even in patients with severe restrictions in neck movement or mouth opening.
The real-time video feedback provided by the C-MAC system is another crucial advantage. It allows for continuous visual assessment during intubation, helping the operator make adjustments for precise placement, which is particularly important in high-risk scenarios. The ability to see the airway structures on a video screen also promotes better team coordination and assists in training new clinicians.
While a VLS generally improves intubation success rates, their optimal use requires familiarity with the device and the ability to interpret the video feed accurately. Proper training is essential for maximizing the benefits of this technology, as inexperienced operators may struggle with the device’s unique angulation or video output. The advantage of using the VLS in relation to the Macintosh metal blade is that there is no need to align the pharyngeal and laryngeal axes during the laryngoscopy maneuver. Therefore, the VLS is a great option in scenarios in which there are factors suggesting the presence of difficult airway.4 However, several patients of apparently normal appearance unexpectedly present great difficulties at intubation. A study of anatomical factors in these patients should improve ability to predict and manage a potential failed intubation.9
The use of VLSs like the C-MAC system has been shown to enhance patient safety in difficult airway management. Studies indicate that video laryngoscopy improves first-attempt success rates, reduces complications, and offers greater precision compared to direct laryngoscopy, particularly in patients with challenging anatomies or in emergency situations.
Patients that could be intubated directly without difficulty or using only external laryngeal manipulation are more with D‑Blade. Use of accessory maneuvers such as tube rotation, partial inflation of cuff, and use of forceps were less with D‑Blade than Macintosh laryngoscope.4
It was easy to insert the C-MAC, to obtain a view of the glottis, and to intubate the trachea, without major complications. Because the shape of the blade is similar to the original Macintosh blade, using a tube stylet is not required.6 The use of the C-MAC VL in the setting of an anticipated difficult airway with Mallampati grade 3 and 4 should lead to a higher rate of successful intubation when compared with McCoy laryngoscopy.11 D-Blade VLS causes less dental compression compared to Macintosh and especially the conventional C-MAC VLS.12 C-MAC D-Blade videolaryngoscope had significant benefits for intubation time and difficulty compared to the McCoy laryngoscopy during nasotracheal intubation. It provided for better glottic visualization and it took less time to advance the nasotracheal tube from the oropharynx to the glottic inlet with this device.13 C-MAC VLS-aided intubations using D-blade significantly reduced the incidence and severity of post-operative sore throat, hoarseness of voice, and cough following orotracheal intubation as compared to use of traditional Macintosh laryngoscope.13 There was no significant difference in terms of sympathetic stimulation between Macintosh and C-MAC D-Blade videolaryngoscope.4
Despite its advantages, some limitations remain, such as its higher cost and potential reduced effectiveness in patients with extreme anatomical challenges. Additionally, the widespread adoption of VLSs may be limited in resource-constrained settings. In contrast to many previous VLS’s, the C-MAC has the unique advantage of obtaining both a direct laryngoscopic view and a camera view that are displayed on the video screen. On one hand, this may be very helpful for educational purposes, because the instructor may follow the student’s intubation attempts directly on the video screen.6
Further research is needed to evaluate the comparative effectiveness of the D-Blade against other VLSs and direct laryngoscopy, especially in emergency settings. Large-scale studies could also assess its impact on long-term patient outcomes, including airway trauma and post-intubation complications.
4. CONCLUSION
The D-Blade of the C-MAC video laryngoscope is a highly effective tool for managing difficult airways, providing superior glottic visualization and improving intubation success in complex scenarios. While operator proficiency is essential, its integration into routine airway management is likely to improve safety and outcomes, particularly in high-risk cases. Further studies are necessary to fully understand its broader applications and effectiveness.
5. Ethical considerations
Ethical approval was obtained from the institutional ethical committee. Written consent was obtained from every patient to use and publish the data for the academic interest.
6. Conflict of interest
All authors declare that there was no conflict of interest.
7. Funding
The study utilized the hospital resources only, and no external or industry funding was involved.
8. Authors’ contribution
UG: Concepts, Design, Literature search, Data acquisition, Manuscript preparation
PR: Concepts, Design, Literature search, Data analysis, Editing
SRS: Concepts, Design,
9. REFERENCES
- Garg M, Shakya R, Mary Lyngdoh N, Pradhan D. Comparison between McCoy laryngoscope and C-MAC video laryngoscope in anticipated difficult airway: a prospective randomised study. Cureus. 2022;14(7):e26685. PubMed DOI: 7759/cureus.26685
- Jeong HW, Song EJ, Jang EA, Kim J. Managing a difficult airway due to supraglottic masses: successful videolaryngoscopic intubation after induction of general anesthesia. Perioper Med. 2024;13:21. PubMed DOI: 1186/s13741-024-00377-9
- Dubey M, Goel N, Choudhary I, Gupta L. C-MAC D-blade laryngoscope: a saviour for difficult intubation in lateral position. Indian J Clin Anaesth. 2017;4(4):536–8. Full Text
- Hazarika H, Saxena A, Meshram P, Kumar Bhargava A. A randomized controlled trial comparing C Mac D Blade and Macintosh laryngoscope for nasotracheal intubation in patients undergoing surgeries for head and neck cancer. Saudi J Anaesth. 2018;12(1):35–41. PubMed DOI: 4103/sja.SJA_239_17
- Gupta A, Gupta N, Kamal G, Girdhar KK. Videolaryngoscopy bails us out of difficult intubation scenarios in syndromic children: a case series. Turk J Anaesthesiol Reanim. 2021;49(1):78–82. PubMed DOI: 5152/TJAR.2020.00947
- Cavus E, Kieckhaefer J, Doerges V, Moeller T, Thee C, Wagner K. The C-MAC videolaryngoscope: first experiences with a new device for videolaryngoscopy-guided intubation. Anesth Analg. 2010;110(2):473–7. PubMed DOI: 1213/ANE.0b013e3181c5bce5
- Ki S, Cho SB, Park S, Lee J. Management of unanticipated difficult airway in a patient with well-visualized vocal cords using video laryngoscopy: a case report. Anesth Pain Med. 2023;18(2):204–9. PubMed DOI: 17085/apm.23002
- Yun HJ, So E, Karm MH, Kim HJ, Seo KS. Orotracheal intubation in a patient with difficult airway by using fiberoptic nasotracheal intubation: a case report. J Dent Anesth Pain Med. 2018;18(2):125–8. PubMed DOI: 17245/jdapm.2018.18.2.125
- King TA, Adams AP. Failed tracheal intubation. Br J Anaesth. 1990;65(3):400–14. PubMed DOI: 1093/bja/65.3.400
- Cangiani LH, Vicensotti E, Ramos GC, Oliveira GJS. Use of video laryngoscope for tracheal intubation in patient with oral cavity mass: case report. Braz J Anesthesiol. 2020;70(4):434–9. PubMed DOI: 1016/j.bjan.2020.03.016
- Kılıçaslan A, Topal A, Erol A, Uzun ST. Comparison of the C-MAC D-Blade, conventional C-MAC, and Macintosh laryngoscopes in simulated easy and difficult airways. Turk J Anaesthesiol Reanim. 2014;42(4):182–9. PubMed DOI: 5152/TJAR.2014.59672
- Seo KH, Kim KM, John H, et al. Comparison of C-MAC D-blade videolaryngoscope and McCoy laryngoscope efficacy for nasotracheal intubation in simulated cervical spinal injury: a prospective randomized comparative study. BMC Anesthesiol. 2020;20:114. PubMed DOI: 1186/s12871-020-01021-x
- Tosh P, Kadapamannil D, Rajan S, Narayani N, Kumar L. Effect of C-MAC video laryngoscope-aided intubations using D-blade on incidence and severity of postoperative sore throat. Anesth Essays Res. 2018;12(1):140–4. PubMed DOI: 4103/aer.AER_182_17