Dario Galante, MD1, Marco Caruselli, MD2, Francesco Dones, MD3, Salvatore Meola, MD1, Gianluca Russo, MD4, Giuseppe Pellico, MD5, Antonio Caso, MD6, Massimo Lambo, MD1, Flora Donadei, MD7, Giuseppe Mincolelli, MD7
1University Department of Anesthesia and Intensive Care University Hospital “Ospedali Riuniti”, Foggia (Italy)
2Department of Anesthesia and Intensive Care, G. Salesi Children’s Hospital, Ancona (Italy)
3Department of Anesthesia and Intensive Care, University of Palermo (Italy)
4Department of Anesthesia and Intensive Care, Hospital of Lodi (Italy)
5Department of Anesthesia and Intensive Care, G. Tatarella Hospital, Cerignola Foggia (Italy)
6Department of Anesthesia and Intensive Care, Teresa Masselli-Mascia Hospital, San Severo Foggia (Italy)
7Department of Anesthesia and Intensive Care, M. Bufalini Hospital, Cesena (Italy)
Correspondence: Dario Galante, Responsible for Pediatric and Neonatal Anesthesia, University Department of Anesthesia and Intensive Care, University Hospital “Ospedali Riuniti”, Foggia (Italy); Tel: +390881732387; +390881732357; Fax: +39088173287; E-mail: dario.galante@tin.it
ABSTRACT
The transversus abdominis plane (TAP) block is a relatively simple technique that provides myocutaneous anesthesia that, as part of a multimodal analgesic treatment, may be useful in the prevention and treatment of parietal postoperative pain. Initial experience with ultrasound TAP block demonstrated efficacy of the echoguided technique in different surgical procedures such as cesarean section, appendicectomy, laparoscopic cholecystectomy, infra umbilical surgery in adult and pediatric patients. Recently published clinical trials suggest that TAP block may represents an effective alternative to epidural anesthesia but further studies in larger population are necessary.
Keywords: Ultrasound guidance; Regional anesthesia; Pediatric anesthesia; Transversus abdominis plane block
Citation: Galante D, Caruselli M, Dones F, et al. Ultrasound transversus abdominis plane (TAP) block in pediatric patients: Not only a regional anesthesia technique for adults. Anaesth Pain & Intensive Care 2012; 16(2): 201-204
Successful regional anesthesia relies on the accurate location of the target nerve and the placement of local anesthetic solution around the nerve. Historically, nerve identification has relied on surface anatomical landmarks to locate the injection site and then either pops, clicks or paresthesiae to identify the position of the needle close to the nerve.
For the last 25 years, peripheral nerve stimulation (PNS) has replaced paresthesiae, using a small electric current passed through the needle to stimulate the nerve. All these techniques are essentially blind and use an indirect method to locate and identify the nerve, but more importantly to predict success. Anesthetic solution blocks the nerve, but its spread cannot be accurately predicted using ‘the old’ or ‘conventional’ methods; as such, until now all local anesthetic techniques carry an inherent failure rate of 5%-20%, depending on the skill of the operator. Multiple trial-and-error attempts to locate the target nerve can lead to operator frustration, unwarranted patient pain and time delay in the operating room, especially in patients with difficult anatomical landmarks.
Medical ultrasound has been used for more than 40 years but its use in anesthesia has only developed recently. Since 2000 and on the back of NICE Technology Appraisal Guidance No.49, which stressed the use of ultrasound in central venous access, the ultrasound machines have become commonplace within our hospital and a growing body of evidence is developing to support the use of ultrasound in regional anesthesia.
Recently, the ultrasound transversus abdominis plane (TAP) block has gained popularity for intraoperative and postoperative pain management1,2 in a variety of abdominal surgical procedures in adult, pediatric and neonatal patients.
The abdominal wall consists of three muscle layers: the external oblique, the internal oblique and the transversus abdominis and their associated fascial sheaths. This muscular wall contains the T7-12 intercostal nerves, the ilioinguinal and iliohypogastric nerves and the lateral cutaneous branches of the dorsal rami of L1-3. The above nerves run in a neurovascular plane between the internal oblique and transversus abdominis muscles and represent the ‘target’ of local anesthetics. Anyway it has been demonstrated that anatomical variants exist and this aspect is highly individual. For these reasons the traditional landmark-guided technique involving needle insertion at the triangle of Petit was often accompanied by a high rate of failure.3,4 The goal of TAP block about the excellent level of analgesia produced is due to the progressive spread of the local anesthetic over several hours.
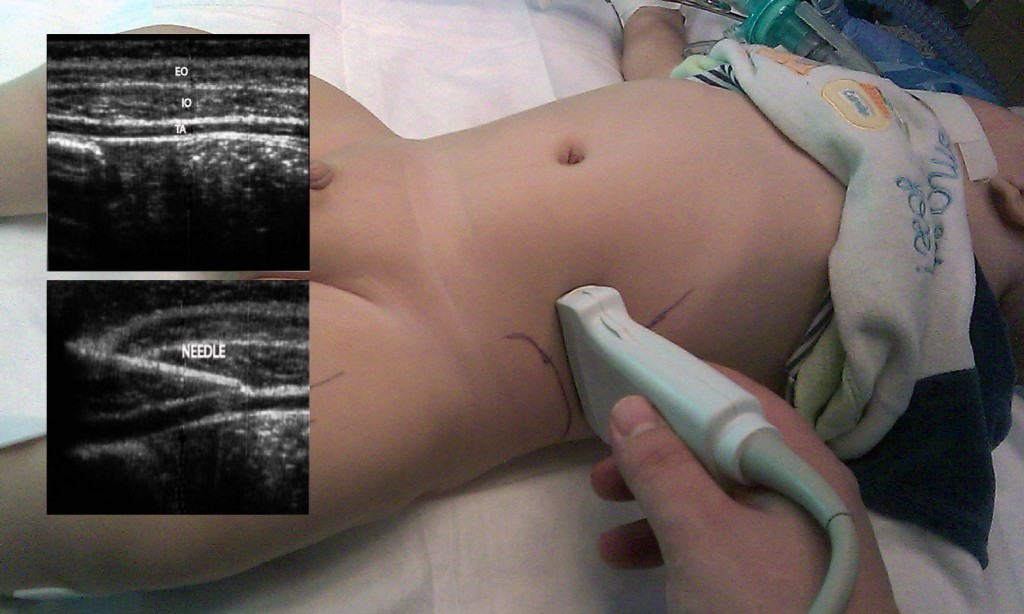
Fig 1: The position of the probe. The insets show three muscle layers: the external oblique (EO), the internal oblique (IO) and the transversus abdominis (TA); the needle well visualized under ultrasound guidance
For what concern the technique a linear, 5 to 15 MHz ultrasound probe, is placed in a transverse plane to the lateral abdominal wall in the mid axillary line between the lower costal margin and iliac crest. The tip of the needle needs to be positioned between the internal oblique and the transversus abdominis muscle in the fascial layer that separates the two muscle layers (Fig 1). A predetermined volume of local anesthetic (0.2-0.3 ml/kg in pediatric patients; up to 20 ml in adults or older children) is injected on either side as single shot or continuous infusion through a catheter under ultrasound guidance.
Various subcostal approaches have been described for ultrasound TAP block. The oblique subcostal TAP block produces a reliable analgesia of the suvraumbilical abdomen.5. In this case the linear probe needs to be positioned parallel to the costal margin and oblique respect to the sagittal plane. The needle is inserted close to the xiphoid process and its tip directed between transversus abdominis and the rectus abdominis muscles where the local anesthetic needs to be injected. Anyway, some studies demonstrated that the traditional ultrasound TAP block approach produced a good analgesia from the L2 to the T7 dermatome and above the umbilicus because the local anesthetic spreads easily between muscles planes so it is not always necessary to move the needle in different directions increasing the risk of vascular or parenchymal injuries.6,7 The neuraxial blocks are usually preferred for intraoperative and postoperative analgesia in pediatric patients (for example caudal/epidural block) but they are not always possible.
Bleeding tendencies (coagulopathy), spinal dysraphism (meningomyelocele), post-laminectomy, post-spinal fusion with instrumentation, infants with potential bony anatomical abnormalities (VATER) contra-indicate the performce of neuraxial blocks so an alternative is necessary.
In pediatric patients indications for TAP block are laparotomy, appendectomy, Nissen fundoplication, pyloromyotomy, major abdominal wall surgery, colostomy placement and closures.8 In fact, in many surgical procedures a good level of analgesia can be obtained. An interesting study has been recently published about the effectiveness of TAP block in 64 pediatric patients aged 5-12 years receiving bone graft from the ilium to the alveolar cleft. In these patients analgesia was effective with a significant reduction of postoperative analgesic rescue drugs.9
On the contrary, another research paper demonstrated that, following pediatric inguinal surgery, ilioinguinal block was effective than ultrasound TAP block in which supplemental postoperative and intraoperative analgesics were necessary.10
A significant reduction in intraoperative and postoperative opioids requirements after TAP block has been demonstrated also for renal transplant recipients. This aspect is very important due to the altered pharmacokinetics of many drugs in these patients.11 Nevertheless, the above conclusions seems to be contradicted by a recent research performed in twenty-eight adult patients undergoing elective open gynecological surgery that received bilateral ultrasound TAP block (3 mg/kg of ropivacaine). In each patient the mean peak total venous ropivacaine concentration resulted in potentially neurotoxic (2.2 mcg/ml) level. We have no data about pediatric patients, so it is likely that peak venous concentration may be different as well in the elderly or critically ill.12 It is well known that the use of ultrasound helps in reducing volume and concentration of local anesthetic but during the TAP block the absorption surface area between the muscle layers is wide, whatever technique is used.
Another important issue that should not be underestimated is represented by the risk of femoral nerve palsy due to the position of this nerve that lies in the same tissue plane as the space deep to transversus abdominis. The local anesthetic placed between transversus abdominis and transversalis fascia (that is continuous posteriorly with the iliacus fascia) can spread up to femoral nerve and surround it. It is not clear if the use of ultrasound may really avoid this complication but helps to reduce the amount of local anesthetic administered and consequently the rate of this complication.
Ultrasound TAP block is also accompanied by a good pain relief and reduced intraoperative and postoperative opioids requirements after laparoscopic surgery. In this case a bilateral TAP block is necessary because the abdominal skin incisions for the ports of laparoscopic procedure are performed on both sides.13
The echoguided techniques allow avoiding or reducing a great number of complications described for traditional procedures using landmarks. This affirmation seems to be controversial and much debated. A case of ultrasound-guided TAP block causing liver trauma and bleeding in a patient undergoing an inguinal hernia repair has been described, perhaps for using an inappropriate ultrasound machine.14 This complication was more frequent with the old blind technique, where it was necessary to locate the inferior lumbar Petit triangle. On the contrary, the use of ultrasound has significantly reduced this risk, so we can affirm that similar complications must be attributed to poor training or procedural errors rather than the technique itself. An in-plane approach is the best choice when performing the ultrasound guided TAP block because it allows a correct visualization of the needle tip, the three muscle layers and peritoneum. The needle tip has always to be identified and followed during the whole procedure. If appropriately performed under ultrasound guidance with skilled hands TAP block is safe but it’s necessary to receive training in sonoanatomy. An inappropriate ultrasound machine is another important risk factor but we cannot consider it the main cause of liver damage. In fact, liver sonoanatomy can be well visualized also with older ultrasound equipment. With the use of appropriate needles, even with low ultrasound resolution, the transversus abdominis plane and the liver are well visualized without difficulties.
Catheter can be placed, also bilaterally, in the said plane for continuous infusion of local anesthetics even if a multimodal analgesia and intravenous opioid are often required in addition to the TAP block because visceral pain is not blocked. Continuous infusion by this technique requires both a detailed knowledge of sonographic anatomy and technical skill. Multimodal analgesia combined with TAP block sometimes do not provide additional benefit as demonstrated after major gynecological cancer surgery with no significant difference in postoperative morphine consumption.15
Echoguided TAP block seems to be useful in reducing morphine requirements and opioid-related side-effects in the intensive care unit in patients following major abdominal surgery. This aspect represents a great advantage versus epidural anesthesia due to a reduction of hemodynamic changes and pain influences on assisted ventilation.16 The use of regional pain control techniques in intensive care unit is a much-debated issue because neuraxial blocks are often associated with complications when other comorbidities are present. Clotting disorders and hemodynamic instability make the blocks unreliable and safe; and the intravenous administration of high dosages of opioids and other drugs for pain management may represent a further risk in this class of patients.
The use of ultrasound helps to reduce volume and concentrations of local anesthetics with the ability to ‘target’ exactly the neural structures.17 Echoguided TAP block help us to administer the local anesthetic at any level between the internal oblique and the transversus abdominis muscles. In this way a kind of ‘natural elastomeric pump’ is produced with a gradual slow-release of drugs over several hours without the hemodynamic side effects of neuraxial blocks.
To study this last topic further, a comparative study between ultrasound TAP block and ultrasound caudal block in pediatric patients undergoing infraumbilical surgery for postoperative analgesia is under way in our institution. From an analysis of the first data, the analgesia of the abdominal wall evaluated by Children and Infants Postoperative Pain Scale (CHIPPS)/h24 appears to be equivalent on early postoperative time points and on emergence with similar score. Mean postoperative CHIPPS score over the first 6 hours suggest a prolonged postoperative analgesia when compared with caudal block. Mean duration of action was 9.6 hours (range 7-15.5 hours) and mean depth of the TAP was 1.1 cm (range 0.8-1.6) in children of ages 1-36 months.
CONCLUSION
Further research, including prospective pharmacokinetic and pharmacodynamic studies, is necessary to determine the safety, efficacy and the exact dosages with different local anesthetics for provision of analgesia following anterior abdominal wall surgery. This issue is particularly important in pediatric patients for whom the published indexed literature is still poor and limited to a small number of patients. The use of advanced ultrasound techniques allowed obtaining great advantages during the last few years, not only for traditional regional blocks but also for patients with rare diseases for which safety is essential.
Financial support received: None
Conflict of interest: None
REFERENCES
- McDonnell JG, O’Donnel B, Curley G, et al. The analgesic efficacy of transversus abdominis plane block after abdominal surgery: A prospective randomized controlled trial. Anaesth Analg 2007; 104: 193-97.
- O’Donnell BD, McDonnell JG, McShane AJ. The transversus abdominis plane (TAP) block in open retropubic prostatectomy. Reg Anaesth Pain Med 2006; 31: 91.
- Rafi AN. Abdominal field block: a new approach via the lumbar triangle. Anesthesia 2001; 56: 1024.
- McDonnell JG, O’Donnell BD, Farrell T, et al. Transversus abdominis plane block: a cadaveric and radiological evaluation. Reg Anesth Pain Med 2007; 32: 399.
- Hebbard P. Subcostal transversus abdominis plane block under ultrasound guidance. Anesth Analg. 2008; 106: 674-5; author reply 675.
- McDonnell JG, O’Donnell B, Curley G, Heffernan A, Power C, Laffey JG. The analgesic efficacy of transversus abdominis plane block after abdominal surgery: a prospective randomized controlled trial. Anesth Analg 2007; 104: 193–7
- O’Donnell BD, McDonnell JG, McShane AJ. The transversus abdominis plane (TAP) block in open retropubic prostatectomy. Reg Anesth Pain Med 2006; 31: 91
- Suresh S, Chan VW. Ultrasound guided transversus abdominis plane block in infants, children and adolescents: a simple procedural guidance for their performance. Paediatr Anaesth. 2009; 19: 296-9.
- Tanaka M, Mori N, Murakami W, Tanaka N, Oku K, Hiramatsu R, Nakagawa M, Yasumoto K. The effect of transversus abdominis plane block for pediatric patients receiving bone graft to the alveolar cleft. Masui. 2010; 59: 1185-9.
- Fredrickson MJ, Paine C, Hamill J.Improved analgesia with the ilioinguinal block compared to the transversus abdominis plane block after pediatric inguinal surgery: a prospective randomized trial. Paediatr Anaesth. 2010; 20: 1022-7.
- Mukhtar K, Khattak I. Transversus abdominis plane block for renal transplant recipients. Br J Anaesth. 2010; 104(5): 663-4.
- Griffiths JD, Barron FA, Grant S, Bjorksten AR, Hebbard P, Royse CF. Plasma ropivacaine concentrations after ultrasound-guided transversus abdominis plane block. Br J Anaesth. 2010; 105(6): 853-6.
- El-Dawlatly AA, Turkistani A, Kettner SC, Machata AM, Delvi MB, Thallaj A, Kapral S, Marhofer P. Ultrasound-guided transversus abdominis plane block: description of a new technique and comparison with conventional systemic analgesia during laparoscopic cholecystectomy. Br J. Anaesth. 2009; 102(6): 763-7. Epub 2009 Apr 17.
- Lancaster P, Chadwick M. Liver trauma secondary to ultrasound-guided transversus abdominis plane block. Br J Anaesth. 2010; 104: 509-10.
- Griffiths JD, Middle JV, Barron FA, Grant SJ, Popham PA, Royse CF. Transversus abdominis plane block does not provide additional benefit to multimodal analgesia in gynecological cancer surgery. Anesth Analg 2010; 111: 797-801.
- Niraj G, Kelkar A, Fox AJ. Application of the transversus abdominis plane block in the intensive care unit. Anaesth Intensive Care 2009; 37: 650-2.
- McNaught A, Shastri U, Carmichael N, Awad IT, Columb M, Cheung J, Holtby RM, McCartney CJ. Ultrasound reduces the minimum effective local anaesthetic volume compared with peripheral nerve stimulation for interscalene block. Br J Anaesth. 2011; 106(1): 124-30. Epub 2010 Nov 8.