Muhammad Ahsan-ul-Haq, MCPS, FCPS*, Mushtaq Hussain Raja, FCPS**
*Consultant Anesthesiologist, Prince Abdul Aziz Hospital, Arar (Saudi Arabia)
** Consultant Anesthesiologist, Combined Military Hospital, Peshawar (Pakistan)
Corresponding Author: Dr Muhammad Ahsan-ul-Haq, MBBS, FCPS (Anesthesiology), Consultant Anesthetist, Prince Abdul Aziz Hospital, Arar (Saudi Arabia); E-mail: ehsanulhaq702@yahoo.com
ABSTRACT
Background: The aim of this study was to highlight the excessive workload on the under staffed surgical teams, handling the combat mass casualties of ‘war on terrorism’. Triage, nature of injuries sustained, operative management, post operative care and the outcome in terms of morbidity and mortality are discussed.
Study period and place: This study was carried out at Combined Military Hospital (CMH) Peshawar Pakistan, from July 2008 to June 2009.
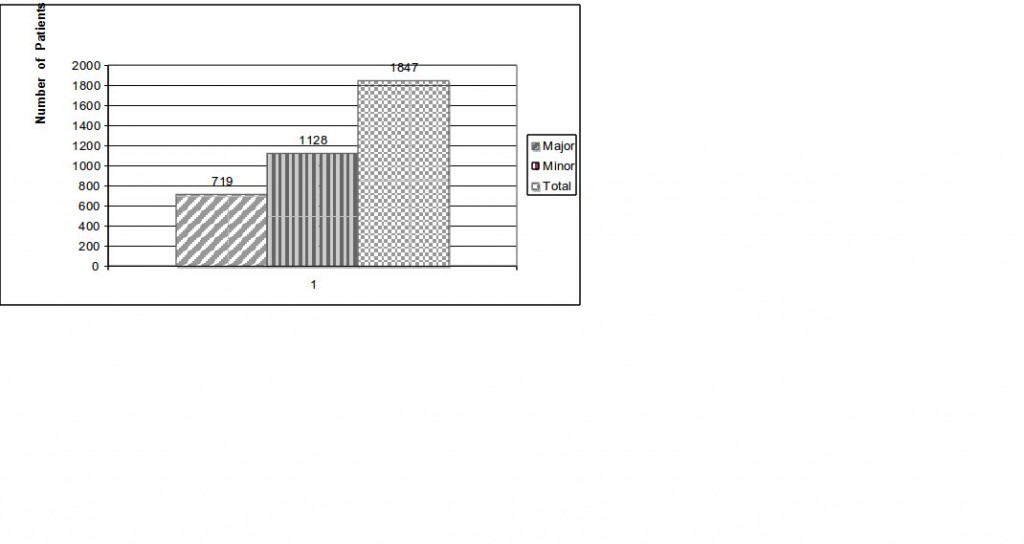
Methodology: A total of 1309 evacuated combat casualties were received at this hospital from the combat zone during this period and 1847 surgical procedures (1128 minor and 719 major) were performed. The major surgical procedures were performed for 80 abdominal, 204 orthopedic, 12 chest, 31neurological, 17 vascular and 375 multiple injuries (including burns, amputations, foreign bodies, deep lacerated wounds, ENT, eye and orodental injuries). Two surgical teams, each comprising of 2 anesthesiologists, 6 surgeons and 18 operating room assistants (ORA), worked alternatively, round the clock in 6 operating rooms. It was a race against the time as almost all the patients requiring major surgery, were in shock state. Resuscitation and surgical procedures had to start simultaneously. Only two trained nurses were looking after 11 critically ill patients in ICU and just one nurse was available for 20-30 patients in the general ward at any given time.
Results: Out of a total of 1309 patients, 1298 survived, 29 required ventilatory support. Out of 10 patients of penetrating head injury 6 developed brain death and were removed from the ventilator, 4 were successfully weaned off. Five patients died due to septicemia, DIC (disseminated intravascular coagulation) and multiple organ dysfunction syndrome (MODS).
Conclusion: Combat casualties comprise of a spectrum of trauma; head injury, hemorrhage and septicemia are the main killers. Apart from optimal use of resources available, it is the shear dedication and commitment to the service that drives the men to work continuously for long hours to manage mass combat casualties efficiently and yield good result.
Key words: War injuries; Combat casualties; Evacuation; Triage; Operative management; Ventilatory support; Under staffing.
INTRODUCTION
‘War on terrorism’ started initially in Afghanistan after 9/11, but later on involved Pakistan as well. It is being fought at about 1100 kilometers long mountainous border between Pakistan and Afghanistan. It is one of the most difficult terrains in the world. Rugged mountains, spiky peaks, crevices, thick forests, caves and deep burrows, are common physical features (2). The local people living across the border of both countries are
tribal people living almost nomadic life since ages. Manufacturing and selling small weapons, poppy cultivation and drug trafficking and smuggling of all type of goods were their main trades to make a living; but US invasion in Afghanistan lead them to train children for suicidal attacks and kidnapping people for ransom (3). These local people are born warriors and they have been fighting tribal wars since ages. British and other foreign intruders longed for taking over the control of this area, but miserably failed and left it as a bad job due to heavy casualties and declared it as no man’s land (3). Pakistan is one of the key partners of Allied Forces, committed to the ‘war on terrorism’. It has contributed and suffered a lot, not only at Afghan border but throughout the country where suicidal attacks are a common happening and taking the lives of innocent civilians including children and women (4). We present here our experience of managing combat casualties flown in to a tertiary care base hospital.
METHODOLOGY
Most of the casualties were received by helicopter evacuation. After disembarking, they were immediately rushed to the emergency suite, where triage was done.
Triage:
A team of two senior surgeons and a senior anesthesiologist was detailed to perform triage at emergency room. Following guidelines were used for categorizing and sorting the patients according to the severity of their injuries;
(1) Immediate: Patient whose condition demands immediate treatment to save life, limb, or eyesight. This category has the highest priority. Examples include, airway obstruction, massive external bleeding e.g., amputation, shock, burns of the face, neck, hands, feet, or perineum and genitalia. Salvage of life takes priority over salvage of limb.
(2) Delayed: Patients who have less risk of losing life or limb by treatment being delayed. Examples are, open chest wound (without respiratory distress), abdominal wounds (without shock),eye injury (severe, without hope of saving eyesight),other open wounds, fractures, second and third degree burns (not involving the face, hands, feet, genitalia, and perineum) covering 20 percent or more of total body surface area.
(3) Minimal: ‘Walking wounded’, minor lacerations, contusions, sprains and strains, minor combat stress problems, burns 1st or 2d degree under 20 percent of total body surface area and not involving critical areas such as hands, feet, face, genitalia, or perineum.
(4) Expectant: Patient so critically injured that only complicated and prolonged treatment offers any hope of improving life expectancy. Massive head injury with signs of impending death, third degree burns covering more than 85 percent of body surface area, prolonged unconsciousness, severe facial injuries and terminal cases (11).
Advanced management at base hospital:
Combined Military Hospital Peshawar is a 600 bedded, tertiary care hospital, which received all the casualties from FATA and Swat valley. All were brought to this hospital mostly by air ambulances. It served as a base hospital. Base hospital is a tertiary care teaching hospital where almost all the facilities of advanced treatment are available, including vascular, chest, neurosurgery and post operative ventilatory care in multidisciplinary ICU. On arrival, priority 1 patients were resuscitated on the operating table with I/V fluids and blood transfusion, ionotropic support was added as per requirement. Usually the patients were having multiple injuries and at times two surgical teams were performing surgery simultaneously on the same patient, e.g. one team doing the vascular repair on the limb and other team operating on head and neck, thorax or abdomen. All the patients were labeled as full stomach. Anesthetic technique usually employed was, inj. ketamine as induction agent and rapid sequence intubation with short acting muscle relaxants. Maintenance was done with isoflurane in a mixture of oxygen and nitrous oxide, together with good analgesia. Central line was placed and standard monitoring was done (12).
Major limb injuries were managed by external fixators and debridement of wounds.
A team of 6 surgeons, 2 anesthesiologists, 18 ORA and 2 trained ICU nurses had to deal 30 to 40 casualties at a stretch. This hospital has 6 Ors; the ORA to OR ratio is 3:1. There is an acute shortage of anesthesiologists (13), only 2 anesthetists looked after 6 patients undergoing major surgeries. Moreover, one of them had to run from OR to ICU to attend the calls in ICU or to ER to receive more casualties. Both the ER and ICU were being looked after by house officers, who were not well trained to deal such emergencies. There is a medical ICU and a surgical ICU with total bed strength of 21, but during emergency all the beds were being used for surgical patients. As compared to international standards, where 2 well trained nurses are supposed to look after one patient on ventilator (14), only 2 nurses were available to look after 11 critically ill patients in ICU, including 3 to 4 patients on ventilators. In general ward only one nursing assistant was looking after 20 to 30 patients.
RESULTS
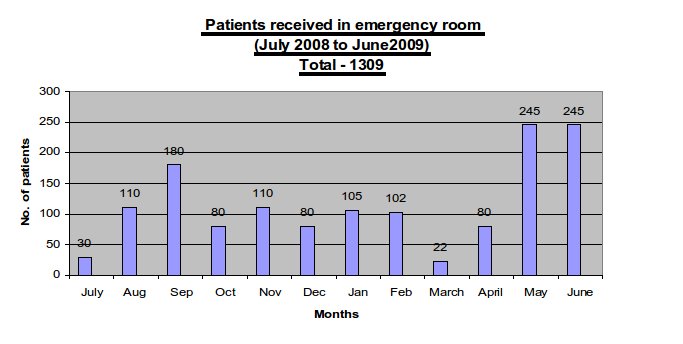
Figure 1 shows the number of combat casualties received per month during July 2008 to June 2009. Figure 2 shows number of minor and major operations done and Table-I shows surgical procedures performed. Most of the soldiers suffered from multiple injuries; including multiple fractures, chest and abdominal injuries with multiple intestinal perforations, diaphragmatic, splenic and liver injuries (6). Most of the soldiers who sustained a head injury, died on the spot due to severe hypoxemia and shock which are two considerable factors associated with poor prognosis in severe traumatic brain injury (7).
We received eighty patients, who sustained multiple abdominal injuries, 65 had intestinal perforations, 20 liver lacerations, 12 splenic rupture, 6 ureteric injuries and 6 stomach perforations. Twenty five operated cases required redo surgery; per operative finding in these showed 10 missed perforations and in the remaining 15 patients there was disruption of anastomosis. In 17 patients with vascular injuries (6 femoral, 2 axillary, 4 brachial and 5 poplitial artery injuries), 12 grafts and 5 simple repairs were performed. Out of these, two femoral grafts were rejected; redo surgery was done, but due to post operative infection and graft rejection, lower limb amputation was opted to save the life in both of the cases.
In 22 patients, amputation of the limbs was needed to save the life. Out of 12 chest injured patients, 8 penetrating chest injuries (PCI) were managed by tube thoracostomy. Four patients needed open thoracostomy for haemostatic control. Rate of chest infection was very high among the patients who needed chest intubation in ER.
Out of 31 head injury patients, 21 had penetrating injuries; debridement and haemostasis was done; ten patients needed ventilation and only 4 out of ten could make full recovery (12).
Ventilatory support:
Twenty nine patients were placed on ventilator post-operatively. Table 2 shows the indications for putting the patient on ventilator. Most of the patients were weaned off the ventilator in 48 hours. In difficult weaning cases, per cutaneous tracheostomy was performed, usually on third post op day in ICU, which eased the weaning process. Patients who needed prolong ventilation included those with chest injury resulting in pneumothorax, hemothorax or pyothorax, penetrating head injury and those who underwent extensive surgery. Ventilator induced pneumonia (VIP) was a common feature in patients who required prolong ventilation. Mild to moderate complications were treated successfully.
Eleven patients died during the course of postoperative ventilatory management. Six ‘penetrating head injury’ patients were declared as brain dead; while septicemia and DIC was the cause of death in 5 patients, who had been received in the ER in a severe state of shock. All of them underwent extensive surgery, required massive transfusions and developed post op complications. Two were reopened due to disruption of anastomoses and secondary bleeding from liver site, two developed ARDS (acute respiratory distress syndrome) after aspiration pneumonitis and one died due to multiple organ failure after rejection of femoral graft (12).
DISCUSSION
*The fate of the wounded lays with those who apply the first dressing (1) (Col. Nicholas Senn)
*90% of combat deaths occur on the battlefield before the casualty ever reaches a medical treatment facility (1) (Col. Ron Bellamy)
In this article, a first hand, practical experience as a member of an under staffed surgical team, managing the soldiers who suffered serious life threatening war injuries, is discussed. There is an ongoing war on terrorism being fought in the Federally Administered Tribal Areas (FATA), bordering with Afghanistan and Swat valley of Pakistan. Condition of the terrain and the difficulties faced to evacuate the seriously wounded soldiers and triage are discussed. By the time the wounded arrived at the base hospital, almost all the major cases, were found in severe shock. An attempt is made to discuss about the type of injuries received during the said period.
Major injuries were those where general anesthesia was required to deal the emergency cases and minor injuries were small wounds treated under local anesthesia or sedation +analgesia. Management involved resuscitation, operative procedures and post operative care. Many patients underwent multiple surgeries. Under staffing was a major problem faced. Dedication of doctors and paramedics working untiringly was appreciable.
Under staffing:
Under staffing is one of the major problems in our hospitals. We are deficient in man power in every department, whether it is ER, OR, ICU, or the general wards. Secondly, due to the prevalent security threats about one third of the staff has to be deputed on guard duties. Apart from guard duties, medical staff was frequently sent to the battlefields, either to meet the shortage of staff, to relieve the front line medical staff for a break or to replace the injured medical staff.
Chain of evacuation:
In traditional wars, Pakistan army has got an efficient chain of evacuation of casualties. Injured soldiers fighting in the front battle field are brought by the stretcher bearers to Regimental Aid Post (RAP) where first aid is given and then all patients are transferred to an Advanced Dressing Station (ADS) where proper treatment is given and patients are examined in detail. Serious patients are shifted to a Main Dressing Station (MDS) where life and limb saving surgeries are performed and patients requiring advanced treatment are shifted to base hospital, which is usually the nearest Combined Military Hospital, where tertiary and definitive care is provided (8). In FATA and Swat valley, due to difficult terrain, mountainous areas, thick forests and hostile local population, the above mentioned chain of evacuation proved totally ineffective. Injured were brought to the Forward Trauma Centers (FTC), established in the field. Evacuation of seriously injured combat soldiers was a tedious job because of continuous heavy firing; it was virtually impossible to carry the injured till the time the guns of the militants were made silent. Rescue staff had to face heavy firing and many a times rescuers themselves became victims (9). Transferring patients by road was risky too, as most of the roads were infested with mines (IED). Bushes, boulders and caves provided good shelters to the militants who could ambush any vehicle including an ambulance. From the field, injured could only be evacuated by air ambulance to the base hospital. Pakistan Army Aviation is equipped with transport helicopters e.g. Puma and MI 17, which were used as air ambulances. Even transferring patients by air ambulance service was not totally out of danger, as many a time, air ambulances were also fired upon. In acute emergency situations, air ambulances had to fly under cover of Cobra gunship helicopters. Most of those ambulances could lift 12 lying and 20 sitting patients at a time (10). At times more than 40 casualties were received in Emergency Room (ER) of the base hospital.
Nature of injuries:
The common modes of attack by the militants are by ambush, mining the field with IEDs (Improvised Explosive Devices), suicidal attacks on the military posts or moving convoys and ramming suicide vehicles filled with explosives. Bullets, pellets and splinters of hand grenades, dirty nails, were the common weapons used by the militants. (5) A wide variety of injuries were seen.
CONCLUSION
Combat casualties comprise of a spectrum of trauma; head injury, hemorrhage and septicemia are the main killers. The outcome of the mass combat casualties not only depends on early evacuation, simultaneous resuscitation-management and optimal use of available medical facilities, but also on the dedication and good team work that helps reduction in morbidity and mortality. However, management of ventilated patients can be improved if sufficient well trained nursing staff is available.
ACKNOWLEDGEMENTS
We are highly obliged to our surgical teams and Army aviation staff who worked selflessly to evacuate and manage the combat casualties. We are thankful to the administration of Combined Military Hospital Peshawar, for administrative support and medical resources.
REFERENCES
1: Tactical Combat Casualty Care (TCCC), North American Rescue Product. 2008, (Online) http://www.narescue.com/TacticalCombatCasualtyCare.aspx
2: Pakistan History, North West Frontier Province of Pakistan (NWFP). (Online) http://www.pakistan4ever.com/nwfp/nwfp.asp
3: Terrorism Havens, Pakistan council on foreign relations. Updated 2005, copy right 2009 (Online) http://www.cfr.org/publication/9514/
4: Amy Z. Terrorism Timeline, Pakistan and the Global War on Terror. Updated 2009
(Online) http://terrorism.about.com/od/globalwaronterror/tp/Pakistan—Terror-War-Timeline.htm
5: Abbas A. Inter Services Public Relation (ISPR) report, 11th April 2009 (Online) http://news.google.com.pk
6: Operation record register, CMH Peshawar Pakistan, July 2008 to June 2009: 34-63
7: Knuth T, Letarte PB, Ling G, Moores LE, Rhee P, Tauber D, Trask A. Guidelines for the field management of combat-related head trauma. Assessment: oxygenation and blood pressure. New York (NY): Brain Trauma Foundation 2005: 11-13
8: Manual of AMC (Army Medical Corps) training part III, 1990:23-25
9: Abbas A. Inter Services Public Relation (ISPR) report, 10th June 2009 (Online) http://news.google.com.pk
10: Mi-8 / Mi-17 Hip Multi-Mission Helicopter, Russia. (Online) http://www.army-technology.com/projects/mi8t/
11: Triage, Conventional battlefield casualties, Copyright 2009. (Online) http://www.medtrng.com/blackboard/perform_casualty_triage.htm
12: Patient record register medical ICU, CMH Peshawar Pakistan July 2008 to June 2009:4-42
13: Table of organization and equipment, Ministry of Defense Pakistan 1982; 3: 34-38
14: TE Oh. Design and organization of intensive care. Oh, s intensive care manual, 5th edition 2003; 1:7-9