Saeed Ahmed Solangi, MCPS, (FCPS-II)*, Safia Maqsood Siddiqui, FCPS**, Muhammad Saleh Khaskheli, MCPS, FCPS, MSc (Pain Medicine)***, Maqsood Ahmed Siddiqui, MCPS, FCPS-II, MSc (Pain Medicine)*
*Consultant Anaesthetist, ***Assistant Professor
Department of Anaesthesia,SICU& Pain Management, People’s Medical College Hospital, Shaheed Benazir Abad (Nawabshah)
**Assistant Professor
Department of Gynecology and Obstetrics, People’s University of Medical & Health Sciences for Women, Shaheed Benazir Abad (Nawabshah)
Correspondence: Dr. SafiaMaqsoodSiddiqui, Assistant Professor, Flat # M- 6 Doctors Flats, inside People’s University of Medical & Health Sciences for Women Shaheed Benazir Abad (Nawabshah); Cell No: 03337006748,03003212517; Email: drmaqsood70@yahoo.com
ABSTRACT
Objective: To compare the effects of general and spinal anesthesia in patients undergoing elective Cesarean section in terms of neonatal outcome.
Study design: Randomized control trial.
Setting: This study was conducted in the department of anesthesiology, surgical intensive care and pain management and department of Gynecology and Obstetrics, Peoples Medical College Hospital Nawabshah.
Duration of study: June 2009 to December 2009.
Subjects and methods: Patients in this study were admitted through obstetric OPD for lower segment Cesarean section. Patients were selected by simple random envelop draw method. Sample size were 160 patients, they divided in to two equal groups. Group A (N=80) patients underwent spinal anesthesia and Group B patients underwent general anesthesia. Immediately after delivery of the neonate, umbilical artery blood sample was taken for assessment of blood pH. Apgar score was assessed at 01 and 05 minutes and recorded on proforma. Anesthesia was labeled as effective i-e satisfactory if the Apgar score was 7 and above and blood pH 7.2 and above.
Results: An Apgar score >7 was observed at 01 and 05 minutes in 78(97.5%) and 80 (100%) neonates respectively in group A while it was 60(75%) and 74 (92.5%) in group B neonates. Apgar score>7 was observed in significantly more neonates in group A as compare to group B (p =0.028). Average Apgar score at 01 and 05 minutes was also significantly higher in group A than group B; 8.04±0.82 vs 7.10±0.92 (p=0.0001) and 9.89±0.32 vs 9.34±1.07 respectively (p=0.0001).Umbilical artery blood pH>7.2 was observed significantly high in group A93.8% as compared to group B 83.8% (p=0.045). Also average pH was significantly high in group A than group B e.g. 7.38±0.15 vs 7.21±0.16 (p=0.017).
Conclusion: Spinal anesthesia is associated with better neonatal out come as compared to general anesthesia in elective Cesarean sections.
Key words: Cesarean section; Spinal anesthesia; Bupivacaine; General anesthesia.
CITATION: Solangi SA, Siddiqui SM, Khaskheli MS, Siddiqui MA. Comparison of the effects of general vs spinal anesthesia on neonatal outcome. Anaesth Pain & Intensive Care 2012;16(1):18-23.
INTRODUCTION
Cesarean section can be performed under general or regional anesthesia like spinal or epidural technique. The Obstetric anesthetist requires special training and skills to provide safe anesthesia. The anesthetic techniques and agents chosen should provide good anesthesia and analgesia with minimal effects on feto-maternal well being1.
The spinal anesthesia is commonly considered as more practical and safer than other techniques like general and epidural because it is simple to administer, need of minimal monitoring, the dose of drugs required to induce spinal anesthesia is 1.5 milliliter, therefore unlikely to produce systemic effects in the baby so less neonatal exposure to depressant drugs, a decreased risk of maternal pulmonary aspiration and an awake mother at the birth of baby. As with any regional technique the disadvantages are risks of an extensive block, fixed duration of anesthesia, hypotension2 (9%) and the risk of postdural puncture headache1,3.
The drugs required for general anesthesia are multiple, most of the drugs effect the baby in two ways: by direct effect from placental drug transfer and by indirect effect resulting from maternal physiological and biochemical changes, which appear to be much more important. They may produce systemic effects in the baby like low Apgar score and sedation. In this technique there are risks of difficult intubations, maternal pulmonary aspiration, delayed recovery, nausea and vomiting. The incidence of maternal mortality may reach up to 10%2,4.
In 1952 Dr: Apgar an obstetric anesthesiologist proposed the Apgar score as a means of rapid evaluation of the physical condition of infants shortly after the birth. The scores are taken at 01 and 05 minutes after delivery. Of the two scores, the 05 minutes score is regarded as the better predictor of survival in infancy in the long term. Whereas the 01 minute score definitely has the value for; assessing the effects of different drugs given to the mother during the Cesarean section. This method is even more appealing because it is non invasive5.
The most useful umbilical cord blood parameter is arterial pH which is more representative of the fetal metabolic condition. Umbilical cord gas and pH values for the umbilical artery can be affected by alterations in the cord blood flow with the delivery process6. Apgar score and umbilical artery pH provides best measures of neonatal outcome after Cesarean section under general and spinal anesthesia. Apgar score study conducted at Abbasi Shaheed Hospital, Karachi, indicates that Apgar score of neonates at 1 and 5 minutes whose mother received spinal anesthesia was 8.1±0.7and9.8±0.41 while it was 9.52±0.71 and6.9±0.73 in general anesthesia7.
Though the previous studies have observed that fetus born under general anesthesia had higher incidence of acidemia and lower Apgar scores, whereas during spinal anesthesia there occurs decrease in pH, resulting in acidemia of neonate but these studies didn’t shown results on pH and as overall outcome including the Apgar score, remains unproved4,8.
So this study was conducted to obtain our own observation regarding pH and Apgar score because spinal anesthesia is commonly used technique in our setup. The local data available in this regard is limited and this study was conducted to assess the safer mode of anesthesia for elective Cesarean section in terms of neonatal outcome, so that the same may be followed in such patients.
METHODOLOGY
This randomized control trial was conducted from June 2009 to December 2009 in the department of anesthesiology, surgical intensive care and pain management and department of Gynecology and Obstetrics, Peoples Medical College Hospital Nawabshah. A total of 160 patients were selected for study meeting the inclusion criteria. Assume that Apgar score at 5 minutes in Group A(spinal anesthesia) P1=80% while in Group B(General anesthesia) P2=62.2%. With 80% power of the test and 5% level of confidence, 80 patients were included in each Group. The patients were divided in to two groups by envelop draw method. Group A was given spinal anesthesia and Group B underwent general anesthesia.
Sampling technique was purposive sampling. All pregnant women with gestational age 37-40 weeks, ASA-1, with singleton pregnancy selected for elective Cesarean section were included. Fetal factors considered were normal growth parameters on ultrasound and adequacy of liquor.
Mother having PIH, history of spine or brain deformity, morbidly obese patient having BMI > 40, skin to uterine incision time > 10 minutes and uterine incision to delivery time > 3 minute were excluded from the study. Fetal factors for exclusion were congenital malformations, babies small for dates, and fetal distress.
After the approval of study from ethical committee of Peoples Medical College Hospital Nawabshah, informed written consent was taken from all selected patients on the basis of inclusion and exclusion criteria. The source of patients was department of gynecology/obstetrics. The risk and benefits of spinal and general anesthesia were explained to all of the patients in the study groups. As the patients were randomly divided by envelop draw method so all kind of bias and most confounds were ruled out.
After application of standard monitors i.e. non–invasive blood pressure, ECG and pulse oximetry and maintaining the intravenous lines, general anesthesia was given by a standardized anesthesia technique by performing rapid sequence induction and intubation with inj. propofol 2mg/kg, inj. suxamethonium 1.5 mg/kg, application of Sellick’s maneuver, confirmation of endotracheal tube, inj. atracurium 0.5mg/kg and then maintainance on 0.25%-0.5% isoflurane in oxygen/nitrous oxide. After the delivery of baby inj. nalbuphine 0.2mg/kg was given. At the end of surgery when patient resumed some breathing effort, residual effects were reversed with inj. neostigmine 0.35mg/kg and inj. glycopyrrolate 0.05mg/kg. When the patient became fully awake, the endotracheal tube was removed in lateral position.
Patients prepared for spinal anesthesia were preloaded with crystalloid solution. Bupivacaine 0.75%, 1.5 ml was given at L3-4 or L4-5 interspaces in sitting or lateral position and all patients were placed in supine position. Supplemental oxygen 4 liter/min was administered via Hudson mask.
Immediately after delivery of the neonate, umbilical artery blood sample was taken for assessment of blood pH and Apgar score was assessed at 01 and 05 minutes and recorded. Anesthesia was labeled as effective i.e. satisfactory if the Apgar score was ≥7 and blood pH was ≥7.2.
All statistical analysis was done using SPSS version 10. Frequency and percentages were computed for categorical variables like age groups, Apgar score, satisfactory and unsatisfactory outcomes. Mean with standard deviation, 95% confidence interval and median were also computed for quantitative variable like age, Apgar score and pH. Independent sample ‘t’ test was used to compare mean differences between groups for age, Apgar score and pH. According to cutoff value of Apgar score and pH, satisfactory and unsatisfactory condition was compared between groups by chi-square test and fisher exact test. P<0.05 was considered level of significance.
RESULTS
Most of the pregnant women were 21 to 35 years of age 148(92.5%) in both groups.The average age of the patients was 27.61±4.36 years (95%CI: 26.93 to 28.29). Average and 95% confidence interval of overall Apgar score at one and five minutes and pH of both groups are presented in Table 1.
The mean age of the patients received spinal anesthesia was 27.49±4.32 years and those received general anesthesia was 27.74 ± 4.42 years. Significant difference was not observed in age between the groups (p=0.72).Mean Apgar score of neonates at 01 and 05 minutes was significantly high in those women who received spinal anesthesia 7.21±0.16 and 9.89±0.32 as compared to those who received general anesthesia7.10±0.92 and 9.34±1.07 (p<0.01). Average pH was also significantly high in spinal group 7.38±0.15 as compared to general anesthesia group7.21±0.16 (p=0.017) (Table 2).
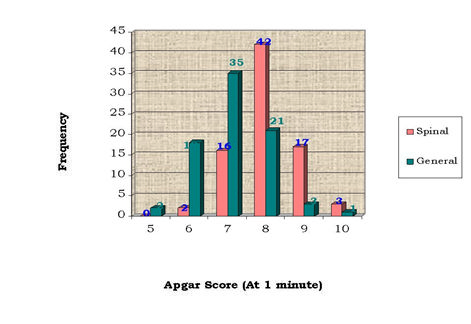
Satisfactory Apgar score at one minute in group B was observed in 60(75%) neonates while it was observed in 78(97.5%) neonates in group A. Unsatisfactory Apgar score was observed in 20(25%) neonates ingroup B as compared to 2(2.5%) of the neonates in group A (graph 01). Comparison of satisfactory Apgar score at five minutes between groups is presented in Table 3 and Graph 2. In group A, satisfactory (Apgar ≥ 7) was observed in all i.e. 80(100%) neonates while in group B it was observed in 74(92.5%) neonates. Satisfactory Apgar score was significantly high in group A than group B (p =0.028).
Umbilical artery blood pH≥7.2 was observed significantly low in group B as compared to group A; 83.8% vs. 93.8% respectively (p=0.045) as shown in Table 3.
Table 1: Overall descriptive statistics of study variables (n=160)
| Study Variables | Mean ± SD | 95%CI | Median
(IQR) |
Range |
| Age (Years) | 27.61 ± 4.36 | 26.93 to 28.29 | 28 (5) | 40 – 19 |
| Apgar at 01 min | 7.57 ± 0.99 | 7.41 to 7.72 | 8(1) | 10 – 5 |
| Apgar at 05 min | 9.61 ± 0.83 | 9.48 to 9.74 | 10(1) | 10 – 6 |
| pH | 7.24 ± 0.16 | 7.21 to 7.26 | 7.24(0.08) | 7.8 – 6.12 |
Table 2: Mean comparison of characteristics of patients between groups
| Variables | Group A
(Spinal (Anesthesia) |
Group B
(General (Anesthesia) |
P-Values |
| Age (Years) | 27.49 ± 4.32 | 27.74 ± 4.42 | 0.72 |
| Apgar at 01 min | 8.04 ± 0.82 | 7.10 ± 0.92 | 0.0001 |
| Apgar at 05 min | 9.89 ± 0.32 | 9.34 ± 1.07 | 0.0001 |
| Ph | 7.38 ± 0.15 | 7.21 ± 0.16 | 0.017 |
Graph 1: Frequency of Apgar score at 01 minute according to groups
Graph 2: Frequency of Apgar score at 05 minutes according to groups
Table 3: Comparison of satisfactory condition with respect to Apgar score at five minutes and ph
| Outcomes
|
Group A
(Spinal Anesthesia) n=80 |
Group B
(General Anesthesia) n=80 |
Total
n=160 |
p-Value |
| Apgar≥7 | 80(100%) | 74(92.5%) | 154(96.3%) | 0.028 |
| Apgar<7 | 0(0%) | 6(7.5%) | 06(3.8%) | |
| pH ≥ 7.2 | 75(93.7%) | 67(83.7%) | 142(88.7%) | 0.045 |
| pH< 7.2 | 5(6.3%) | 13(16.3%) | 18(11.3%) |
DISCUSSION
Internationally an obstetric anesthesia guideline recommends spinal and epidural over general anesthesia for most Cesarean sections9,10. This subject has been studied by many investigators over the years. Some have shown no difference in Apgar scores between the groups while others reported lower Apgar scores and worse outcomes with the use of general anesthesia11.
Apgar score of neonate at 01 and 05 minutes was significantly high in those women who received spinal anesthesia (8.04±0.82and 9.89 ±032) in the present study as compared to those who received general anesthesia(7.10±092 and 9.34±1.37), nearly consistent with the study on Apgar score conducted at Abbasi Shaheed hospital Karachi7; 8.1±0.7 and 9.8±0.41 in spinal anesthesia as compared to 6.9±0.73 and 9.52±0.71 in general anesthesia group. Kolatat et al12,Ong BY11and Alfredo M et al13 also found lower Apgar scores of the neonates whose mothers received general anesthesia. Dyer et al14 found worse outcome after spinal versus general anesthesia concerning pH but the better Apgar score in spinal group. Other investigators found no differences between different anesthetic regimens15,16.
Comparison of satisfactory Apgar score at one minute was also observed high in spinal group 78(97.5%) as compared to general anesthesia group 60(75%) neonates. Unsatisfactory Apgar score was observed in 20(25%) neonates in general anesthesia group as compared to 2(2.5%) of the neonates who received spinal anesthesia. Tony et al18 found it 0.6% in spinal and 2% in general anesthesia group while SukheraSA1found it 36% in general anesthesia group. Alfredo M et al14found depressed newborns 1.1% in the spinal group and 25.9% in the general group. At 01 min, a higher score for each parameter was found in spinal group with respect to general anesthesia group.
Satisfactory condition of Apgar score at five minutes was significantly high in group A than group B. In group A, it was observed in all i.e. 80(100%) neonates while in group B it was observed in 74(92.5%) neonates and Apgar<7 were seen in 6(7.5%) neonates. Tony et al17 found <7 Apgar at 05 minutes 1.3% in general anesthesia group and 4.3% in spinal anesthesia group whileSukheraSA1found it 11% in general anesthesia group. Alfredo M et al13found all newborns vigorous at 05 minutes in both groups. In the terms of better Apgar score and earlier initiation of breast-feeding, spinal anesthesia may be preferred to general anesthesia in Cesarean section15.General anesthesia has a detrimental effect on the Apgar score but this is short lived4.
Some authors believe that umbilical artery pH monitoring is more accurate method of assessing the fetal well being18,19. In the present study, average pH was significant high in neonates of groupA 7.38±0.15 than group B 7.21±0.16.Koltat et al12 showed that the fetuses born under general anesthesia had higher incidence of acidemia pH 7.21-7.26 and lower Apgar scores where as spinal anesthesia was associated with acidotic pH 7.19-7.26 but vigorous newborns. Hodgson et al20and Arif Yegin et al21observed high neonatal pH in spinal group. According to Sendag F and colleagues22, the mean umbilical artery blood PaCO2 and HCO3 values did not show any significant difference between the groups. Modern general anesthesia may sedate the baby, although this effect is short lived, easily overcome and its effect on acid base balance is essentially benign12.Kvak ZN and colleagues8 demonstrated no difference in short-term neonatal outcomes including Apgar scores and cord gas parameters.
Also in our study, satisfactory pH was found high 75(93.7%) in spinal group as compared to general anesthesia group 67(83.7%) and unsatisfactory pH was low 05(6.3%) in spinal as compared to general anesthesia group 13(16.3%). Arif Yegin et al21also found unsatisfactory pH16.1% in general anesthesia group. Alfredo M et al13 found no differences in pH values. Morgan PJ and colleagues23 found it 4.7 and 1.1%, in spinal and general anesthesia respectively. According to Robert et al24, regional anesthesia was associated with fetal acidemia, and had features of an acute respiratory type of acidemia, approximately 18% of infants had umbilical artery blood pH values of 7.19 or less.
Data is varying regarding the effect of anesthetic options on neonatal Apgar scores and umbilical artery parameters and the significance of small differences in these numbers is unclear. Each situation must be evaluated individually.
CONCLUSION
In our study, we observed that Apgar score and umbilical artery blood pH of neonates whose mothers received general anesthesia were lower than neonates whose mothers received spinal anesthesia. Spinal anesthesia is as effective as general anesthesia; fetal outcome is favorable and can be preferred over general anesthesia. It can be further evaluated in future by large studies on emergency cesarean sections, having all grades of anesthesia risk factors.
REFERENCES
- Sukhera SA, Ahmed S. Neonatal outcome: a comparison between epidural and general anesthesia for cesarean sections. Professional Med J 2006;13:72-8.
- Waris S, Yousuf M, Ahmed RA, Shahid M. An experience of spinal anesthesia versus general anesthesia. Surg Pak 2002;7:25-7.
- Kamran S, Akercan F, Akarsu T, Firat V, Ozcan O, Karadadas N. Comparison of the maternal and neonatal effects of epidural block and of combined spinal-epidural block for Cesarean section. Eur J Obstet Gynecol ReprodBiol 2005;121:18-23.
- Reynolds F, Seed PT. Anesthesia for cesarean section and neonatal acid-base status a meta analysis. Anesthesia 2005;60:636-53.
- Skolnick AA. Apgar quartet plays perinatologist’s instruments. JAMA 1996;276:1939-40.
- Khoury AD, Moretti ML, Barton JR. Fetal blood sampling in patients undergoing elective cesarean section: a correlation with cord blood gas values obtained at delivery. Am J Obstet Gynecol 1994;171:679-84.
- Sultana A. Masood Z, Hasan S. Effect of type of anesthesia on neonatal outcome. Anl Abbasi Shaheed Hospital Karachi Med Dent Coll 2004;9:552-7.
- Kavak ZN, Basgul A, Cehyan N. Short term outcome of newborn infants: Spinal versus general anesthesia for elective cesarean section: a prospective randomized study. Eur J Obstet Gynecol Rep Biol 2001;100:50-4.
- American Society of Anesthesiologists Task Force on Obstetric Anesthesia. Practice guidelines for obstetric anesthesia: an updated report by the American Society of Anesthesiologists Task Force on Obstetric Anesthesia. Anesthesiology 2007;106:843-63.
- Cyna AM, Dodd J. Clinical update: obstetric anesthesia. Lancet 2007;370:640-42.
- Ong BY, Cohen MM, Palahniuk RJ. Anesthesia for cesarean section — effects on neonates. Anesth Analg. 1989;68:270-275.
- Koltat T, Somboonnanonda A, Lertakyamanee J, Chinachot T, Tritrakaran T, Muangkasem J. Effect of general and regional anesthesia on the neonate (a prospective randomized trial). J Med Assoc Thai 1999 Jan; 82(1):40-45.
- Alfared M, Antonio DV, Anammaria G, Valentina P, Lara MG, Marianna G et al. General versus spinal anesthesia for elective caesarean sections: effects on neonatal short-term outcome. A prospective randomize study. J of Mat-Fet and Neot Med. Posted online Jan 21, 2010.
- Dyer Ra, Els I, Farbas J, TorrGJ, SchoemanLK, James MF. Prospective, randomized trial comparing general with spinal anesthesia for cesarean delivery in preeclamptic patients with a non reassuring fetal heart trace. Anesthesiology 2003 Sep;99(3):561-
- Wallace DH, Leveno KJ, Cunningham FG, Giesecke AH, Shearer VE, Sidwai Je. Randomized comparison of general and regional anesthesia for cesarean section delivery in pregnancies complicated by severe preeclampsia. Obstet Gynecol 1995;86:193-9.
- Lertakyamanee J, Chinachoti T, Tritrakarn T, Muangkasem J, Somboonnanonda A, Kolatat T. Comparison of general and regional anesthesia for cesarean section: success rate, blood loss and satisfaction from randomized trial. J Med Assoc Thai 1999;82:672-9.
- Tooni G, Ferrari B, De Felice C, Ventura A. Fetal acid-base and neonatal status after general and neuraxial anesthesia for elective Cesarean section. Int J Gynecol Obstet 2007;97:143-6
- Casey BM, Mclntire DD, Leveno KJ. The continuing value of the Apgar score for the assessment of newborn infants. N Engl J Med 2001;344:467-71.
- Winkler CL, HaultJC, Tucker JM, Owen J, Brumfield CG. Neonatal complication at term as related to the degree of umbilical artery acidemia. Am J Obstet Gynecol 1991;164:637-41.
- Hodgson CA, Wauchob TD. A comparison of spinal and general anesthesia for elective cesarean section: effect on neonatal condition at birth. Int J Obstet Anesth 1994;3:25-30.
- Arif Y, Zeki E, Murat Y, Meliha E. The effects of epidural anesthesia and general anesthesia on newborns at cesarean section. Turk J Med Sci 2003;33:311-14.
- Sendag F, Terek C, Oztekin K, Sagol S, Asena U. Comparison of epidural and general anesthesia for elective caesarean delivery according to the effects of Apgar scores and acid-base status. Aust N Z J Obstet Gynecol 1999;39:464-7.
- Morgan PJ, Halpern S, Lam-McCulloch J. Comparison of maternal satisfaction between epidural and spinal anesthesia for elective Cesarean section. Can J Anesth 2000 Oct;47(10):956-61.
- Roberts SW, Leveno KJ, Sidawi JE, Lucas MJ, Kelly MA. Fetal acidemia associated with regional anesthesia for elective cesarean delivery. Obstet Gynecol 1995 Jan;85(1):79-83.