Shabnam Saleem, FCPS*. Waseem Ismat Ch, FCPS, Diplomat Iranian Board**, Khulda Naaman, MCPS***
*Senior Registrar, **Professor, ***Anaesthetist
Department of Anesthesiology, Intensive Care & Pain, Shaikh Zayed Hospital & Federal Postgraduate Medical Institute Lahore (Pakistan).
Address for correspondence:
Dr Shabnam Saleem, Department of Anesthesiology, Intensive Care & Pain, Shaikh Zayed Hospital & Federal Postgraduate Medical Institute, Lahore (Pakistan).Email:shabnamsaleem72@gmail.com
ABSTRACT
Objective: We conducted this study to prove the hypothesis that the use of propofol-ketamine combination as induction agent is associated with less hemodynamic effects as compared to propofol-thiopentone combination.
Place and duration of study: The study was conducted in the Department of Anesthesiology, Intensive Care & Pain, Shaikh Zayed Hospital & Federal Postgraduate Medical Institute, Lahore from January 2009 to August 2009.
Study design: An interventional comparative study
Methods: One hundred and fourteen patients were enrolled for the study and were randomly allotted into two equal groups A (57) and B (57). ASA I and ASA II patients between the age group of 20-50 years, undergoing elective surgery under general anesthesia were enrolled in the study. Patients with neurological disease, pregnancy, ASA III and above, suspected difficult airway, hypertensive patients, and those taking drugs effecting blood pressure and heart rate were excluded from the study. Group A was induced with propofol–thiopentone combination and group B was given propofol and ketamine combination. The hemodynamic parameters, e.g. heart rate, systolic, diastolic and mean arterial pressures were monitored starting from baseline up to 10 minutes.
Results: Both groups did not differ as regards to gender, ASA physical status and age distribution.
On comparison of systolic, diastolic and mean arterial pressures among two groups, there was significant increase in group A combination at 1 minute after intubation (p <0.05), while no significant change was observed at 4, 7 and 10 minutes after intubation (p >0.05). There was significant increase pulse rate in group A at 1, 7 and 10 minutes after intubation (p <0.05), while no significant change was depicted at 4 minutes after intubation (p >0.05).
Conclusion: Administration of ketamine with propofol was comparatively better in maintaining the haemodynamic stability after induction as compared to thiopentone.
Key Words: Propofol-thiopentone; Propofol–ketamine combination; Haemodynamics; Blood pressure; General anaesthesia; Induction.
INTRODUCTION
Propofol, a commonly used agent for induction and maintenance of general anesthesia,1 is ideal for short and ambulatory surgical procedures requiring general anesthesia, as onset and recovery is rapid with fewer unwanted side effects.2 However, when used as the sole induction agent, it may cause significant reduction in arterial blood pressure and cardiac output.3 It produces a decrease in systemic arterial pressure greater than with a comparable dose of thiopentone.4 The decrease in blood pressure is due to both a decreased systemic vascular resistance and a reduced myocardial contractility (MC).1Despite a decrease in arterial pressure, the heart rate (HR) remains unchanged due to depression of the baroceptor response.1
Thiopentone sodium is also one of the most commonly used intravenous induction agents throughout the world.5 It causes a decrease in MC as well as peripheral vasodilation.5 Heart rate may fall but there is often a reflex tachycardia5 probably due to a central vagolytic effect. Cardiac output is often maintained due to increase in HR and increased MC from compensatory baro-receptor reflexes.6 However, HR and arterial pressure after intubation following induction with thiopentone proved to be no different from those achieved with ketamine.7 It has been shown that a mixture of thiopentone and propofol produces less hypotension as compared to propofol alone.8
Ketamine is a potent analgesic which also releases catecholamines, with subsequent tachycardia and hypertension.7 Intravenous ketamine causes a rise in systemic and pulmonary arterial blood pressure, HR, cardiac output and myocardial oxygen requirement.9 Direct stimulation of the central nervous system leading to increased sympathetic nervous system outflow seems to be the most important mechanism for cardiovascular stimulation.9 Administration of ketamine before induction with propofol has been shown to produce more hemodynamic stability as compared to propofol alone.1,10 The aim of our study was to prove the hypothesis that the use of propofol-ketamine combination as induction agent is associated with less hemodynamic effects as compared to propofol-thiopentone combination.
METHODOLOGY
The study was conducted in the Department of Anesthesiology, Intensive Care & Pain, Shaikh Zayed Hospital & Federal Postgraduate Medical Institute, Lahore after obtaining institutional approval and informed consent from all patients. The sample size was 114, divided into two equal groups, A and B, of 57 patients each. ASA I and ASA II patients between the age group of 20-50 years from both sexes, undergoing elective surgery under general anaesthesia were enrolled in the study. Patients with neurological disease, pregnancy, ASA III and above, suspected difficult airway, hypertensive patients and those on drugs effecting blood pressure and HR were excluded from the study. The patients were selected on pre-operative visits. All the patients were evaluated clinically to rule out any of the exclusion criteria. It was convenient sampling method. The randomization was done among the enrolled patients for allocation to either Group A or B. Data were collected on semi-structure Proforma in which study parameters were entered before and during intervention. On the day of surgery patients were shifted to the pre-operative area and were given oral midazolam 7.5mg 30 minutes before shifting to the operating room. In the operating room, baseline blood pressure and HR were recorded. After pre-oxygenation for 3 minutes induction with propofol and thiopentone mixture 1:1 (thiopentone 1.25% and propofol 0.5mg %) was done in Group A. In Group B, ketamine 0.5mg/kg was given 1 minute prior to induction with propofol 2mg/kg. Immediately after induction, vecuronuim 0.15mg/kg was administered. Three minutes after administration of vecuronuim, tracheal intubation was performed. Anaesthesia was maintained using isoflorane 0.5% -1% with 60% nitrous oxide in oxygen. The systolic, diastolic and mean arterial pressures and HR were recorded prior to tracheal intubation, 1 minute after intubation and every 3 minutes, thereafter.
Statistical Analysis
The sample size was calculated by using a computer soft ware epi-info-6 at 95% confidence interval 80% power and with expected frequency of hypotension in unexposed patients 4 with assumed relative risk equal to 6. Data was entered in a computer software SPSS. Data was cleaned and analyzed as the frequency tables were generated for basic variables (age, gender and type of surgery) of the data. Comparisons of the means of the systolic, diastolic and mean arterial pressures and HR were calculated and compared. The cross analysis for the HR changes with two of the combination of the drugs were done. Student’s t-test was applied in comparison of means of systolic, diastolic, MAP and HR with two combinations of drugs. Two- tailed Fisher test was applied in comparison of ASA I and II and chi-square test for gender profile of the patients in two groups.
RESULTS
One hundred and fourteen patients were enrolled for the study. Out of these 57 (50%) patients were randomly given drug-combination A, consisting of propofol and thiopentone and 57 (50%) patients were given drug-combination B, consisting of propofol and ketamine.
Age distribution among two groups was similar as shown in (Table 1). Both groups did not differ with regard to gender and ASA physical status (Table 2 and 3). The haemodynamic parameters mean of the systolic, diastolic and mean arterial pressure and HR were compared before and after induction up to 10 minutes between group A and B. There was significant increase of the mean systolic and diastolic arterial pressure in propofol–thiopentone combination (group A) at 1 minute after intubation (p <0.05, Graph1)
The mean systolic blood pressure in group A and B at 1 minute after intubation were 134mmHg SD ±22 and 126mmHg SD±21.The mean diastolic blood pressure in group A and B were 84 SD ± 14 and 76 SD ± 15. There was no significant change in arterial pressure depicted before induction, after intubation, 4 minutes, 7 minutes and 10 minute after intubation among two groups A and B (p >0.05, Graph 1).
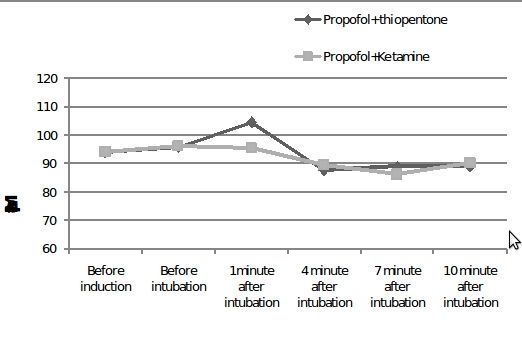
Mean HR was compared among two groups, A and B. There was significant increase in group A combination at 1 minute, 7 minute and 10 minute after intubation (p <0.05).The mean HR at 1min after intubation in group A and B were 100 SD ± 16 and 94 SD ± 13 , at 7min were 91 SD ± 15 and 84 SD ± 14 ,at 10min were 89 SD ± 17 and 81 SD ± 15. No significant change was depicted before induction, prior to induction, at 4 minutes after intubation (p >0.05, Graph 2 ).
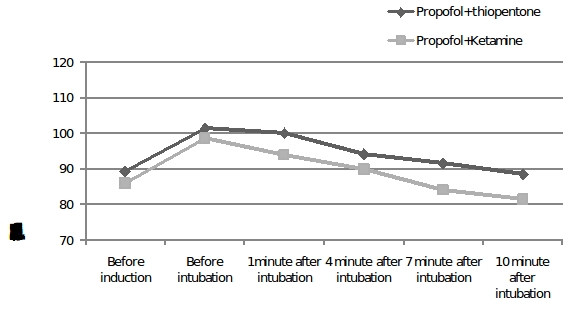
The mean arterial pressure (MAP) was compared between two groups A and B. There was statistically significant difference in MAP,1 minute after intubation in group A (p <0.05, Graph 3).The mean arterial pressure taken 1min after tracheal intubation in group A and group B were 104 SD± 17 and 95 SD ± 16 (p<0.05). There was no significant difference in MAP before induction, prior to intubation, 4 minutes, 7 minutes and 10 minutes after intubation.
DISCUSSION
The use of propofol for general anaesthesia is associated with decrease in arterial pressure which is due to reduction of MC, peripheral vascular resistance and sympathetic tone.10-12 Vagotonic effects of propofol reduce the HR that may cause severe bradycardia, complete atrio-ventricular block and cardiac arrest.10,13
Arterial pressure reduction by propofol is much greater than those seen after thiopentone administration.10 Advantage of propofol is that it is more effective in preventing the increase in arterial pressure after intubation than thiopentone .14
Sympathetic stimulation by ketamine increases MC and vascular resistance which in turn leads to increased arterial pressure and HR.15,16 Increases in plasma concentrations of epinephrine and norepinephrine occur as early as 2 minutes after intravenous administration of ketamine and return to control levels 15 minutes later.9
In our study, we compared haemodynamics of two combinations of drugs propofol–thiopentone (Group A) and propofol–ketamine (Group B). According to our results the later combination preserved greater hemodynamic stability than the former. Our results correlate with that of Furuya and colleague .10 Their results showed smaller increase in systolic, diastolic and mean arterial pressure just after intubation and 3 minutes after intubation when propofol-ketamine combination was given.10 Similarly, Srivastava and colleagues showed in their study that sympathomimetic actions of ketamine were effective in counteracting the hemodynamic depression of propofol which is also consistant with our study.17
Vora and colleagues have compared propofol with mixtures of propofol with either thiopentone or ketamine and found that propofol–ketamine is superior to propofol–thiopentone mixture because of its better hemodynamic stability.18 The results were consistant with our study. However, in their study a ketamine–propofol mixture was used consisting of 1% propofol 10ml and 0.5% ketamine 10ml, whereas in our study, we used ketamine 0.5mg/kg/min, one minute before induction by propofol 2mg/kg.
In our study, there was smaller increase in mean diastolic, mean systolic and mean arterial pressure 1 minute after intubation in Group B and there was no difference between two groups up to 10 minutes after intubation. HR remained relatively stable in Group B but there was significant increase in HR, 1, 7 and 10 minute after intubation in Group A. Furuya and colleagues reported that HR remained essentially unchanged after induction with propofol–ketamine combination, which is consistent with our study.10 The finding of relatively stable HR in group B is also supported by the findings of Ozkocak et al.19
The hemodynamic stability of the propofol–thiopentone admixture was also demonstrated by Yeo et al which is consistent with our study.8,20 Lesser doses of either agent is required for induction when a combination is used as afterload and MC is effected to a lesser extent. In present study, there was no significant difference in arterial pressure between the two groups prior to tracheal intubation, 4, 7 and 10 minutes after intubation. However, there was significant increase in arterial pressure 1 minute after intubation in Group A. It could be due to the fact that we recorded arterial pressure and HR after laryngoscopy and intubation, whereas previous studies monitored hemodynamics with propofol–thiopentone combination during laryngeal mask insertion.8 Wilson and colleagues showed that use of laryngeal mask airway was accompanied by smaller cardiovascular effects than those after laryngoscopy and intubation.21
One previous study showed that lack of analgesia with thiopentone provided no protection against catecholamine release commonly caused by noxious stimulus such as tracheal intubation.2 On the other hand, intense analgesia could be achieved with subanaesthetic doses of ketamine, e.g. 0.5mg/kg.22 Reduced concentration due to redistribution and antanalgesic effects of thiopentone are probable causes of increase in HR in Group A.
In summary, administration of both combinations preserved hemodynamic stability but propofol-ketamine combination (Group B) prevented any excessive increase in arterial pressure 1 minute after intubation and produced less effect on HR which allowed greater haemodynamic stability as compared to propofol-thiopentone combination. Hence, theoretically it is preferable for induction especially in hemodynamically unstable patients and possibly can be used in patients with ischemic heart disease.10
ACKNOWLEDGEMENTS
I am grateful to Allah Almighty, Who gave me the power, strength and determination to complete my study. I am extremely thankful and grateful to my honorable and respected teacher Prof. Waseem Ismat Chaudhry and to my parents for their continuous guidance and encouragement throughout my work.
I am also thankful to Dr. Muhammad Ashraf for data analyzing and Mr. Muhammad Yaseen Shad, whose technical skill enabled me to prepare this article.
REFERENCES
1. Bano F, Zafar S, Sabbar S, Aftab S, Haider S, Sultan ST. Intravenous ketamine alternates injection pain and arterial pressure changes during the induction of anaesthesia with propofol. A comparison with lidocaine. J Coll Physician Surg Pak 2007; 17: 390-3.
2. Turner RJ, Gatt SP, Kam PCA, Ramzan I, Daley M. Administration of a crystalloid fluid preload does not prevent the decrease in arterial blood pressure after induction of anaesthesia with propofol and fentanyl. Br J Anaesth 1998; 80: 737-41.
3. Djaini G, Ribes-Pasto MP. Propofol auto-co-induction as an alternative to midazolam co-induction for ambulatory surgery. Anaesthesia 1999; 54: 51-8.
4. Stoelting RK.Cardiovascular effects of propofol. In: Stoetling RK eds. Non-barbiturate induction drugs. New York: Lippincott-Raven, 1999; 143.
5. Aitkenhead AR. Thiopentone sodium as induction agent. In: Aithkerhead AR, Rowbohian DJ, Smith G eds.Intravenous anesthetic agents Edinburgh: Churchill Livingstone, 2001; 171-72.
6. Morgan GE. Cardiovascular effects of barbiturates. In: Morgan GE, Mikhail MS, Murray MJ eds. Non volatile anesthetic agents. Chicago: McGraw-Hill companies, 2006; 186.
7. Katz RL, Levy A, Slepian B, Sobel B, Lagasse RS. Haemodynamic stability and Ketamine-alfentanil anaesthetic induction. Br J Anaesth 1998; 81: 702-6.
8. Yeo KS, Kua SW, Teoh GS, Onsiong MK. The use of thiopentone/propofol admixture for laryngeal mask airway insertion. Anaesth Intens Care 2001; 29: 38-42.
9. Tweed WA, Minuck MS, Mymin D. Circulatory response to ketamine anesthesia. Anesthesiology 1972; 37: 613-619.
10. Furuya A, Matsukawa T, Ozaki M, Nishiyama T, kume M, Kumazawa T. Intravenous ketamine attenuates arterial pressure changes during the induction of anaesthesia with propofol. Eur J Anaesthesiol 2001; 18: 88-92.
11. Michelsen I, Hansen HSH, Kohler F, Lorenzen AG, RydLund E, Bentzon MW. Prophyloctic ephedrine attenuates the hemodynamic response to propofol in elderly female patients. Anaesth Analg 1998; 86: 477-81.
12. Robinson BJ, Ebert TJ, O’Brien TJ, Colinco MD, Muzi M. Mechanism whereby propofol mediates peripheral vasodilation in humans. Sympathoinhibiton or direct vascular relaxation. Anaesthesiology 1997; 86: 64-72.
13. Igarashi M, Nishikawa K, Nakayama M. Circulatory changes at the time of anaesthetic induction and endotracheal intubation. Comparison of thiamylal induction group and propofol induction group. Jap J Anaesthesiology 1998; 47: 1193-99.
14. Rouby JJ, Andreev A, Leger O. Peripheral vascular effects of thiopentone and propofol in humans with artificial hearts. Anaesthesiology 1991; 75: 32-42.
15. Hui TW, Short TG, Hong W, Suen T, Gin T, Plummer J.Additive interactions between propofol and ketamine when used for anaesthesia induction in female patients. Anaesthesiology 1995; 82: 641-48.
16. Schwabe K, Schenk HD. Optimized dosing strategies for TIVA with propofol and ketamine. Anaesthesist 1992; 41: 365-66.
17. Srivastava U, Sharma N, Kumar A, Saxena S. Small dose propofol or ketamine as an alternative to midazolam co-induction to propofol. Indian J Anaesth 2006; 50: 112-4.
18. Vora KS, Prabodhachandran MS, Bhosale GP, Singhal N, Pirikh GP, Shah VR. Comparison of admixtures of propofol – thiopentone, propofol – ketamine and propofol in ambulatory surgery. J Anaesth Clin Pharmacol 2005; 21: 413-8.
19. Ozkocak I, Altunkaya H, Ozer Y, Ayoglu H, Demirel CB, Cicek E. Comparison of ephedrine and ketamine in prevention of injection pain and hypotension due to propofol induction. Eur J Anaesthesiol 2005; 22: 44-8.
20. Jones O, Prankkenl R, Iang C. Propofol–thiopentone admixture-hypnotic dose pain on injection and effect on blood pressure. Anaesth Intensive Care 1999; 27: 346-56.
21. Wilson JG, Fell D, Robinson SL, Smith G. Cardiovascular responses to insertion of laryngeal mask airway. Anaesthesia 1992; 47: 300-2.
22. Stoelting RK. Clinical uses of ketamine. In: Stoelting RK eds.Non-barbiturate induction drugs. New York: Lippincott – Raven 1999;150-51.
Table 1: Age profile of the patients under study (n=114)
| Age groups ▼ | Drug Groups► | Total N=114 | |
| A Propofol + Thiopentone N=57 | B Propofol + Ketamine N=57 | ||
| Frequency (%) | Frequency (%) | Frequency (%) | |
| 1 to 20 Years | 4(7.01) | 6(10.52) | 10(8.77) |
| 21 to 40 Years | 38(66.67) | 41(71.92) | 79(69.29) |
| 41 to 60 Years | 15(26.31) | 10(17.4) | 25(21.92) |
Table 2: Gender profile of the patients under study (n=114)
| Gender
▼ |
Drug Groups► | Total
N=114 |
|
| A
Propofol + Thiopentone N=57 |
B
Propofol + Ketamine N=57 |
||
| Frequency (%) | Frequency (%) | Frequency (%) | |
| Male | 25(43.85) | 20(35.08) | 45(39.47) |
| Female | 32(56.14) | 37(64.91) | 69(60.52) |
| Statistical Analysis
Chi-square = 0.918 p value 0.338 (> 0.05) |
|||
Table 3: ASA profile of the patients under study (n=114)
| ASA Status
▼ |
Drug Groups► | Total
N=114 |
||
| A
Propofol + Thiopentone N=57 |
B
Propofol + Ketamine N=57 |
|||
| Frequency (%) | Frequency (%) | Frequency (%) | ||
| I | 52(91.23) | 56(98.25) | 108(94.74) | |
| II | 5(08.77) | 1(01.75) | 06(05.26) | |
| Statistical Analysis
Two tailed Fisher exact test value = 0.206 (> 0.05) ASA scoring was not significantly different among two groups of patients |
||||
Figure 1: Comparison of mean systolic and diastolic arterial pressure between two study groups
[The systolic and diastolic arterial pressure was significantly higher in propofol+ thiopentone combination at 1 minute after intubation with p = 0.044 and 0.003 respectively]
Figure 2: Comparison of mean heart rate between two study groups
[The heart rate was significantly higher in propofol+ thiopentone combination at 1, 7 and 10 minutes after intubation with p-values 0.034, 0.007 and 0.017 respectively]
Figure 3: Comparison of mean arterial pressure between two study groups
[Mean arterial pressure was significantly higher in propofol+thiopentone combination at 1minute after intubation (P<0.006)]