Ravi Bhat, MD*, Sameer K. Malhotra, MD**, Mandeep S. Dhillon, MS, MD***
* Assistant Professor of Anaesthesiology, JN Medical College, Belgaum (India)
**Professor of Anaesthesiology, Postgraduate Institute of Medical Education & Research, Chandigarh (India)
***Professor of Orthopaedics, Postgraduate Institute of Medical Education & Research, Chandigarh (India)
Correspondence: Ravi Bhat, MD; Department of Anaesthesia, JN Medical College, Belgaum , India); Phone: 09482181582; 0831–2473788, Extension: 1292; Fax: 0831-2472777; Email: kakkodravi@yahoo.co.in
ABSTRACT
Background and objective: Knee arthroscopy is the most common ambulatory orthopaedic procedure performed and there are few randomized studies comparing local anaesthesia and regional anaesthesia. The purpose of the study was to compare operating condition, recovery time, side effects of local anaesthesia combined with propofol infusion (LA/Propofol) with spinal anaesthesia (SA).
Methodology: Fifty ASA status I – II patients, between 18-50 years of age, scheduled for knee arthroscopy received either low dose bupivacaine spinal anaesthesia or intraarticular lignocaine combined with propofol infusion titrated to patient comfort randomly. An independent observer collected data.
Results: 24 patients (average age, 30 years) received LA/Propofol and 26 received SA. Baseline assessment of the two groups was similar. The mean time spent in the postoperative anaesthesia care unit (PACU) was 60.00 ± 14.89 minutes for the LAP group and 122.11 ± 19.55 minutes for the SA group (P = .0001). There were no statistically significant differences between the 2 groups with respect to nausea/vomiting (P =.5) or overall patient satisfaction (P = .3). The amount of time required to administer anaesthesia was similar between the two groups (14.23 ± 4.4 and 15.00 ± 5.89 min).The number of patients requiring airway support intraoperatively was higher in the LA/Propofol group compared with the SA group, 4 of 24 and 0 of 26, respectively (P =.02).
Conclusions: Although subjects receiving LA/Propofol were more likely to require some airway support intraoperatively compared with the SA group, LA/Propofol was associated with significantly less time to home readiness as measured by time in the PACU and comparable operating condition as well as patient satisfaction .
Key Words: Knee arthroscopy; Local anaesthesia; Propofol; Spinal anaesthesia
CITATION: Bhat R, Malhotra SK, Dhillon MS. A prospective, randomized comparison of low dose bupivacaine spinal anaesthesia versus local anaesthesia with propofol infusion for knee arthroscopy. Anaesth Pain & Intensive Care 2012;16(1):24-30
INTRODUCTION:
The shift in much of surgical practice from an inpatient to an outpatient paradigm has impelled us to adapt our anaesthetic techniques to the ambulatory setting1. Knee arthroscopy for outpatients can safely be performed under general anaesthesia, neuraxial anaesthesia, local portal infiltration/intraarticular injection or peripheral nerve blocks and each anaesthetic technique has its own advantages and disadvantages as shown by several studies2-4. The ideal anaesthetic for outpatient knee arthroscopy would be that which can be performed easily, has a fast onset and provides good operating conditions with a rapid recovery and minimal side effects. Spinal anaesthesia may provide many of these advantages, but the optimum drug and dose for this technique remains undetermined. A few reports in recent years have demonstrated both the feasibility and the benefits of spinal anaesthesia using small-dose bupivacaine in combination with an opioid5. Of the various anaesthetic techniques local anaesthesia (LA) appears to provide early recovery and shortest time to discharge. However, LA alone may not provide a comfortable patient experience or optimal operating conditions. The addition of propofol infusion with LA may provide excellent anaesthesia while still allowing for rapid recovery and patient discharge.
The purpose of this prospective, randomized study was to determine the operating room efficiency and recovery profiles as well as the reliability, complications, side effects and patient satisfaction levels of the minidose bupivacaine spinal anaesthesia technique compared with a technique of LA in combination with a titrated propofol infusion.
METHODOLOGY:
After approval from institutional ethical committee and written informed consent from the patients, this prospective randomized study was conducted in 50 ASA status I – II patients, between 18-50 years of age, scheduled for knee arthroscopy as a day care procedure. Patients with contraindications to either technique (e.g., allergy, coagulopathy, localized infection, or neurologic disease) were excluded. The two study groups were as follows: SAB – spinal anaesthesia with 0.5% bupivacaine 7.5 mg and LA/Propofol – local anaesthesia using 30 mL of 1% lidocaine with titrated IV propofol infusion. Visual Analogue Scale was explained to the patient at the time of pre-anaesthetic evaluation. Patients were kept fasting for 8 hours before taking up for surgery. After shifting to operating room, an intravenous access was obtained and infusion of isotonic sodium chloride 0.9% was started. Non-invasive monitoring like electrocardiogram, blood pressure and SpO2 were attached and baseline readings were taken. For all patients’ i.v. midazolam 0.02-0.03 mg/kg and fentanyl 0.75 – 1 mg/kg was given. All patients received oxygen through ventimask.
Group I (Spinal): Under aseptic condition, these patients were given spinal anaesthesia with 7.5 mg 0.5% hyperbaric bupivacaine through 26G Quinke’s spinal needle in L3-4 interspace.
Group II(LA + propofol): An infusion of propofol was started at the rate of 25-50mg/kg/min on arrival to operating room and titrated to maintain a stable level of sedation in which the patient remains responsive to verbal or light tactile stimulation. Boluses of propofol were given as needed (200-400 mg/kg). Before application of tourniquet and surgical preparation, 30ml of 1% lignocaine with epinephrine (1:2, 00000) was injected intraarticularly by the surgeon. Before incision additional 10ml of local anaesthetic was injected along the portal sites. If patient experienced pain at the time of skin incision additional fentanyl 0.5 mg/kg was given. In case still patient was anxious, further sedation was given with midazolam 0.01 mg/kg and fentanyl 0.5 mg/kg. If the patient comfort and/or airway could not be maintained (SpO2< 90%), it was considered as anaesthetic failure and general anaeshesia using propofol 2mg/kg , Oxygen and nitrous oxide through a laryngeal mask airway or an endotracheal tube was administered.
Heart rate, SpO2, NIBP, VAS score for pain were recorded every 5 minutes during intraoperative period. Time taken for anaesthetic procedure, Duration of surgical procedure, Patient comfort and operating condition as assessed by surgeon as A = Satisfactory, B = Neutral C = Unsatisfactory were also noted. In the Post Anaesthesia Care Unit all the patients were monitored until discharge criteria were met. Heart rate, blood pressure, respiration, level of consciousness, ability to stand and VAS score were recorded on arrival to the PACU and every 15 minutes until discharge. Severity of pain was assessed by 10 point linear Visual Analogue Scale and the rating of which was as follows: ‘0’ as no pain and ‘10’ as maximum imaginable pain. Postoperatively rescue analgesia was given with parecoxib 40 mg i.v. if the visual analogue score was more than 4 or patient asked for it. Number of rescue analgesic doses and time to first rescue analgesic requirement was noted. Vomiting was evaluated by number of episodes of vomiting. Ondansetron 0.15 mg/kg was given if nausea/vomiting were present and patients requiring antiemetic were noted.
Vital parameters and home readiness was evaluated every 15 minutes in the post anaesthesia cars unit until discharge. Patients were considered fit for discharge if:
a) Vital signs within 20% of pre-operative value
b) Consciousness –fully awake and oriented
c) Able to stand up for > 1 minute
d) Minimal nausea/vomiting
e) Minimal to moderate pain
f) Tolerating oral fluids
g) Minimal surgical bleeding
Time interval from arrival into Recovery Room until first oral intake, home readiness, and actual discharge was noted. Patient satisfaction was rated on a verbal scale of 5 = very satisfied, 4= satisfied, 3 = neutral, 2 = dissatisfied, 1 = very dissatisfied and was recorded at the time of discharge.
Statistical analysis was performed using SPSS 10.0 software for Windows (SPSS software GmbH, Munich, Germany). Data are presented as mean (with 2SD or 95% confidence interval [CI95]. The sample size of the study (Group I – 26, Group II – 24) was not normally distributed. Difference with respect to demographic data (age, weight, sex, preparation time and surgery duration) and Hemodynamic variables were analyzed using Mann-Whitney U test. Distribution of arthroscopic procedure was assessed using Fischer’s exact test. VAS score and level of satisfaction, airway support/GA between the groups were assessed by Chi-square test. Requirement of rescue analgesics and incidence of nausea/vomiting were compared using Fischer’s exact test. Time of first oral intake, time of ambulation, discharge time and duration of total hospital stay were assessed by paired t- test. A value of P < 0.05 was considered significant.
RESULTS:
The demographic data, duration of surgery, anaesthesia preparation time in Group I and Group II were comparable (Table-1)
All the patients in Group I had successful subarachnoid block, and none of the patients required general anaesthesia or airway support. One patient (4%) in Group II required general anaesthesia as relaxation was not adequate because of anxiety and inadequate pain relief. LMA was inserted and anaesthesia was maintained with propofol. Airway support in the form of jaw lifting was required in 3 patients and face mask was used in one patient. Jaw lifting was used only for short time (3 -8 min) when patient was deeply sedated and was obstructing the airway. None of these patients had oxygen saturation less than 92% and the airway support was somewhat precautionary measure. These episodes of partial airway obstruction were mostly after boluses of propofol when patient was uncomfortable due to value test applied to examine the knee joint (Table 2).
Hemodynamic parameters (HR, SBP, DBP, and SpO2) were comparable in both the groups during intraoperative and postoperative period. Intraoperative and postoperative values of these parameters did not show any significant change compared to baseline preoperative values in both the groups
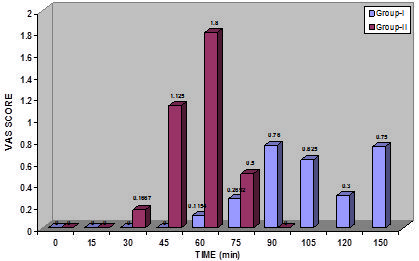
Pain at skin incision was present in 11 patients (45.8%) in Group II (P < 0.001) and was absent in all the patients in group-I. Those patients who had pain at skin incision responded to intravenous fentanyl supplementation and subsequently had median VAS score of 0(0-0) throughout rest of the intraoperative period (P>0.05). Postoperative VAS pain scores were comparable between both the groups at all the times except, at 45 and 60 minutes VAS scores were significantly higher in Group II (P < 0.001) A total of in 3 patients (11%) group-I and 6 patients (25%) in group II required rescue analgesia and the difference was not significant (P < 0.193) The number of episodes of nausea and vomiting and the rescue antiemetic used were not significantly different between the groups (P = 0.66)
Overall level of satisfaction with the anaesthetic technique was comparable between the groups (P > 0.05). Twenty (76.9%) patients in Group I and 16 patients in Group II (66.7%) were satisfied with anaesthetic technique. One patient in each group was not able to express the opinion and 4 patients in each group were neutral. None of the patient in both the groups was dissatisfied with the anaesthetic technique used. Anaesthetic technique was satisfactory in both the groups. There was no difficulty in examining the joint in any group.
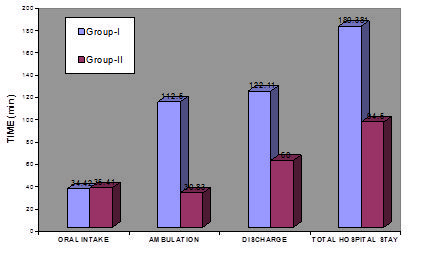
Time to ambulation, discharge, and total hospital stay was significantly higher in Group I as compared to Group II. Mean time to ambulation was 112.50 ± 25.70 and 30.83 ± 9.16 minutes in Group I and Group II, respectively (P < 0.001). Mean time to oral intake was 46.92±13.78 and 35.41 ± 8.19 minutes in Group I and Group II, respectively (P > 0.05). Mean time to discharge from hospital was 122.15 ± 19.55 in Group I and 60.00 ± 14.89 minutes in Group II (P<0.001). Total hospital stay was 180.38 ± 33.51 in Group I and 94.5 ± 29.20 minutes in Group II (P<0.001).
In Group II, 66% patients were discharged in less than 60 minutes and in Group I none of the patients achieved discharge criteria at 60 minutes.
DISCUSSION
The need to adapt to ambulatory surgeries has led to significant changes in anaesthetic techniques and choice of technique. In day care anaesthetic procedures several issues are considered such as patient safety, procedure time, early ambulation, postoperative analgesia and cost effectiveness.
While spinal anaesthesia is attractive for reasons of speed, simplicity and reliability, traditional methods of spinal anaesthesia have proven problematic for ambulatory surgery8. For decades lignocaine has been the local anaesthetic of choice for spinal anaesthesia in the ambulatory surgical patient. This choice is based on the drug’s short duration of action, which allows for a timely recovery and discharge. Many reports of transient neurological symptoms9,10 with lignocaine have led researchers to undertake the adaptation of the longer-acting local anaesthetic bupivacaine in the ambulatory setting. In ambulatory surgery, bupivacaine may delay the recovery of motor function, cause urinary retention, and lead to delayed discharge. These concerns have led to use small doses of bupivacaine with or without opioids. Low dose spinal anaesthesia, which also provides excellent hemodynamic stability, can significantly extend the population of patients suitable for day surgery11-14. Local anaesthesia for knee arthroscopy is a well documented procedure that offers several advantages over other types of anaesthesia: complications are rare, cost of surgery is low and the patient is awake and can follow the procedure. 15, 16. Local anaesthesia alone is frequently insufficient to provide the patient with a comfortable operative experience. Local anaesthesia in combination with propofol sedation may enhance patient comfort without compromising rapid recovery.
In the present study we compared minidose bupivacaine spinal anaesthesia with local anaesthesia and propofol infusion for outpatient knee arthroscopy and found that preparation time was comparable in both the groups. One patient in local/propofol group received general anaesthesia (4.2%) which was comparable to previous study by Ben David et al12.
None of the patients in either of the groups had oxygen desaturation intraoperatively. In four patients airway obstruction was noted during procedure probably because of excessive sedation and airway support in the form of jaw lifting was done. In the study by Ben David et al12 20% patients had oxygen saturation less than 85% and 54% required some form of airway support.
Pain at the time of skin incision was present in 45% patient in local/propofol group where as none of the patients in spinal group complained of pain. Mean VAS score in local/propofol group was 0.9167(range 0-3) where as 0.00 in spinal group. In the study by Jacobson et al11 the mean VAS score in local group was 1.78 and median was 0.6, which is comparable to our study. In the study by Maldini et al17 more pain was experienced during injection of local anaesthetic than during the surgical procedure. In the study by Ben David et al12 many patients had substantial pain with the local anaesthesia technique and required titration of the propofol to levels of anaesthesia that were something more than “sedation” (total IV anaesthesia, TIVA, with spontaneous ventilation?).
Toshiaki et al18 studied pain during knee arthroscopy performed under local anaesthesia. The average VAS score describing pain during the procedure was 2.4 and satisfaction with pain control during the procedure received an average VAS score of 1.4. The pain scores in their study were comparable to our local/propofol group.
Data from a study in volunteers19 and another study in surgical patients20,21 suggests that a desired duration of 60 minutes surgical anaesthesia at the knee would require approximately 7.5 mg of bupivacaine. Using minidose spinal anaesthesia technique, doses as low as 6mg Vs 4mg of hyperbaric bupivacaine were compared for knee arthroscopy. Failure rates were 3/48 in the 4 mg group and 1/48 in the 6mg group. In our study there was no failure of subarachnoid block in any patient.
The time required to achieve a state of home-readiness (“fitness” for discharge home) is influenced by a wide variety of surgical and anaesthetic factors. However the major contributors to delays in discharge after ambulatory surgery 22, 23 are nausea, vomiting, dizziness, pain and prolonged sympathetic and/or motor blockade. The primary factors delaying discharge after spinal anaesthesia are recovery from theresidual motor blockade and sympatholytic effects of the subarachnoid block, contributing to delayed ambulation and inability to void.
The mean time to discharge in our study is 122 ± 19.55 minutes in spinal group and 60 ± 14.89 minutes in local/propofol group. The mean time to ambulation in our spinal group was 112.5 ± 25.7 0 minutes. The other variables that affect discharge in ambulatory patients like PONV and pain were comparable in both the groups. Time to discharge after administration of low dose bupivacaine (5-7.5 mg) is approximately 120 -180 minutes as reported by previous studies4, 19, 30, 31. In the study by Ben David et al 23 mean time to discharge were 187 ± 51 minutes. In their study discharge criteria included ability to void. The time to out of bed was 146±39 minutes, which is comparable to time of ambulation in our study. The time to urination in their study was 169 ± 32 minutes, which might be the cause of delayed discharge in their study. Ability to pass urine was not included in our discharge criteria because study by Mulroy et al 25 showed that ambulatory surgery patients can be discharged before voiding after short acting spinal and epidural anaesthesia. The post anaesthetic discharge score does not include voiding as a discharge criteria component.
Dahl et al27 reported that lignocaine of 1% or 1.5% can be used for intraarticular analgesia for knee arthroscopy. Maldini et al17 used 2% lignocaine with epinephrine 15 ml in their study. Patient comfort was satisfactory and no lignocaine toxicity was reported in the above studies. In our pilot study we used 30 ml of 1% lignocaine with epinephrine and patients were comfortable intraoperatively. So in the present study we used 1% lignocaine and no local anaesthetic toxicity was noted in any patients in our study.
Arthroscopic surgery has evolved from simple diagnostic and minor reconstructive procedures to complex reconstructive procedures done with arthroscopic aid. These more complex arthroscopic procedures require longer operative time, larger incision and more knee joint manipulations. To best of our knowledge thee are no reported studies of ligament reconstruction under LA with sedation. In our experience also LA is not ideal for above procedures with the present state of knowledge and techniques.
One limitation of our study was that the sample size of this study is not large enough to provide new information on the incidence of some less common side effects like post-dural puncture headache, TNS, urinary retention and local anaesthetic toxicity due to intraarticular injection. Serum lignocaine level was not measured due to practical reasons and documentation of serum lignocaine level would have given more confirmatory evidence regarding safety of intraarticular injection of LA. We suggest that future studies using long acting local anaesthetics like ropivacaine, levobupivacaine to maximize potential benefits of this technique. Considering the potential benefits with the LA/Propofol technique, we suggest anaesthesiologists and surgeons to re-examine their current clinical practice for outpatient knee arthroscopy.
Conflict of interest – None
REFERENCES
1. White PF, Smith I. Ambulatory Anaesthesia: past, present, and future. Int Anaesthesiol Clin 1994;32:1-16.
2 .Dahl V, Gierioff C, Omland E, Raeder JC. Spinal, epidural or propofol anaesthesia for outpatient knee arthroscopy? Acta Anaesthesiol Scand 1997;41:1341-1345.
3. Casati A, Capepelleri G, Fanelli G, Borghi B, Anelati D, Torri G: Regional anaesthesia for outpatient knee arthroscopy: a randomized clinical comparison of two different anaesthetic techniques. Acta Anaesthesiol Scand 2000;44:543–547.
4 . Jacbson E, Forssblad M, Rosenberg J, Westman L,Weidenhielm L. Can local anaesthesia be recommended for routine use in elective arthroscopy ? A comparison between local, spinal, and general anaesthesia. Arthroscopy 2000;16:183-190.
5. Ben-David B, DeMeo PJ, Lucyk C, Solosko D. A comparison of minidose lidocaine-fentanyl spinal anaesthesia and local anaesthesia/propofol infusion for outpatient knee arthroscopy. Anesth Analg 2001;93:319-325.
6. Dunn WR, Cordasco FA, Flynn E, Jules K, Gordon M, Ligouri G. A prospective randomized comparison of spinal versus local anaesthesia with propofol infusion for knee arthroscopy. Arthroscpy 2006;22:479-483.
7. Shapiro MS, Safran MR, Crocket H, Finerman GA. Local anaesthesia for knee arthroscopy: efficacy and benefits. Am J Sports Med 1995;23:50-53.
8. Watson B, Howell V. Spinal anaesthesia: The saviour of day surgery? Curr Anaesth & Crit Care 2007;18:193–199.
9. Shinder M, Ettlin T, Kauffman M, Schumacher P, Hampl K, Urwyler A et al. Transient neurologic symptoms after hyperbaric subarachnoid anaesthesia with 5% lidocaine. Anesth Analg 1993;76:1154-1157.
10. Freedman JM, Maria JC, De-Kun Li, Drasner K, Larsen B: Transient neurologic symptoms after spinal anaesthesia. Anesthesiology 1998;89:633-641.
11. Ben-David B,Frankel R, Arzumonov T, Marchevsky Y. Minidose bupivacaine –fentanyl spinal anaesthesia for surgical repair of hip fracture in the aged. Anesthesiology 2000;92:6-10.
12. Gurkan Y, Canatay H, Ozdmar D, Solak M and Toker K. Spinal anaesthesia for arthroscopic knee surgery. Acta Anaesthesiol Scand 2004;48:513-517.
13. Korhonen AM, Valanne JV, Jokela RM, Ravaska P, Korttila K. Intrathecal hyperbaric bupivacaine 3 mg + fentanyl 10µg for outpatient knee arthroscopy with tourniquet. Acta Anaesthesiol Scand 2003;47:342-346.
14. Cappelleri G, Aldegheri G, Danelli G, Marchetti C, Nuzzi M, Casati A et al. Spinal anaesthesia with hyperbaric levobupivacaine and ropivacaine for outpatient knee arthroscopy. Anesth Analg 2005;101:77-82.
15. Helmuth W. Trieshmann Jr. Knee Arthroscopy: A Cost Analysis of General and Local Anesthesia. Arthroscopy: 1996;12:60-63.
16. Shapiro MS, Safran MR, Crocket H, Finerman GA. Local anaesthesia for knee arthroscopy: efficacy and benefits. Am J Sports Med 1995;23:50-53.
17. Maldini B, Miskulin M. Outpatient arthroscopic knee surgery under combined local and intravenous propofol anaesthesia in children and adolescents. Paediatr Anaesth 2006;16:1125-1132.
18. Toshiaki T, Tanaka M, Ikeuchi1 M, Sadahiro T, Tani T. Pain in arthroscopic knee surgery under local anaesthesia. Acta Orthop Scand 2004;75(5):580–3.
19. Liu SS, Ware PD, Allen HW et al. Dose-response characteristics of spinal bupivacaine in volunteers: Clinical implications for ambulatory anesthesia. Anesthesiology 1996;85:729-736.
20. Ben-David B, Levin H, Solomon E, Admoni H, Vaida S. Spinal bupivacaine in ambulatory surgery: The effect of saline dilution. Anesth Analg 1996;83:716-720.
21. Liu SS. Optimising spinal anesthesia for ambulatory surgery. Reg Anesth 1997;22:500-510.
22. Pavlin DJ, Rapp SE, Polissar NL, et al. Factors affecting discharge time in adult outpatients. Anesth Analg 1998;87:816-26.
23. Chung F, Mezei G. Factors contributing to a prolonged stay after ambulatory surgery. Anesth Analg 1999;89:1352–1359.
24. Chung F, Chan V, Ong D. A post-anesthetic discharge scoring system for home-readiness after ambulatory surgery. J Clin Anesth 1995;7:500–506.
25. Mulroy MF, Salinas FV, Larkin KL, Polissar NL. Ambulatory patients may be discharged before voiding after short acting spinal and epidural anaesthesia. Anesthesiology 2002;97:315-319.
26.Song D, Greilich NB, White PF, et al. Recovery profiles and costs of anesthesia for outpatient unilateral inguinal herniorrhapy. Anesth Analg 2000;91:876–881.
27. Dahl MR, Joseph FD, Zuelzer W, McSweeney TD. Lidocaine local anaesthesia for arthroscopic knee surgery. Anesth Analg 1990;71:670-674.
28. Hultin J, Hamberg P, Stenstrom A. Knee arthroscopy under local anaesthesia. Arthroscopy 1992;8:239-241.
Table 1: Demographic Data (Mean ± SD)
| Group I | Group II | P value | |
| Age (years) | 29.9 ± 9.4 | 30.1±11.2 | 0.933 |
| Weight (kg) | 173.12 ± 8.70 | 171.29 ± 6.87 | 0.416 |
| Height(cm) | 71.73 ± 13.66 | 69.28 ±11.21 | 0.481 |
| Male/Female | 21/5 | 19/5 | 0.582 |
| ASA status (class I/II) | 26/0 | 23/1 | 0.480 |
| Preparation time (min) | 14.23 ± 4.4 | 15.00 ± 5.89 | 0.602 |
| Duration of surgery (min) | 54.04 ± 20.83 | 45.00 ± 8.99 | 0.095 |
Table 2: Patients requiring airway support/ GA, pain at skin incision
| Group I
n =26 |
Group II
n =24 |
P value | |
| Required GA | 0 (0%) | 1 (4%) | 0.48 |
| Airway support | 0 (0%) | 4 (14%) | 0.02 |
| a. Face mask | 0 | 1 | > 0.05 |
| b. Jaw lifting | 0 | 3 | > 0.05 |
| Pain at skin incision (mean ± SD) | 0 ± 0.00 | 0.92 ± 1.13 | 0.001 |
| No of patients with VAS 0 | 26 | 14 | 0.01 |
| No of patients with VAS 2 | 0 | 8 | 0.01 |
| No of patients with VAS 3 | 0 | 2 | 0.225 |
Table 3: Oral intake, discharge, hospital stay, nausea/vomiting, rescue analgesia (Mean ± SD)
| Group I | Group II | P value | |
| Oral intake (min) | 46.92 ± 13.7 | 35.41 ± 8.19 | 0.729 |
| Ambulatory (min) | 112.50 ± 25.7 | 30.83 ± 9.16 | 0.001 |
| Time of discharge (min) | 122.11 ± 19.55 | 60.00 ± 14.89 | 0.001 |
| Total hospital stay (min) | 180.38 ± 33.51 | 94.50 ± 29.20 | 0.001 |
| No of patients requiring rescue analgesia | 3 (11.5%) | 6 (25%) | 0.193 |
| Timings to first rescue analgesics (min) | 75 | 45 | |
| No of patients with vomiting | 2 | 2 | 0.664 |
Fig 1: Postoperative VAS Score (Mean)
Fig 2: Discharge and hospital stay