Neha Singh, MD*, Parnandi Bhaskar Rao, MD, PDCC**, Sushil Prakash Ambesh, MD***, Devendra Gupta, MD, PDCC***
*Department of Anesthesiology, Critical Care and Pain Medicine, IMS and SUM Hospital, Bhubaneswar-751030, Odisha (India). **Department of Anesthesiology, Critical Care and Pain Medicine, AIIMS, Bhubaneswar- 751019, Odisha (India).
***Department of Anesthesiology, Intensive Care and Pain Medicine, SGPGIMS, Lucknow- 226014 (India).
Correspondence: Dr. Neha Singh, MD, Department of Anesthesiology, Critical Care and Pain Medicine, IMS and SUM Hospital, Bhubaneswar-751030, Odisha (India). Email: hinehabhu@rediffmail.com
The use of laryngeal mask airway (LMA®; Laryngeal Mask Company, Henley-on-Thames,UK) has been well established for airway management. It is difficult to place a nasogastric tube with a properly positioned Classic LMA®. The technique of inserting nasogastric tube with the help of passing nasal red rubber tube is difficult to perform and associated with a risk of trauma.1 We used a new method of nasogastric tube insertion using a polyvinyl chloride (PVC) endotracheal tube.
A 45-year-old male patient weighing 78 kg was brought for appendectomy. Patient was nil by mouth for eight hours. General examination was normal but systemic examination revealed marked abdominal distension, generalised abdominal tenderness and sluggish bowel sounds. Routine blood investigations were normal and the patient was taken up for surgery.
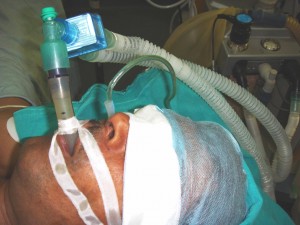
The venous access was secured with two 18G intravenous cannulae and standard monitors attached. Patient was premedicated with midazolam (0.04 mg/kg) and fentanyl (2 µg/kg). Induction was achieved with inj. propofol (2 mg/kg) and inj. Succinylcholine 1.0 mg/kg after ensuring for adequacy of ventilation. Following several failed intubation attempts, airway was secured with size 3 Classic LMA® and cuff was inflated with 20 ml of air. Effectiveventilation was judged by observation of chest wall movement, a square wave capnograph and by auscultation for bilateral breath sounds. The surgeons insisted for a nasogastric tube placement for gastric evacuation. After due checking for obstruction and deviated nasal septum the nostrils were prepared with a vasoconstrictor agent. A well lubricated size 5.0 uncuffed PVC tube was threaded over nasogastric tube which was placed in the prepared nostrils along with nasogastric tube tip placed at the tip of PVC tube. Correct position of nasogastric tube was confirmed by injection of air and auscultation over the epigastrium. The stomach was aspirated for any contents and surgery was uneventful (Figure 1).
Figure 1: LMA with NG tube passed through nasal ETT
The esophageal inletmay not be sealed at all times because of the technical design of the LMA. Use of LMA is associated with potential risk of aspiration. Studieshave found an incidence of 6% to 35% visualization of the esophagus through theLMA and thus regurgitation of gastric contents.2-3 Lower esophageal tone is also reduced with LMA.4 The technique used by us is easy but not a new one. In difficult cases same technique has been used, especially in ICU setting, but its use with an LMA has not been reported.
REFERENCES
- Dutta A, Ganguly N, Sood J, Kumra VP. Intraoperative Nasogastric Tube Insertion with Non-ProSeal Laryngeal Mask Airway in Place. Anesth Analg 2006;102:1294-95. [PubMed]
- Fullekrug B, Pothmann W, Werner C, Schulte am EJ. The laryngeal mask airway: anesthetic gas leakage and fiberoptic control of positioning. J Clin Anesth. 1993 Sep-Oct;5(5):357-63. [PubMed]
- Valentine J, Stakes A.F,Bellamy M.C. Reflux during positive pressure ventilation through the laryngeal mask. Br J Anaesth. 1994;73:543-44. [PubMed] [Free Full Text]
- Rabey PG, Murphy PJ, Langton JA, Barker P, Rowbotham DJ. Effect of the laryngeal mask airway on lower oesophageal sphincter pressure in patients during general anaesthesia. Br J Anaesth. 1992;69:346-8. [PubMed]