Tanvir Samra, MBBS, MD*, Neha Sharma, MBBS**
*Assistant Professor, **IInd Year Post graduate student (MD Anaesthesia)
*Department of Anesthesiology, Lady Hardinge Medical College, New Delhi 110001 (India);
Correspondence: Dr Tanvir Samra, C-II/ 77, Moti Bagh 1, New Delhi-110021 (India);E-mail: drtanvirsamra@yahoo.co.in; Phone: 9910703609
Bupivacaine is the most commonly used local anesthetic for epidural and spinal anaesthesia; retrobulbar and peripheral nerve blocks and local infilteration.1 Topical use of bupivacaine for urethral and ocular anesthesia is reported in various clinical studies.2,3 Intramuscular injection of 0.5% bupivacaine at cervical spinous process alleviates headache.4 Enhancement of hypnotic effect of propofol have been documented by prior administration of intramuscular bupivacaine.5
Bupivacaine is contraindicated in patients with known hypersensitivity to local anesthetic agents of the amide group or to other components of the injectable formulation and for intravenous regional anaesthesia (Bier’s block). Bupivacaine hydrochloride (0.75% ) is not recommended for obstetric anesthesia. Use of intra articular infusions of local anesthetics is not approved in view of post-marketing reports of chondrolysis in patients receiving such infusions.
Hypobaric multidose vials contain antiseptic preservative methylparaben which is implicated as the causative agent for allergic reactions and chronic adhesive arachnoiditis.1 Safety of preservatives has not been established with regard to intrathecal injection also. These vials are thus used for infilteration and nerve blocks only; preservative free preparations are preferred for caudal, epidural and spinal anaesthesia.
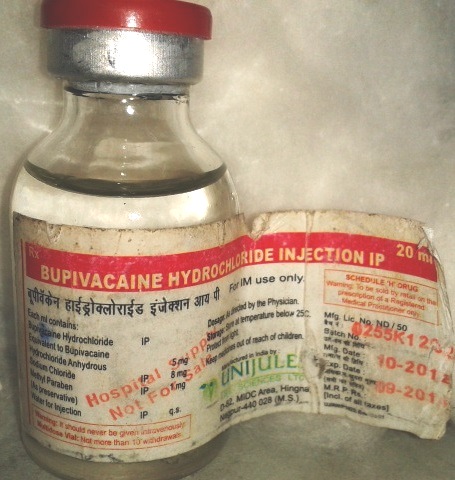
In our public sector hospital bulk purchase of drugs and anesthetic agents is done as per need. The bupivacaine multidose vials supplied to the hospital (Figure 1) a few months back were unique as they were labelled “ For IM use only” by the manufacturer. To our knowledge there is no formulation of bupivacaine which has been marketed for intramuscular use. There was no change in the drug composition of these ‘new’ multidose vials; it contained bupivacaine (0.5%), methylparaben (1 mg/ml), sodium chloride and water. The new label on the vials was initially missed by some anesthesiologists and 25 patients had already received either nerve block or local infilteration by the time this error was noted. These patients were followed up for a period of one month but none of them complained of any adverse effect. The manufacturer was informed of the error and the drugs were returned.
Medication error is defined as “any preventable event that may cause or lead to inappropriate medication use or patient harm while the medication is in the control of the health care professional, patient, or consumer. Error can occur at level of drug prescribing; product labelling, packaging and nomenclature; compounding; dispensing; distribution; administration; education; monitoring; and use. The anesthesiologist must take appropriate steps to minimise the same. Any contraindication for administration of the drug to the patient also needs to be ruled out.
REFERENCES
- Berde CB, Strichartz GR. Local Anaesthetics; In Miller RD. ed. Miller’s Anaesthesia 6th ed. Philadelphia, Churchill Livingstone; 2005:.p.583-592.
- Dawkins GP, Harrison NW, Ansell W. Urethral anaesthesia with topical bupivacaine. A role for a longer-acting agent. Br J Urol 1995 ;76:484-7. [PubMed]
- Soliman MM, Macky TA, Samir MK. Comparative clinical trial of topical anesthetic agents in cataract surgery: lidocaine 2% gel, bupivacaine 0.5% drops, and benoxinate 0.4% drops. J Cataract Refract Surg 2004;30:1716-20. [PubMed]
- Mellick LB, McIlrath ST, Mellick GA. Treatment of headaches in the ED with lower cervical intramuscular bupivacaine injections: a 1-year retrospective review of 417 patients. Headache 2006 ;46:1441-9. [PubMed]
- Senturk M, Pembeci K, Menda F, Ozkan T, Gucyetmez B, Tugrul M, Camci E, Akpir K. Effects of intramuscular administration of lidocaine or bupivacaine on induction and maintenance doses of propofol evaluated by bispectral index. Br J Anaesth 2002;89:849-52. [PubMed] [Free Full Text]