Dilip Kothari1, Sameer Gupta2, Anju Gautam3, Shilpa Agrawal4
1Professor; 3Assistant Professor; 4P.G. Medical Officer
Department of Anesthesiology, G. R. Medical College & J. A. Group of Hospitals, Gwalior (India)
2Assistant Professor, Department of Surgery, G. R. Medical College & J. A. Group of Hospitals, Gwalior (India)
Correspondence: Dr. Dilip Kothari. E-mail: drdilip_kothari@yahoo.co.in
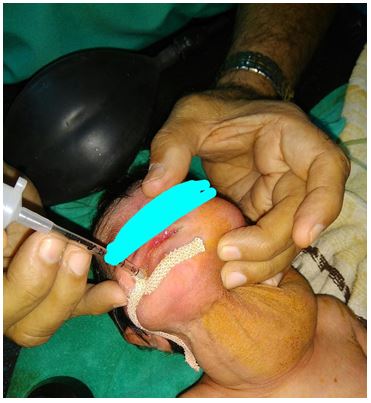
A 6 days old female neonate with huge cystic hygroma (Figure 1 & 2) was shifted in emergency from ward to operating room (OR) with cyanosis, respiratory obstruction and drowsiness. On examination her heart beat was 140 /min, respiratory rate 40 /min and SpO2 74% on air. No other investigations were available.
Oropharyngeal suction was done. O2 supplementation improved her color and SpO2 rose to 93%. Awake oral laryngoscopy was done but epiglottis was not visible due to huge cystic swelling.
As FOB or SGAD were not available, so it was decided to aspirate fluid from the swelling with an 18 G needle to reduce the size of swelling to facilitate the intubation.
Once swelling was reduced (Figure 3) intubation with 2.5 mm ETT was possible after O2 and sevuflurane induction (Figure 4). It improved her oxygenation and all vital signs. The surgery was deferred till blood was arranged. Extubation was done once extubation criteria was met.
[Permission from patient’s relative and the surgeon obtained for teaching purpose]
Figure 1: Cystic Hygroma Front View
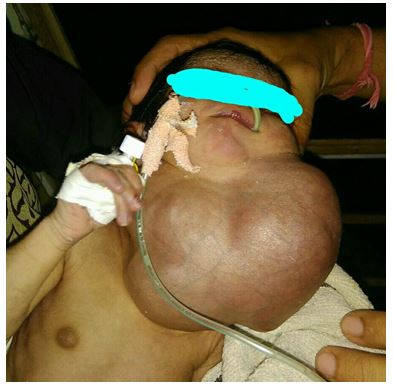
Figure 2: Cystic hygroma, lateral view
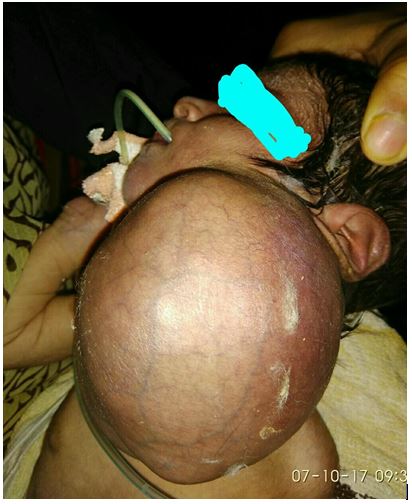
Figure 3: After aspiration of fluid
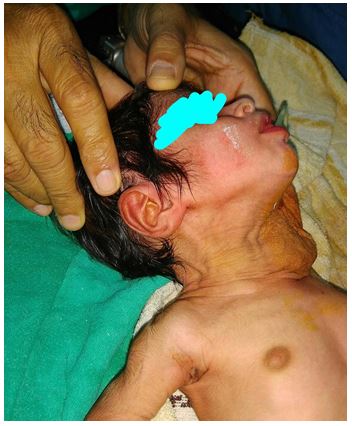
Figure 4: After orotracheal intubation