Anju Ghai, MD*, Meenu goyal, MD**, Raman Wadhera, MS***, Manish kumar goel, MD****
*Associate Professor, **Assistant Professor, Department of Anesthesiology
***Associate Professor & Head, Department of ENT
****Assistant Professor, Department of Community Medicine
Pt. B.D. Sharma Postgraduate Institute of Medical Sciences, Rohtak (India)
Correspondence: Dr. Meenu goel, M.D., Assistant Professor, Department of Anesthesiology, Pt. B.D. Sharma Postgraduate Institute of Medical Sciences, Rohtak (India); Phone: 09416538815; E-mail: meenu297@yahoo.com
ABSTRACT
Massive subcutaneous emphysema is a rare complication of interventional bronchoscopy. Complications reported include laryngeal and bronchial spasm, hematorrhea, arrhythmia, airway obstruction, tracheoesophageal fistula, and pneumothorax. Massive subcutaneous emphysema is a rare complication of rigid bronchoscopy. There has been no case report mentioned in the literature till date to the best of our knowledge. We report an eighteen months old female child who developed emphysema involving upper third of her chest, neck and face after rigid bronchoscopy, which increased progressively threatening closure of the airways but was successfully managed conservatively. The details of this case and the management are discussed.
Keywords: Subcutaneous emphysema; Rigid bronchoscopy; Stridor; Bronchodilators; Bronchospasm
Citation: Ghai A, Goyal M, Wadhera R, Goel MK. Massive subcutaneous emphysema secondary to rigid bronchoscopy in a child. Anaesth Pain & Intensive Care 2012;16(3):293-295
INTRODUCTION
Bronchoscopy is a widely performed procedure and is generally considered to be safe and effective. Reported rate of severe complications of bronchoscopy and mortality is 0.739% and 0.013% respectively.1 Complications reported include laryngeal and bronchial spasm, hematorrhea, arrhythmia, airway obstruction, trachea-esophageal fistula, and pneumothorax. A case of massive subcutaneous emphysema secondary to rigid bronchoscopy causing a serious risk to airway, which was managed conservatively, is being described here.
CASE REPORT
An 18 months old female child presented to the hospital emergency department with history of difficulty in breathing for the previous ten days. She had been on treatment for laryngotracheobronchitis and status asthmatics. There was inadequate relief after treatment with antibiotics and bronchodilators. The respiratory distress had increased for the last four days.
At the time of presentation the child was very sick-looking; her pulse rate was 160 beats/min and respiratory rate was 46/min. She had expiratory stridor with chest indrawing and accessory muscles being used. Auscultation revealed bilateral bronchospasm and decreased air entry on right basal lobe. Chest x-ray showed hyperlucent right lower zone. On enquiring in detail, the mother revealed history of handling of groundnuts by the child when the episode of choking followed by tearing of the eyes started. The child was slightly relieved after a thrust on back, but the difficulty in breathing persisted. An urgent bronchoscopy was planned.
In the operating room, after securing an intravenous line, monitors were attached for SpO2, ECG and heart rate. Oxygen saturation (SpO2) was 90%. Patient was induced with inj. ketamine 40 mg and inj. suxamethonium 10 mg. Rigid bronchoscope size 3.5 was introduced. Inj. atracurium was given. After about ten minutes, a sudden fall in SpO2 and bradycardia was noticed. Bronchoscope was immediately removed by the surgeon. A gush of blood was noticed coming through oral cavity. The child was immediately intubated with 3.5 mm endotracheal tube and suction done. Chest auscultation revealed severe bronchospasm bilaterally. Saturation dipped to 85% even with ventilation with 100% oxygen through the ETT. Endotracheal suction was done. Child was nebulized with adrenaline and salbutamol solution. Injection hydrocortisone 40 mg IV and terbutaline 8 mg SC was administered. Saturation improved up to 94%. After a few minutes, bronchospasm got relieved and the saturation rose to 98%. The child was extubated with adequate spontaneous respiratory effort. We continued intermittent nebulization with adrenaline and salbutamol solutions. After about ten minutes surgical emphysema was noticed in left chin area, which rapidly increased with strenuous coughing. It then spread to her neck and face including the lower eyelid and to upper chest lower down. The child was fully awake and crying, and saturation of 95-100% with oxygen was maintained. The emphysema increased with coughing and crying and got localized to the above-mentioned areas. She did not have any difficulty in breathing, yet massive emphysema encircling around the neck was a potential threat to the airway, which could lead to complete obstruction of the airways any time. So, consultation with cardiothoracic surgeon was sought. A chest x-ray revealed no evidence of pneumothorax. Hence, introduction of the chest drain was deferred. Patient was kept under close observation overnight, keeping emergency airway management cart standby. A digital chest x-ray was ordered, which revealed subcutaneous emphysema in right chest wall and neck.
On the next day, CT scan of the thorax revealed subcutaneous emphysema, pneumothorax and pneumomediastinum on right side of the chest. Linear adhesions and fibrous bands were seen at the lower end of the trachea and at the origin of right main bronchus. There was a breach in the posterior wall of the right main bronchus at the subclavian level with an accumulation of air adjacent to it. There was also consolidation of the right lower lobe of the lung. The child’s vital signs remained stable and the subcutaneous emphysema reduced slowly over the next two days. She was managed conservatively with bronchodilators and nebulised four hourly for bronchospasm. After two days a chest x-ray was repeated, which showed absence of pneumomediastinum, insignificant pneumothorax and no collapse. After discussion with the surgeons, it was planned to manage the child conservatively, as patient’s respiratory status had improved significantly. Patient was followed up to seven days. She regained normal activity and was discharged thereafter.
DISCUSSION
Rigid bronchoscopy is widely used for the diagnosis and/or therapy of many lung and airway diseases. Concern has been raised about its complications. The bleeding and emphysema in our patient was due to an iatrogenic injury to the bronchial wall in an attempt to remove the peanut piecemeal. The complications involving the airway were managed successfully with intubation and repeated endobronchial suctioning.
In suspected injury to the airways it is probably better to allow the patient to resume spontaneous respiration. IPPV needs to be deferred and early extubation should be planned in such cases, so as not to exaggerate the airway injury. We extubated when the child was fully awake with adequate motor tone with no evidence of further bleeding from the airway. Though emphysema did not become apparent immediately as there was just a breech in posterior wall of right bronchus, it became evident by sudden intra-bronchial high pressures caused by coughing. The strenuous cough could have widened the tear and increased the air leakage thereby causing pneumothorax. Our patient had subcutaneous emphysema of chin, neck and upper chest, which progressively increased, spreading to whole of the neck and face. Jougon et al suggested that surgical intervention should be recommended at an early stage and depends on length and depth of the lesion, the degree of subcutaneous emphysema, pneumothorax and/or pneumomediastinum as well as clinical signs suggestive of any mediastinitis.2 In our patient there was no evidence of pneumothorax on chest x-ray. As the choice between conservative and surgical treatment is variable depending upon clinical findings, chest tube drainage was deferred. The absence of pneumothorax could be attributed to the presence of an incomplete breach in the bronchial wall. Bronchodilators, antibiotics and nebulization were the main stay of treatment. The child maintained the saturation throughout and clinical regression of surgical emphysema and respiratory distress was evident in the next 24-48 hours.
Other reported causes of subcutaneous emphysema in the peri-operative period can be trauma to the pharynx, esophagus or trachea from laryngoscopy, intubation, overinflation of endotracheal tube and gastric tube placement.3,4 Surgical emphysema can also be a rare manifestation of foreign body aspiration.5
We conclude that subcutaneous emphysema with extension into soft tissue planes of the supraglottic airway can be a possibility after rigid bronchoscopy and should be kept in mind. Unnoticed, it may rapidly lead to airway compromise and should be recognized promptly to secure the airway promptly before distortion of the airway anatomy makes intubation difficult or even impossible.
REFERENCES
- Jin F, Mu D, Chu D, Fu E, Xie Y, Liu T. Severe Complications of Bronchoscopy. Respiration. 2008;76(4):429-33 [Medline]
- Marty-Ané CH, Picard E, Jonquet O, Mary H. Membranous tracheal rupture after endotracheal intubation. Ann Thorac Surg. 1995;60:1367–71 [Medline]
- Levine PA. Hypopharyngeal perforation an untoward complication of endotracheal intubation. Arch Otolaryngol. 1980;106:578–80. [Medline]
- Gupta RK, Gupta A, Sanghvi B, Parelkar SV, Mishra P. Subcutaneous Emphysema: An Unusual Presentation of Foreign Body Aspiration. J Bronchology Interv Pulmonol. 2009;16(2):124-6 [Medline]
- Jougon J, Cantini O, Delcambre F, Minniti A, Velly JF. Esophageal perforation: life threatening complication of endotracheal intubation. Eur J Cardiothorac Surg. 2001;20:7-10 [Medline]
Illustrations
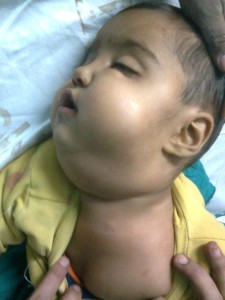
Fig 1: Subcutaneous emphysema of the neck and face of the child