Nidhi Garg, Maya Dehran
Department of Anesthesiology,All India Institute of Medical Sciences, New Delhi (India)
Correspondence: Dr. Nidhi Garg, FTA 106, Ayurvigyan Nagar, New Delhi (India); Email: nidhigarg25084@gmail.com
ABSTRACT
Effective airway management includes anticipating and planning for problems. Difficulties frequently occur as the result of patient characteristics that interfere with spontaneous breathing, bag mask ventilation, laryngoscopy or intubation of the trachea. We are presenting here a case report of a 5 year old child with large sublingual dermoid with bilateral adenoid hypertrophy where successful intubation was done with the use of GlideScope®.
Keywords: GlideScope®, sublingual dermoid, difficult pediatric airway, adenoid hypertrophy
Citation: Garg N, Dehran M. GlideScope: A rescuer in difficult pediatric airway. Anaesth Pain & Intensive Care 2014;18(1):43-45
INTRODUCTION
Epidermoid and dermoid cysts are benign lesions which can be present anywhere in the body but 7% occurs in head and neck area and 1.6% within the oral cavity.1 They represent less than 0.01% of all oral cavity cysts.2 Dermoid cysts generally present with slow and progressive growth. However, they may reach a large size, involve more than one anatomical area and can abut the hyoid bone when in the neck.3 Intraorally this benign slow growing and painless entity is usually located in the submandibular, sublingual and submental region. They can cause symptoms of dysphagia and dyspnoea and have a malignant transformation potential. Surgical excision by intraoral or extraoral route depending on the localization and size of the mass is the treatment of choice.4
Airway management has always been a challenge to the anesthesiologist. One has to balance between patient comfort and cooperativeness versus the technique of anesthesia induction especially when the patient is a child. The anaesthesiologist approaching the patient with a difficult airway has a variety of techniques and instruments which can be utilised to secure and maintain the airway, oxygenation and ventilation.5
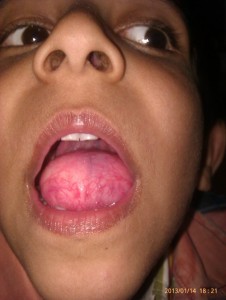
In this article, we are reporting the case of a sublingual dermoid cyst with bilateral adenoid hypertrophy in a 5 year old boy. The big size (6×4 cm) sublingual cyst was pushing the anterior part of the tongue posteriorly. Unless the child was asked to protrude the tongue, the anterior part of the tongue was not visible and there was associated grade 2 adenoid hypertrophy as well. In view of all this, the child became a case of difficult airway.
CASE REPORT
A 5 year old male patient weighing 19 kg was posted for excision of sublingual dermoid cyst. He was admitted in the otolaryngology department with complaints of a mass in the oral cavity and difficulty in breathing with increased snoring for the past 1 1/2 years. Initially the cyst was pea sized and had gradually increased to the present size. There was history of excess snoring with increasing sleepiness in day time.
On examination, there was a 60 × 40 mm sublingual mass with normal covering mucosa displacing the tongue superiorly and posteriorly (Figure 1). Neck examination revealed a firm swelling in the submental area. Airway examination revealed bilateral tonsillar hypertrophy. On nasal patency test, right nostril was slightly patent but left nostril was totally obstructed. A CT scan showed well-circumscribed non-enhancing mass in the sublingual area and grade-2 adenoid hypertrophy. Parents were explained about the difficult airway situation and that the child might need awake intubation, possibility of tracheostomy and of post operative need of ICU stay. Premedication was avoided in view of difficult airway. Plan was to try inhalational induction maintaining spontaneous respiration and to do a check laryngoscopy. In the operation theatre, 22G intravenous cannula was inserted and all standard monitors were attached. Difficult airway management cart was kept ready. The pharynx was anaesthetized topically using 4% viscous lidocaine. Inhalation induction was started with increasing concentrations of sevoflurane but with increasing depth of anesthesia we were not able to maintain the airway because of large intraoral mass pushing the tongue posteriorly and near complete nasal blockade. The child became very restless, so sevoflurane was discontinued and the child was awakened with 100% oxygen. Lignocaine spray (10%) and gargles were repeated twice and the child was explained about the need for his cooperation. Then direct laryngoscopy was attempted and we could see only the posterior commissure. As the child was awake and moving, we could not negotiate the endotracheal tube. At this stage, GlideScope® was brought in, as its use does not need too much manipulation of airway to visualise epiglottis and glottic opening. We succeeded in visualising and intubating the trachea with 5.5 mm uncuffed endotracheal tube without any coughing, bucking and bronchospasm. A bolus of propofol 50 mg and fentanyl 20 µg was given. Anesthesia was maintained using oxygen, N2O, isoflurane, atracurium and fentanyl infusion (1µg/kg/hr). Extraorally, a midline sub mental horizontal incision was made through the mucosa overlying the swelling and the cyst was dissected from the surrounding tissues and removed (Figure 2). Rest of the surgery was uneventful and duration of surgery was 1 hr with minimal blood loss. Following surgery neuromuscular blockade was reversed and the trachea extubated when the child’s protective reflexes appeared and he started responding to verbal commands. The child was shifted to PACU with oxygen therapy and pulse oximetry monitoring. The patient did well in postoperative period.
DISCUSSION
Difficult airway in pediatric population presents its own unique challenges. Difficulty in managing the anatomical and functional aspects of pediatric airway and decreased cardiorespiratory reserve makes the job of an anesthesiologist hugely challenging. To compound the matter further, if some lesion is present on any part of this anatomical track, the degree of difficulty increases manyfold.6 The airway management of such challenging cases has to be planned precisely especially in pediatric age group. In our case, the degree of difficulty was associated with many other challenges as well. Not only the site and size of the lesion carried the risk of difficulty in ventilation and intubation, adenoid hypertrophy too added much scores to the predicted difficulty.
Our plan was to try inhalational induction maintaining spontaneous respiration but we were not able to maintain the airway because of large intraoral mass and near complete nasal blockade. Then awake intubation under local anesthesia was planned. So airway was anaesthetised using lignocaine spray (10%) and gargles. First, we did check laryngoscopy using Macintosh blade. We could see only the posterior commissure but could not negotiate the endotracheal tube. Then we thought of using the GlideScope® and we succeeded in visualising and intubating the trachea. The GlideScope® is designed to allow a view of the glottis with a camera without the alignment of oral, pharyngeal, and tracheal axes and also without any additional lifting force. It may facilitate tracheal intubation in patients with abnormal upper airways, not only by improving the laryngoscopic view, also by virtue of its indirect (videoscopic) nature. With visualization of the tube and glottis, adjustments may be performed allowing the tube to gently pass through the vocal cords.7 The initial work on GlideScope® in normal pediatric populations showed that it provided a laryngoscopic view equal to or better than that of direct laryngoscopy but required a longer time for intubation.8,9 However, a study by Redel and colleagues also showed improved intubating conditions, but with no difference in time taken to intubation.10
To the best of our knowledge, there is no such case reported in literature in pediatric patient with both intraoral and nasal obstruction. In such difficult airway situation, the GlideScope may be a useful tool for facilitating the intubation.
CONCLUSION
In children with known difficult airway, or in patients with a suspected difficult airway, where no previous anaesthetics have been performed to confirm this, the use of GlideScope® , with and without manual external laryngeal pressure, significantly improves the Cormack and Lehane grade at laryngoscopy and facilitates orotracheal intubation.
REFERENCES
- Turetschek K, Hospodka H, Steiner E. Case report: epidermoid cyst of the floor of the mouth: diagnostic imaging by sonography, computed tomography and magnetic resonance imaging. Br J Radiol. 1995;68:205–7. [PubMed]
- Rajayogeswaran V, Eveson JW. Epidermoid cyst of the buccal mucosa. Oral Surg Oral Med Oral Pathol. 1989;67:181–4. [PubMed]
- Bitar MA, Kumar S. Plunging congenital epidermoid cyst of the oral cavity. Eur Arch Otorhinolaryngol. 2003;260:223–5. [PubMed]
- Longo F, Maremonti P, Mangone GM, De Maria G, Califano L. Midline (dermoid) cysts of the floor of the mouth: report of 16 cases and review of surgical techniques. Plast Reconstr Surg.2003;112:1560–5. [PubMed]
- William h., Rosenblatt, Airway management, clinical anesthesia 4th ed 2001, 619.
- Stringel G, Mercer S. Giant hemangioma in the newborn and infants. Clin Pediatr.1984;23:498–502. [PubMed]
- Karsli C, Armstrong J, John J. A comparison between the GlideScope Video Laryngoscope and direct laryngoscope in pediatric patients with difficult airways – a pilot study. Anesthesia 2010;65:353–7. [PubMed]
- Kim JT, Na HS, Bae JY, et al. GlideScope – video laryngoscope: a randomized clinical trial in 203 pediatric patients. British Journal of Anesthesia 2008;101:531–4. [PubMed] [Free Full Text]
- John J, Karsli C, Luginguehl I, Bissonnette B. Pediatric airway management using the GlideScope – video laryngoscope. Anesthesiology 2006;105:A1151.
- Redel A, Karademir F, Schlitterlau A, Frommer M, Scholtz LU, Kranke P, et al. Validation of the GlideScope video laryngoscope in pediatric patients. Paediatr Anaesth. 2009 Jul;19(7):667-71. [PubMed] doi: 10.1111/j.1460-9592.2009.03046.x.
Figure 1: Child with large sublingual dermoid
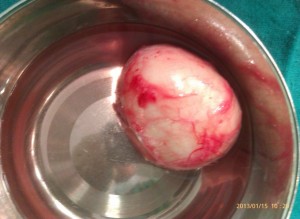
Figure 2: Excised dermoid cyst