Muhammad Shafiq*, Riaz Ahmed Khan**, Muhammad Iqbal*, Hamraz Khan***
*Assistant Professor, **Associate Professor & HoD, ***Head Nurse
Department of Anesthesiology & Critical Care, Rehman Medical Institute, Peshawar (Pakistan).
Correspondence: Dr. Muhammad Shafiq, Surgical ICU, Rehman Medical Institute, Peshawar (Pakistan); E-mail: shafiqkhan2010@yahoo.com.
ABSTRACT
In this case report, we describe the management of a patient with postnatal sepsis caused by retained infected products of conception (POC), who developed lung collapse due to mucus plugs. She had polymodal therapy including frequent hemodialysis. After removal of POC, she was shifted to Surgical Intensive Care Unit (SICU) for critical care including ventilatory support. The next day she was extubated, but on the third day she developed left lung collapse due to mucus plug resulting in ipsilateral lung collapse. Bronchoscopic lavage was considered hazardous by the pulmonologist due to her poor general condition. She was intubated and removal of the mucus plugs was attempted through sterile endobronchial tube suction which resulted in re-expansion of the collapsed lung. The lung remained expanded in her follow up. This method may be used at centers where facilities or expertise for bronchoscopy is not available.
Key Words: Sepsis; Atelectasis; Bronchoscopic lavage
Citation: Shafiq M, Khan RA, Iqbal M, Khan H. Bronchopulmonary lavage and re-expansion of the atelectatic lung without bronchoscopy. Anaesth Pain & Intensive Care 2011;15(3):173-175.
INTRODUCTION
The use of fiberoptic bronchoscopy (FOB) for atelectasis and clearing retained lung secretions has become common place in the ICU´s. In a meta analysis from 1966 to July 2002, bronchoscopy had been moderately effective in removing retained secretions and improving atelectasis with a wide range of success rate (19-89%)1. Broncho-alveolar lavage (BAL) improves its efficacy2 and many authors advocate the use of affected lung or segmental insufflations with different methods like the use of balloon-cuffed rigid bronchoscope3 and balloon cuffed flexible bronchoscope4, which are generally not available. Even FOB requires availability, expertise and cost, and its use is associated with physiologic disturbances. We describe a successful re-expansion of an affected lung by placing cuffed endotracheal Tube (ETT) in the principal bronchus of the affected lung to clear mucus followed by insufflations.
CASE REPORT
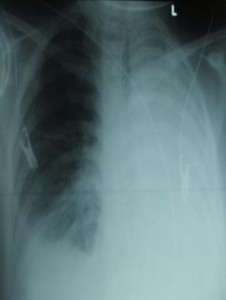
A 35 years old Afghan lady reported with history of recent normal vaginal delivery at home. She developed severe sepsis due to infected retained POC and was admitted to SICU with renal and respiratory failure. Surgical evacuation under General Anesthesia (GA) was done. Postoperative ventilatory support was provided due to her poor inspiratory effort. She was successfully weaned off the ventilator after 24 hours and was extubated, but just after 24 hours, left lung collapse was detected clinically and was confirmed radiographically (Fig 1). Immediate nebulization of a bronchodilator drug, chest physiotherapy and frequent suctioning of the airways were instituted. Supplementary oxygen at the rate of 6 l/min by face mask produced satisfactory SpO2.
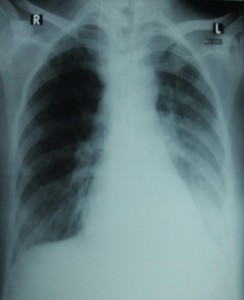
Chest physician’s opinion was asked who showed reluctance to attempt FOB removal of the mucus plugs due to a very poor general condition of the patient. A decision was taken to attempt re-expansion using ETT and blind transtube suction. An informed consent was obtained from the patient’s relatives. A cuffed ETT of 6 mm internal diameter (ID) was prepared by loading with a lubricated stylet and bent anteriorly. The patient was gently placed in left lateral posture. She was induced with 2 mg of inj. midazolam. Neuromuscular paralysis was achieved by suxamethonium chloride 40 mg. The patient was oxygenated with Ambu® self-inflating bag using high flow of oxygen. ETT was passed after recognizing vocal cords on direct laryngoscopy to midtracheal position and then it was rotated 90º anticlockwise and advanced up to 24 cm mark in front of lower incisors to guide it into left main bronchus. The cuff was inflated with little volume of air and the stylet was withdrawn. Correct placement was confirmed clinically. Gentle/sterile suction was done through ETT by sterile suction catheter to clear left main bronchus. N-acetyl cysteine (Mucolator®) 200mg dissolved in 3 ml of normal saline was instilled through ETT and the patient was ventilated gently. The ETT, after deflating its cuff, was withdrawn to mid-tracheal position and now the patient was placed in right lateral posture. Left chest percussion was done. Secretions returning from left lung were aspirated. Right lung was also aspirated. Intermittently small boluses of suxamethonium chloride and midazolam were given and manual ventilation with supplemental oxygen was continued. Hemodynamic state and O2 saturation were continuously monitored. Repeated suctions were done to clear tracheo-bronchial tree as much as possible. Patient was extubated when she regained protective airway reflexes. Immediate SpO2 values dropped to as low as 90-95% and required Ventoline™ nebulization, suction of the orophyranx, supplemental oxygen by face mask and inj. hydrocortisone 100 mg I/V. Oxygen saturation improved after few minutes. Chest auscultation on the next morning showed bilateral air entry with a few scattered crackles on the left side posteriorly. A chest x-ray film showed re-expansion of the affected lung (Fig 2). Bronchodilator nebulization, suction of the oro-phyranx and chest physiotherapy was continued till she was able to maintain blood O2 saturation on room air. Next day patient was shifted to general ward. She was mobilized two days later with normal chest x-rays.
DISCUSSION
The respiratory secretions are derived from of the submucosal tracheobronchial glands and the epithelial goblet cells. These are a mixture of water, proteins, glycoprotein, lipids and salts. These have three important roles; (a) Clearance of the particulate matter deposited within respiratory tract (b) Have anti-bacterial substances and (c) Act as a humidifier of the inspired air. Respiratory mucus secretions are cleared by airflow and ciliary interactions, and are swallowed or cleared by coughing. Patients in ICU have a tendency to retain secretions and are at a risk of lobar, segmental or sub-segmental atelectasis, which may be complicated by pneumonia5. Treatment of atelectasis in ICU patients is focused on suctioning, physiotherapy and bronchoscopy. Chest physiotherapy consists of postural drainage, percussion and vibration. Recently, kinetic beds with percussion capability, therapy with mucolytic agents, hand held vibration devices and theravests have been added to the physiotherapists armamentarium. The occluded air passages may have to be directly visualized, cleared and lavaged by FOB. N-acetyl cystine instillation helps by chemically disintegrating the mucus plugs6. Koumbourlis and Kurland7 developed a technique for non-bronchoscopic, bronchoalveolar lavage performed via a sterile, disposable nasogastric tube in fifteen infants with diffuse lung interstitial disease/atelectasis, while they were intubated and ventilated. FOB was precluded because the small artificial airway did not permit passage of the broncho-scope. The procedure was well tolerated by all and they found radiographic evidence of improvement in two patients. Some other authors3,4 also advocate the use of insufflations. The idea of insufflations is based conceptually on the fact that while mucus plugs may lead to atelectasis, their removal may not be sufficient to correct the defect. They recommend the addition of high pressure to overcome the high critical opening pressure and the reduced lung compliance of the atelectatic lung. We suggest endobronchial intubation of the atelectatic lung, thick mucus liquefaction by N-acetyl cysteine instillation, postural drainage and chest percussion followed by insufflations; all put together. The procedure is convenient, requires available items and expertise: and is cost effective; although the patient is exposed to the risks of anesthetic drugs and ETT placement. This requires careful selection of drugs, hemodynamic/respiratory monitoring and expert anesthesiologist performing the procedure. Trained assistance is mandatory for placing the patient in different postures and performing other tasks. This procedure is a blind one and distal tracheo-bronchial tree cannot be accessed. In our case, we noted a drop in oxygen saturation after the procedure, which was due to the manipulation of airways and biological pulmonary response to N-acetyl cysteine6. It required supplementary oxygen inhalation, sitting posture and nebulization with bronchodilators.
Fig 1: Left lung collapse on plain x-ray
Fig 2: Lung re-expansion after the procedure
REFERENCES
- Mary Elizabeth Kreider and David A. Lipson. Bronchoscopy for Atelectasis in the ICU; A Case Report and Review of the Literature: Chest 2003;124;344-350.
- Weinstein HJ, Bone RC, Ruth WE. Pulmonary Lavage in patients treated with mechanical ventilation. Chest 1977;72:583-587.
- Bowen TE, Fishback ME, Green DC. Treatment of refractory atelectasis. Ann Thorac Surg 1974;18:584-589
- Millen JE, Vandree J, Glauser FL. Fiberoptic bronchoscopic balloon occlusion and re-expansion of refractory unilateral atelectasis. Crit Care Med 1978;6:50-55
- F Konard , T Schreiber, D Brecht- Kraus and M Georgeiff. Mucociliary transport in ICU patients. Chest 1994;105:237-241.
- Marino, Paul L. The Ventilator Dependent Patient. In; The ICU Book, 3rd ed. 2007. pp519-539.
- Koumbourlis, A.C. and Kurland, G. Non-bronchoscopic bronchoalveolar Lavage in mechanically ventilated infants: Technique, efficacy, and applications. Pediatric Pulmonology 1993;15:257-262.