Haidar Abbas, MD*, Zia Arshad MD**, Sulekha Saxena***, Jai Shree Bogra****
*Associate Professor; **Lecturer; ***MD Student; ****Professor & Head
Department of Anesthesiology, King George’s Medical University, Chowk, Lucknow U.P. (India).
Correspondence: Dr. Sulekha Saxena, MD Student, Department of Anesthesiology, King George’s Medical University, Chowk, Lucknow U.P. (India); Cell: 09359618480; E-mail: dr.sulekha2008@rediffmail.com
ABSTRACT
Airway management is one of the most important routine tasks performed by an anesthesiologist. Adept airway management is an essential skill for an anesthesiologist. Although practice guidelines and algorithms may help in such situations, but vigilance and a timely decision remain all important in such a situation. We encountered a patient with a rapidly enlarging subscapular mass due to which maintenance of supine position on the operating table for laryngoscopy and intubation was almost impossible. We had little options for airway management during general anesthesia in this patient. We present our method of successful management in this case and reiterate the role of different methods of correct positioning and intubation in such circumstances.
Key words: Airway management; Laryngoscopy; Difficult airway; Fibreoptic intubation; LMA
Citation: Abbas H, Arshad Z, Saxena S, Bogra JS. Airway management in a patient with a large mass in scapular region: A case report. Anaesth Pain & Intensive Care 2013;17(1):97-99
INTRODUCTION
Management of the difficult airway presents a great challenge for the anesthesiologist. Practice guidelines and algorithms are useful in such circumstances. However, the anesthesiologist’s judgment and vigilance remain the primary means to save airway management. There are few options for securing the airway during induction of general anesthesia in supine position, in a patient with a large mass on the back, which can be enumerated as follows. Placement of a proper wedge on the opposite side of the tumor to make the patient level in supine position without putting weight on the mass or to intubate patient in a lateral position may require some experience and skill. Fibreoptic intubation is the other option available but it is not usually available in the hospitals of the third world countries.
We present here a case of large mass in scapular region which posed anticipated difficulty in maintaining supine position for intubation. The authors tried an alternate scheme to intubate this patient. Patient was taken on the edge of the table with the mass hanging between the edge of the table and the arm rest. By this way we were able to maintain the desired position for laryngoscopy and intubation and the airway was managed successfully.
CASE REPORT
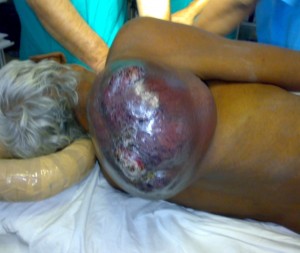
A 55 yr old male presented with a large mass in scapular region posted for wide local excision and split thickness grafting in the Department of Surgery, King George’s Medical University Hospital, Chowk, Lucknow (Figures 1-A & 1-B).
Figure 1-A: Large mass in right scapular region
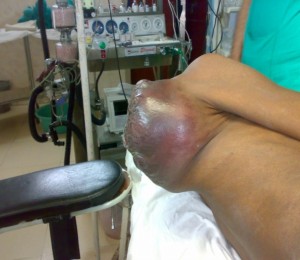
Figure 1-B: The lateral patient position on the edge of the table, before placing him supine
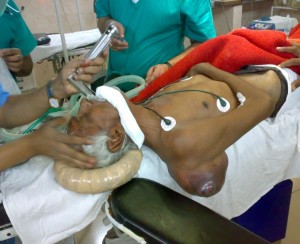
Figure 2: Patient on the edge of the table with mass hanging between the edge of the table and the arm rest
Patient was declared physically fit and ASA grade-1 on preanesthetic checkup. He had a short receding jaw and loose upper incisors, hence was anticipated to be a candidate for difficult laryngoscopy and intubation. Written consent was obtained and standard monitoring devices e.g. electrocardiogram, pulse oximetry, noninvasive blood pressure, and end-tidal carbon dioxide monitors, were attached to the patient in the operating room in the sitting position. An intravenous line with 18G cannula was passed.
The mass was assessed and it was felt that the supine position would be difficult to obtain by using large cushions and pillows. The lateral position was an option but intubation in this position was felt to be particularly difficult in view of his short receding jaw and loose upper incisors. Due to same reasons LMA insertion was also felt to be difficult in the lateral position. We placed the patient in the lateral position, facing towards opposite direction to his mass, on the extreme edge of the table. An arm rest was attached at the most cephaled end of the operating table. Then the patient was asked to roll over to a supine position so that the mass was hanging between the edge of the table and the arm rest (Figure 2). The right arm was supported over his chest and an assistant held the patient in position. Patient was given inj. glycopyrrolate 0.2 mg, inj. fentanyl 100mcg and inj. midazolam 1 mg IV. Anesthesia was induced with inj. propofol 120 mg and intubation was facilitated with inj succinyl choline 100 mg. Laryngoscopy was performed and endotracheal tube size 8.5 mm was placed successfully and secured. The patient was then paralyzed with inj. tracrium, ventilated and placed in lateral position for the surgery. He was extubated uneventfully at the end of the surgery in the lateral position.
DISCUSSION
Awake fibreoptic intubation remains the gold standard for anticipated difficult intubation.1 Blind nasal or oral intubation is a simple technique, but it is associated with two major drawbacks: infrequent success on the first pass, and increased trauma with repeated attempts. We could not risk precipitating complete airway obstruction that necessitated emergent cricothyrotomy.2-6 Also, insertion of the endotracheal tube via the nasal passage has a risk of nasal bleeding. This can result in an inability to visualize subsequent fibreoptic attempts due to both tissue edema and bleeding. Previous studies indicated fibreoptic nasotracheal intubations is associated with frequent failure (66% in some studies).6 However, there are reports of a greater success rate with this procedure, attributed to a well-organized approach, and expertise in flexible bronchoscopy.1,6 Unluckily, this procedure demands high level of expertise and skill for its success. The fiberscopes may not be available at all centers. Sitting fiberoptic bronchoscopic intubation can be life-saving, therefore, we suggest that anesthesiologists occasionally practice this technique so that it may be used when confronted with a patient requiring awake urgent intubation who cannot tolerate the supine position.
Elective tracheostomy using local anesthesia has been considered the ‘definitive’ modality of airway management in difficult situations such as deep neck infections6–8. Nevertheless, it may be difficult or impossible in advanced cases such as in our case because of the supine position needed for tracheostomy, or due to the anatomical distortion of the anterior neck. In our case, surgeons were reluctant to perform tracheostomy using local anesthesia without a secure airway1,5,8.
Intubation in lateral position is requires experience and skill. In our case, we felt it particularly difficult due to features of difficult airway present in this patient. Due to same reasons, the use of LMA or i-gel was thought to be impractical.9,10
We performed the laryngoscopy and intubation in the usual way, except that the position of the patient was adjusted according to the mass on the back to make patient supine to maintain suitable position for laryngoscopy and intubation.
REFERENCES
- Ovassapian A. Fiberoptic Endoscopy and the Difficult Airway. 2nd ed. Philadelphia: Lippincott-Raven Press, 1996
- Belmont MJ, Wax MK, DeSouza FN. The difficult airway: cardiopulmonary bypass—the ultimate solution. Head Neck 1998;20:266–9 [Medline]
- Hariprasad M, Smurthwaite GJ. Management of a known difficult airway in a morbidly obese patient with gross supraglottic oedema secondary to thyroid disease. Br J Anaesth 2002;89:927–30 [Medline] [Free Full Article] doi: 10.1093/bja/aef274
- Huitink JM, Balm AJ, Keijzer C, Buitelaar DR. Awake fibrecapnic intubation in head and neck cancer patients with difficult airways: new findings and refinements to the technique. Anaesthesia 2007;62:214–9 [Medline]
- Oka Y, Nishijima J, Azuma T, Inada K, Miyazaki S, Nakano H, et al. Blunt thyroid trauma with acute hemorrhage and respiratory distress. J Emerg Med 2007;32:381–5 [Medline]
- Ovassapian A, Tuncbilek M, Weitzel EK, Joshi CW. Airway management in adult patients with deep neck infections: a case series and review of the literature. Anesth Analg 2005;100:585–9 [Medline] [Free Full Article]
- Tsilchorozidou T, Vagropoulos I, Karagianidou C, Grigoriadis N. Huge intrathyroidal hematoma causing airway obstruction: a multidisciplinary challenge. Thyroid 2006;16:795–9 [Medline]
- Heidegger T, Gerig HJ. Algorithms for management of the difficult airway. Curr Opin Anaesthesiol 2004;17:483–4 [Medline]
- Ramachandran K, Kannan S. Laryngeal mask airway and the difficult airway. Curr Opin Anaesthesiol. 2004 Dec;17(6):491-3.
- Drolet P. Management of the anticipated difficult airway–a systematic approach: continuing Professional Development. Can J Anaesth. 2009 Sep;56(9):683-701. doi: 10.1007/s12630-009-9144-4. Epub 2009 Jul 28.