Tanvir Samra, MBBS, MD*, Ranvinder Kaur, MBBS, MD**, Lalita Choudhary, MBBS, MD***
*Assistant Professor
Post Graduate Institute of Medical Education and Research (PGIMER), Sector-12, Chandigarh (India);
**Associate Professor, ***Professor
Lady Hardinge Medical College, Shaheed Bhagat Singh Road, New Delhi 110001(India)
Correspondence: Dr Tanvir Samra, C-II/ 77, Moti Bagh 1, New Delhi-110021 (India); E-mail: drtanvirsamra@yahoo.co.in
ABSTRACT
Objectives: Brachial plexus block in combination with general anaesthesia is used for surgical correction of radial club hand. We carried out this retrospective study to assess the feasibility and efficacy of brachial plexus block in children with radial club hand. Intraoperative and postoperative analgesic requirements were the primary outcome measures analysed.
Methodology: We conducted a retrospective audit and collected data on the intraoperative and postoperative analgesic requirements in 24 patients anaesthetised for orthopedic treatment of this congenital deformity in our children’s hospital over a period of 5 years.
Results: Transarterial axillary block was administered to 8 patients; nerve stimulator guided supraclavicular block was used in 4 patients; and 12 were administered anesthesia without administration of brachial plexus block. Intraoperative additional supplementation of intravenous opioid was required in 12.5%, 50% and 75% of patients administered axillary block, supraclavicular block and no block (only general anesthesia) respectively. The mean time interval for administration of first dose of analgesic in postoperative period was 4.5, 3.6 and 0.75 hours respectively. Permanent diaphragmatic paralysis was reported in one patient with supraclavicular block. No complication was reported in the group with axillary block.
Conclusion: Supplementation of general anesthesia with transarterial axillary brachial plexus block provides adequate perioperative analgesia in children with radial club hand operated for centralisation of ulna.
Keywords: Radial club hand; Brachial plexus block; Analgesia;
Citation: Samra T, Kaur R, Choudhary L. Brachial plexus block for perioperative analgesia in children with radial club hand: a retrospective audit. Anaesth Pain & Intensive Care 2014;18(2):142-46.
INTRODUCTION
Congenital radial club hand is characterized by a varying degree of deficiency of the radius, carpal bones and the thumb.1 The patients present with radial deviation of the hand and marked shortening of the forearm. Orthopedic correction of radial club hand has progressed over the years from conservative management to aggressive surgical treatment. Soft tissue stretching by application of corrective cast/ Joshi’s External Stabilization System (JESS)distractor is done prior to definitive management i.e. centralization of the carpus over the distal end of the ulna.2
Brachial plexus block is a well established regional anesthetic technique for intraoperative anesthesia and postoperative analgesia in children.3 The presence of skeletal and neurovascular anatomical variations in patients with radial club hand have discouraged anesthesiologists from administering brachial plexus block in this subset of the population. But recent studies report the successful administration of nerve stimulator and ultrasound guided infraclavicular coracoid approach brachial plexus block in children with radial club hand.4,5
Availability of ultrasound is limited at majority of the hospitals in our country. Previous studies have documented the safety and efficacy of transarterial and perivascular techniques of axillary block in children.6,7 We carried out a retrospective study to assess the feasibility and efficacy of brachial plexus block in children with radial club hand. Intraoperative and postoperative analgesic requirements were the primary outcome measures analysed. The incidence of perioperative complications with axillary and supraclavicular techniques of brachial plexus block was the secondary outcome measure.
METHODOLOGY
All 24 children with radial club hand, operated for centralization of ulna by the same surgeon from 2008 to 2013 at our children’s hospital, were included in this retrospective analysis. Echocardiography, ultrasonography of abdomen and complete hemogram were ordered in the pre-anesthetic check up for all patients with radial club hand. According to our institutional protocol, all children are fasted 6 hours for solids, 4 hours for milk and 2 hours for water prior to an elective surgery. Oral premedication with syrup midazolam (0.5 mg/kg) was given 20-30 min prior to scheduled surgery to all children above one year of age as per the existing protocol. General anesthesia with or without brachial plexus block was administered for the surgery. Block failure was defined as a rise in heart rate (HR) and blood pressure (BP) of more than 20% of the basal after surgical incision. Supplemental doses of opioid and non-opioid analgesics used for rescue therapy were recorded.
Due to lack of a computerised data collection system in our hospital, we identified cases from the operating room registers and retrieved files from the medical records department. Patient data collected included demographic profiles, perioperative anesthetic management, hemodynamic profiles, the technique of brachial plexus block used, perioperative complications and perioperative analgesic consumption.
RESULTS
The patients of radial club hand included in the study had a median age of 1 year (range: 3 months-4 years) with a male to female ratio of 3:1. Patients were anesthetized for centralization of ulna (Figure 1). General anesthesia was induced in 8 patients with propofol (1-2 mg/kg), fentanyl (1 µg/kg) and vecuronium (0.1 mg/kg) and endotracheal tube introduced for IPPV. Maintenance was done with sevoflurane or halothane (MAC=1.2) in O2 andN2O. Transarterial axillary brachial plexus block was administered after endotracheal intubation with the arm abducted and held at 90 degrees where possible. After skin preparation with 0.5% chlorhexidine a 24G needle attached to an extension set and 10 ml syringe prefilled with the local anesthetic solution was inserted at an angle of 30 degree high in axilla parallel to axillary arterial pulsations. An assistant was scrubbed for injection of the drug while the principal anesthesiologist manipulated the needle. The needle was advanced a few millimetres further after aspiration of arterial blood and0.5 ml/kg of 0.25% of bupivacaine was injected after negative aspiration of blood posterior to the axillary artery. We used single injection technique and maintained digital pressure for 5 min distal to injection site to facilitate proximal spread of the local anesthetic and to minimise risk of hematoma formation at the arterial puncture site. An additional 1-2 ml of local anesthetic was infiltrated subcutaneously over the axillary sheath to block intercostobrachial and medial cutaneous nerve of the arm. Adequate intraoperative analgesia was recorded in 7 out of 8 (87.5%) patients; the remaining patients were supplemented with additional dose of fentanyl (1µg/kg). First dose of paracetamol was needed in the postoperative ward after mean duration of 4.5 hours. None of the patients developed any anesthetic or surgical complication.
Only 4 children were administered nerve stimulator guided supraclavicular brachial plexus block after induction before the muscle relaxants were administered. Motor response at either elbow or wrist (flexion, extension, supination, pronation) at a current of 0.5 mA was considered as end point for nerve stimulation and 0.5 ml/kg of 0.25% bupivacaine was injected. One of the children developed left diaphragmatic paralysis secondary to phrenic nerve injury which did not recover even after 2 years of follow up. Thus, this block in children with radial club hand was abandoned in our institute. Two out of four (50%) of these required one supplemental dose of 1µg/kg of fentanyl intraoperatively. The first dose of intravenous paracetamol (15 mg/kg) was required in them for pain relief in the post operative ward after a mean duration of 3.6 hours.
Surgical procedure was started 20 minutes after administration of the block and a tourniquet was used in all cases.
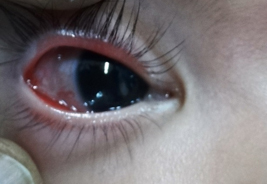
Associated cardiovascular anomalies included restricted ventricular septal defect in 2, small atrial septal defect in one and pulmonary artery hypertension in one child. Prior surgery for correction of tracheo-esophageal fistula and imperforate anus during neonatal period had been performed in two and one of the patients respectively. One of the children was diagnosed with Goldenhar syndrome (Figures 1 & 2). The mean surgical duration was 130.6 minutes.
Figure 1: Epibulbar dermoid in Godenhar syndrome
Figure 2: Preauricular tag and radial club hand
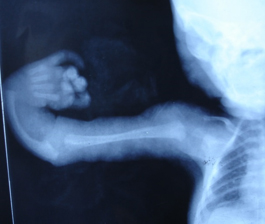
Figure 3: Absent radius on radiograph
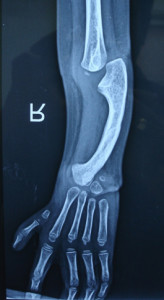
Figure 4: Absent radius on radiograph
No regional anesthesia was administered to 12 patients. The dose of fentanyl used in all these patients was 2 µg/kg at time of induction and 75% of them needed additional intraoperative supplementation of analgesia with 1µg/kg of fentanyl. First dose of paracetamol was needed in the postoperative ward after mean duration of 0.75 hours.
DISCUSSION
Radial club hand is a rare disorder with an incidence of 1:100,000, and literature on its anesthetic management is limited. The main focus of the preanesthetic check up is to rule out associated syndromes; TAR (thrombocytopenia and absent radius), VACTERL (vertebral anomalies, anal atresia, cardiac abnomalies, tracheoesophageal fistula, renal agenesis, and limb defects), Holt-Oram syndrome (autosomal dominant condition characterized by cardiac defects) and Fanconi’s anemia (autosomal recessive condition with aplastic anemia). Perioperative pain management is generally overlooked and brachial plexus block is thus usually not considered.
Regional anesthesia is challenging in this subset of patients due to the presence of various structural anomalies in the development of the upper limb. The radius bone is completely absent or hypoplastic (Figures 3 & 4). There is thus altered attachment of the muscles of the arm and forearm which is variable in each patient and cannot be predicted. Nerves originating from the brachial plexus have variable anatomical course. The radial nerve terminates at the elbow, the musculocutaneous nerve is absent and sensory nerve supply of radial aspect of the hand is by the median nerve. Ponde et al4 have described the successful use of nerve stimulator guided infraclavicular coracoid approach brachial plexus block with the use of fine twitches in the hand, at the wrist or in the surgical area or pronation–supination at a current of 0.5 mA as endpoints.Fused interphalangeal and metacarpophalangeal joints and hypoplastic or fibrosed muscles of forearm and hand preclude the demonstration of classical finger flexion and wrist flexion response with the use of nerve stimulators.Ultrasound (USG) guidance, however, improves the success rate of infraclavicular brachial plexus block.5
Our study highlights the feasibility and efficacy of transarterial axillary block in children operated for radial club hand. USG guided is the gold standard but it is not available in most of the centers. Axillary block has been safely used for perioperative analgesia in pediatric anesthesia6 and for orthopedic manipulations of forearm fractures in the pediatric emergency department.7
Tedore et al8 compared transarterial axillary block and the ultrasound-guided infraclavicular block for upper extremity surgery. They concluded that there was no significant difference in terms of adequacy for surgery and subjective postoperative dysesthesias. Ponde et al4,5 have used the infraclavicular brachial plexus block technique and we used transarterial approach. They reported success in 64% of patients administered block with nerve stimulator and 96% in those in which USG was used. We report a successful block in 87.5% which is close to both. Various adjuvants like clonidine and dexmedetomidine can be added to the block solution but we avoided their use due to their limited efficacy in pediatrics.9
We report left sided diaphragmatic paralysis in a 3 year old child secondary to supraclavicular block. Diagnosis was made after the child developed respiratory distressin the postoperative period. Incidence of phrenic nerve palsy with supraclavicular brachial plexus block is 50%10 and cases have been reported even with the use of USG guided block.11 However, very few case reports document the occurrence of persistent paralysis with interscalene block.12,13 Altered anatomy of upper limb and performance of block in an anesthetised child increase the chance of neural injury and could contribute to the occurrence of this complication in our case. Thus, we do not advocate the use of nerve stimulator guided supraclavicular block in children with radial club hand.
We used the single injection technique for axillary plexus block; the efficacy of which has been proved in previous studies.14 There was no complication with the transarterial axillary block. A previous study reported sensory paresthesia (0.2%) in the distribution of the ulnar nerve and musculocutaneous nerve, upper arm myalgias (0.3%), reflex sympathetic dystrophy (0.2%) and vascular complications like transient arterial spasm (1%), unintentional intravascular injection (0.2%), and small hematomas (0.2%) in patients administered brachial plexus block using the above mentioned technique.15
LIMITATIONS
Limitations of the study are due to its inherent design; inadequate information is obtained from a retrospective data collection and anesthetic and surgical technique cannot be standardised. However, uniformity in the technique of administration of general anesthesia and drug delivery in our audit is due to the existence of an institutional protocol for anesthetic management in our children’s hospital. By including cases operated by a single surgeon we standardised the surgical procedure also. Postoperative pain scores (FLACC, CHEOPS) could not be compared between the groups. A randomised controlled trial (RCT) with an adequate sample size needs to be conducted to compare the efficacy and safety of transarterial axillary brachial plexus block in this set of conditions.
CONCLUSION
Supplementation of general anesthesia with transarterial axillary brachial plexus block provides adequate perioperative analgesia in children with radial club hand operated for centralisation of ulna. This is the safest approach to block the brachial plexus in anesthetised children in which intraneural injections and nerve injuries cannot be ruled out due to lack of neurological assessment.
Conflict of interests: Nil
Financial disclosures: Nil
REFERENCES
- Goldberg MJ, Meyn M. The radial club hand. Orthop Clin North Am. 1976;7:341–59. [Pubmed]
- Management of radial club hand with gradual distraction followed by centralization. Indian J Orthop. 2009;43:292–300. [PubMed][Free Full Text]
- Tobias JD. Brachial plexus anaesthesia in children. Paed Anaesth 2001;11:265–275. [PubMed]
- Ponde V, Athani B, Thruppal S. Infraclavicular coracoid approach brachial plexus block for radial club hand repair. Paediatr Anaesth 2007;17:863–6. [PubMed]
- Ponde VC, Diwan S. Does Ultrasound Guidance Improve the Success Rate of Infraclavicular Brachial Plexus Block When Compared with Nerve Stimulation in Children with Radial Club Hands? Anesth Analg 2009;108:1967-70. [PubMed]
- Fisher WJ, Bingham RM, Hall R. Axillary brachial plexus block for perioperative analgesia in 250 children. Paediatr Anaesth 1999;9:435–438. [PubMed]
- Kriwanek KL, Wan J, Beaty JH, Pershad J. Axillary block for analgesia during manipulation of forearm fractures in the pediatric emergency department a prospective randomized comparative trial. J Pediatr Orthop. 2006;26:737-40. [PubMed]
- Tedore TR, YaDeau JT, Maalouf DB, Weiland AJ, Tong-Ngork S, Wukovits B, et al. Comparison of the transarterial axillary block and the ultrasound-guided infraclavicular block for upper extremity surgery: a prospective randomized trial. Reg Anesth Pain Med. 2009;34:361-5. [PubMed]
- Trifa M, Ben Khalifa S, Jendoubi A, Zribi N, Regaya T, Engelhardt T. Clonidine does not improve quality of ropivacaine axillary brachial plexus block in children. Paediatr Anaesth. 2012;22:425-9. [PubMed]
- Mak PH, Irwin MG, Ooi CG, Chow BF. Incidence of diaphragmatic paralysis following supraclavicular brachial plexus block and its effect on pulmonary function. Anaesthesia. 2001;56:352-6. [PubMed]
- Guirguis M, Karroum R, Abd-Elsayed AA, Mounir-Soliman L. Acute respiratory distress following ultrasound-guided supraclavicular block. Ochsner J. 2012;12:159-62. [PubMed][Free Full Text]
- Ediale KR, Myung CR, Neuman GG. Prolonged hemidiaphragmatic paralysis following interscalene brachial plexus block. J Clin Anesth. 2004;16:573-5. [PubMed]
- Robaux S, Bouaziz H, Boisseau N, Raucoules-Aimé M, Laxenaire MC; S.O.S. Regional Hot Line Service. Persistent phrenic nerve paralysis following interscalene brachial plexus block. Anesthesiology. 2001;95:1519-21. [PubMed][Free Full Text]
- Carre P, Joly A, Cluzel Field B, Wodey E, Lucas MM, Ecoffey C. Axillary block in children: single or multiple injection?. Paediatr Anaesth 2000;10:35-9. [PubMed]
- Stan TC, Krantz MA, Solomon DL, Poulos JG, Chaouki K. The incidence of neurovascular complications following axillary brachial plexus block using a transarterial approach. A prospective study of 1,000 consecutive patients. Reg Anesth. 1995;20:486-92. [Pubmed]
- Audenaert SM, Vickers H, Burgess RC. Axillary block for vascular insufficiency after repair of radial club hands in an infant. Anesthesiology. 1991;74:368-70. [PubMed][Free Full Text]
- Dalens B. Regional anesthesia in children. Anesth Analg 1989; 68:654-672. [PubMed]